Fibromyalgia
- What is fibromyalgia?
- What are the symptoms of fibromyalgia?
- What causes fibromyalgia?
- What are the risk factors for fibromyalgia?
- How is fibromyalgia diagnosed?
- How is fibromyalgia treated?
- What are the complications of fibromyalgia?
- When should you see a healthcare provider?
- What is the outlook for fibromyalgia?
- How to live better with fibromyalgia
- Featured fibromyalgia articles
Introduction
Around 4 million adults in the United States live with fibromyalgia. It’s the third most common musculoskeletal pain condition, trailing only low back pain and osteoarthritis (OA).
The chronic pain disorder was initially identified in the nineteenth century under the misnomer “fibrositis.” It was only in the mid-1970s that fibromyalgia’s tender points (areas of extreme tenderness on the body) were first accurately described. Still, much about this complex and sometimes debilitating condition remains cloaked in mystery.
Find out what researchers have learned about fibromyalgia, including what may cause it, who’s at risk for it, and how it’s diagnosed and treated. Learn which lifestyle strategies, complementary and alternative medicine (CAM) approaches, and natural remedies may be part of an effective fibromyalgia treatment plan. And find out how you can play an active role in managing fibromyalgia symptoms and living better with the condition.
What is fibromyalgia?

Fibromyalgia (also known as fibro) is classified as a rheumatic disorder, an umbrella term that includes arthritis and other conditions that affect bones, joints, and muscles. To be more accurate, fibromyalgia is a syndrome, or a group of symptoms that occur together, and is sometimes called fibromyalgia syndrome (FMS).
The hallmark symptoms are extreme tenderness in many areas of the body (referred to as tender points) and widespread pain in connective tissues, including muscles, ligaments, and tendons. (Pain in muscles is known as myalgia.) The pain and tenderness are often felt above and below the waist and on both sides of the body.
Fibromyalgia doesn’t cause the kind of tissue inflammation, damage, or deformity that may be seen in other rheumatic diseases such as osteoarthritis, rheumatoid arthritis (RA), and psoriatic arthritis (PsA). It doesn’t damage internal organs and isn’t life-threatening, although it can cause intense pain that may be incapacitating.
Who gets fibromyalgia?
People of all ages and racial and ethnic background experience fibromyalgia. These include children and adolescents. The risk goes up as people age, however, with fibromyalgia symptoms often appearing in middle age.
Around 6 to 15 percent of people in the U.S. live with the syndrome, with people assigned female at birth (AFAB) experiencing fibromyalgia up to five times more often than people assigned male at birth (AMAB). In fact, fibromyalgia is often the cause of generalized, musculoskeletal pain in people AFAB between the ages of 20 to 55 years.
People who have certain health conditions, including various mood disorders and other types of rheumatic disease, are also more likely to have fibro. In addition to osteoarthritis and rheumatoid arthritis, these include:
- Ankylosing spondylitis (a type of arthritis that causes inflammation in the joints and ligaments of the spine)
- Anxiety or depression
- Chronic back pain
- Irritable bowel syndrome (IBS, a group of symptoms that affect the intestines)
- Lupus (a group of chronic disorders in which the immune system mistakenly attacks healthy tissues and cells throughout the body)
What are the symptoms of fibromyalgia?
The type, intensity, and duration of fibromyalgia symptoms can vary for each person, with symptoms lasting days to months and sometimes years. Symptoms often come and go and fluctuate over time.
At times, fibromyalgia symptoms can flare up. That is, the number or intensity of symptoms may get worse. Other times, they can feel mild or go into remission. Remission describes a period when fibro symptoms aren’t present.
The most common fibromyalgia symptom is widespread pain
The central symptom of fibromyalgia is widespread (referred to as diffuse), chronic, and persistent muscle and soft tissue pain, despite the fact that no injuries or other abnormalities can be seen or felt in the affected areas. This fibro symptom has been described as a deep aching, burning, soreness, stiffness, or throbbing pain. People with fibro often report feeling like they always have the kind of muscle and body aches that come with the flu.
Mild to moderate pressure applied to tender points can trigger pain. Numbness, tingling, or unusual crawling sensations in the arms and legs may also occur. Joints can feel swollen, although joint inflammation can’t be seen or detected by touching or feeling the area.
Early in the course of the disease, fibro pain may only be felt in certain areas, most often the neck and shoulders. The pain gradually spreads to multiple areas of the body, including the middle and lower back, hips, arms, legs, and chest wall. And although pain may always be felt to some degree, fibromyalgia can be made worse by certain conditions or experiences such as:
- Anxiety or stress
- Exertion or exhaustion
- Exposure to cold or damp conditions
- Poor sleep
Other fibromyalgia pain symptoms
People with fibromyalgia may also experience other pain-related symptoms such as:
- Headaches, including migraines
- IBS symptoms, including frequent abdominal pain and episodes of diarrhea and/or constipation
- Interstitial cystitis/painful bladder syndrome, which causes bladder pain and urinary urgency (frequent and urgent need to urinate), although an infection isn’t present
- Temporomandibular joint (TMJ) syndrome, which can limit jaw movement and cause clicking or popping sounds when opening or closing the mouth along with headaches and pain within the facial or jaw muscles in or around the ear
Other fibromyalgia symptoms
Pain and tender points aren’t the only symptoms of fibromyalgia. People with fibro also experience:
- Anxiety
- Chronic, debilitating fatigue (possibly due to the close association between fibro and chronic fatigue syndrome, referred to as myalgic encephalomyelitis/chronic fatigue syndrome or ME/CFS)
- Depression
- Insomnia (problems falling or staying asleep or getting quality sleep)
- Sleep apnea (a condition marked by breathing that repeatedly stops and starts during sleep)
- Memory issues or trouble concentrating
- Stiffness upon waking that lasts more than an hour
Fibro fog symptoms
Fibro fog describes cognitive (brain-related) dysfunction that occurs with fibromyalgia. Also called brain fog, these symptoms may also occur with ME/CFS.
Fibromyalgia fog symptoms may include:
- Decreased alertness and reduced ability to think quickly and efficiently
- Forgetfulness and short-term memory problems, including remembering new information
- Inability to concentrate or multitask
- Trouble holding a conversation or recalling words and names
Fibro fog can greatly impact a person’s quality of life. In some cases, these fibromyalgia symptoms can be severe enough that some might mistake it for other conditions that affect the brain, such as attention deficit hyperactivity disorder (ADHD) or dementia.
What causes fibromyalgia?

Researchers are still working to unravel the mysteries of the syndrome, including what causes fibromyalgia. Much of what they know points to these possible origins:
Overly sensitive neurons (nerve cells)
It’s likely that people with fibromyalgia have a lower pain threshold, making them more sensitive to pain. In fact, the intensity of a stimulus needed to generate a pain response is nearly 50 percent lower in people with fibro, according to a 2022 review of studies published in Biomedicines. This is known as abnormal pain perception processing or signaling.
For people with fibro, the areas in the brain that process or regulate pain interpret painful sensations as more intense compared to people without fibro. This is referred to as hyperalgesia.
In addition to pain, people with fibromyalgia have a heightened sensitivity to other stimuli, including pressure, heat, and cold. This is called hyperalgesia allodynia.
Researchers believe these hyperalgesic responses involve issues with the way a part of the brain called the cortex processes signals. It’s also likely that the inability of the central nervous system (CNS) to control or manage pain and other stimuli via the spinal cord is also involved.
People with fibromyalgia may also have a cytokine imbalance. Cytokines are small proteins in the body, such as interleukin (IL) and interferon (IFN), that help regulate inflammation. People with fibro tend to have higher levels of cytokines such as IL-6 an IL-8 that promote inflammation and lower levels of those that decrease inflammation.
Neurotransmitter imbalance
Neurotransmitters are chemicals the nervous system uses to transmit, boost, and balance signals that travel from one neuron to another or from neurons to muscle. In essence, they’re the language of the nervous system, including the brain.
Neurotransmitters affect:
- Cognition (which includes perception, reasoning, and thinking)
- Communication
- Movement
- Sensation
Fibromyalgia symptoms have been linked with an imbalance in various neurotransmitters, contributing to pain sensitivity and a lower pain threshold. Certain “excitatory” neurotransmitters have the effect of causing neurons to send messages, while “inhibitory” neurotransmitters block messages from being passed along. These imbalances may include:
- Higher levels of excitatory neurotransmitters (such as glutamate and substance P)
- Lower levels of the inhibitory neurotransmitter serotonin and excitatory neurotransmitter norepinephrine
- Dopamine dysregulation, which involves reduced or diminished transmission of nerve signals by this neurotransmitter. (Note that dopamine can be excitatory or inhibitory, depending on the receptor it binds to.)
The brain also produces opiate-like hormones that the body uses as neurotransmitters to help reduce painful sensations. In people with fibro, these hormones may not function correctly.
These opioids produced by the body (called endogenous opioids) also help regulate other processes such as hunger, thirst, mood, and the body’s immune response. Examples of these opioids include dynorphin, enkephalins, and endorphins (the brain’s “feel-good” hormones).
Sleep disturbances and oxidative stress
Sleep disorders and disturbances are thought to play a role in fibromyalgia, especially issues with deep sleep. Also known as slow-wave sleep or delta sleep, deep sleep helps the body repair, restore, and optimize its many functions.
Slightly more than 92 percent of people with fibromyalgia experience sleep disorders, more than 50 percent of whom meet the criteria for insomnia. This lack of restful and restorative sleep is associated with higher pain levels in people with fibro.
That’s because sleep disturbances can interfere with the brain’s natural ability to control pain. This impairment not only has the effect of amplifying pain but it also impacts a person’s ability to cope emotionally with fibromyalgia symptoms.
People with fibro are more likely to experience what’s called “cognitive-emotional sensitization.” They tend to ruminate, have persistent negative thoughts, and think in terms of worst-case scenarios when distressing events occur (a mental habit known as “catastrophizing”).
Disrupted sleep can impact the amount of hormones the body releases. One such hormone is melatonin, which is produced by the brain’s pineal gland to regulate the body’s circadian rhythm and regulate the sleep-wake cycle.
The pineal gland boosts production of melatonin in response to darkness and stops making it in response to light. This facilitates the body’s transition to sleep and promotes quality rest.
People with fibromyalgia may have lower melatonin levels, which can intensify pain sensations, especially at night. In addition to regulating sleep, melatonin helps reduce inflammation, thereby decreasing the risk for chronic pain and pain that arises from issues with nerve signals (also known as neuropathic pain).
Melatonin also reduces oxidative stress, an imbalance between free radicals that damage the body and antioxidants that protect it. Research has shown that the hormone helps remove damaging free radicals.
Along with reducing inflammation and pain, lowering oxidative stress helps counter fatigue and anxiety. But disruptions in melatonin production contribute to poor sleep at night, sleepiness and fatigue during the day, and a heightened sense of pain. These, in turn, lead to less melatonin production, spawning a vicious cycle.
What are the risk factors for fibromyalgia?
People who have certain health conditions such as lupus and RA have a higher risk for fibromyalgia. People who are over 40 years old or assigned female at birth (AFAB) are also at elevated risk. Other possible risk factors for fibro include:
Family history and genes may raise the risk for fibromyalgia
Fibromyalgia often runs among closely related blood relatives. The authors of the review of studies published in Biomedicine note that first-degree blood relatives of people with fibromyalgia are 8.5 times more likely to have the condition themselves compared to the biological family ties of people with rheumatoid arthritis.
This strong association has led researchers to believe that genetic factors may predispose people to fibromyalgia. Although gene involvement hasn’t been definitively proven, certain gene mutations (variants) are thought to raise the risk for fibro.
Two that stand out include mutations in the adrenergic receptor gene and the D4 dopamine receptor gene. Other gene variants that may be involved in the development of fibromyalgia include:
- Cannabinoid receptor 1 (CNR1)
- Glutamate receptor, ionotropic, and alpha-amino-3-hydroxy-5-methyl-4-isoxazole propionate (AMPA 4) (GRIA4)
- Regulator of G-protein signaling 4 (RGS4)
- Trace amine-associated receptor 1 (TAAR1)
Environmental factors can increase the risk for fibromyalgia
Genetic predisposition interacts with environmental factors to raise the risk for fibromyalgia. In particular, early life experiences, long-term stress, and traumatic experiences can alter gene expression, the perception of pain, and the likelihood that fibromyalgia will develop.
Stress raises the risk of fibromyalgia
Stress can lead to fibromyalgia symptoms such as fatigue and insomnia. Studies have shown that people with fibro tend to have an especially active stress response, but why or how this occurs isn’t fully understood.
Some people with fibromyalgia may have higher levels of the stress hormone cortisol and higher cortisol levels have been tied to higher levels of pain upon awakening and up to an hour afterward.
Furthermore, the autonomic nervous system (ANS) in people with fibromyalgia may not function properly. The ANS consists of a network of nerves that regulate unconscious body processes such as blood pressure, heart rate, breathing, digestion, and sexual arousal.
The ANS usually adjusts these processes in response to stress. But when the ANS doesn’t function properly, pain and other associated fibromyalgia symptoms (such as higher blood pressure) may emerge as a result of stress.
Depression increases fibromyalgia risk (and vice versa)
A two-way relationship exists between fibromyalgia and depression. Depression raises the risk of fibro later in life and fibro raises the risk for depression.
People who experience persistent pain are more likely to experience depression compared to those without chronic pain. Moreover, people who experience chronic pain in multiple areas of the body have a higher risk of depression compared to people who experience pain in fewer areas.
The mechanisms that cause fibromyalgia and depression seem to be intertwined, although how or why either occurs or occur together isn’t exactly known. For instance, stress due to factors such as injury and traumatic experiences can trigger both fibro and depression symptoms.
The brain’s limbic system (which includes the amygdala, anterior cingulate cortex, anterior insular cortex, and hippocampus) is involved in regulating pain. It also plays a role in controlling the stress response and mood.
The amygdala in particular plays a central role in the way emotions are experienced and recalled. It’s more active when people are sad or depressed, and this increased activity can persist even after they overcome or recover from depression.
Inflammation in the central nervous system has also been tied to both conditions. Depression, fatigue, hyperalgesia, and fatigue have been linked with higher levels of IL-6. Increased levels of this cytokine have also been associated with more severe depression symptoms in people whose symptoms aren’t relieved by antidepressants.
Infections and illness raise fibromyalgia risk
For many people with fibromyalgia, their symptoms first developed after a serious illness or infection, such as the flu or Lyme disease. This is especially true if their symptoms were severe.
Trauma can increase fibromyalgia risk
Physical and emotional trauma may also raise the risk for fibromyalgia, especially when combined with other risk factors such as having a sleep disorder. This includes traumatic events involving:
- Childhood emotional abuse or neglect
- Physical assault or abuse
- Sexual assault or abuse
A serious injury or major surgery also qualifies as physical trauma.
How is fibromyalgia diagnosed?
There’s no gold standard for diagnosing fibromyalgia. It’s usually diagnosed based on a thorough discussion with a healthcare provider (HCP) about your symptoms and family and medical history along with a physical exam.
Tests to rule out other health conditions
Based on your symptoms, medical history, and the results of the physical exam, an HCP may also recommend specific tests to rule out other conditions that produce symptoms like those experienced with fibromyalgia. There’s no standard blood or imaging test that’s ordered in these situations. Tests are ordered on a case-by-case basis and depend on the condition suspected.
These include tests to confirm or rule out conditions such as:
- Autoimmune disease in which the immune system mistakenly attacks the body’s healthy cells, such as lupus
- Arthritis types such as ankylosing spondylitis, osteoarthritis, and rheumatoid arthritis
- Polymyalgia rheumatica (rheumatic disease that causes pain and stiffness around the neck, shoulder, and hip area)
- Thyroid disorders such as hypothyroidism (decreased thyroid gland activity, which causes fatigue, sleep disturbances, and muscle aches)
- Diseases that affect the muscles such as myositis (muscle inflammation, which causes muscle fatigue and weakness)
- Neurological disorders that affect the brain, spinal cord, and/or nerves such as multiple sclerosis (an autoimmune disease that affects the central nervous system)
Other fibromyalgia tests
Since fibro pain may be accompanied by other fibromyalgia symptoms, including sleep and mood disturbances, an HCP may also recommend the following:
- Referral to a licensed mental health provider for evaluation and treatment of mood disorders such as depression and anxiety
- Sleep study, if your HCP suspects that a sleep disorder such as sleep apnea or restless legs syndrome may be contributing to your fibromyalgia symptoms
Fibromyalgia diagnostic criteria
Along with having widespread pain, diagnostic criteria for fibromyalgia from the American College of Rheumatology (ACR) previously involved having at least 11 of 18 specific, excessively tender points, as determined by an HCP during a physical exam.
Updated ACR guidelines no longer require a tender point exam. Instead, widespread pain must be present for at least three months. The guidelines provide a numerical rating system to assess the extent and severity of fibro pain based on the person’s description.
To be diagnosed with fibromyalgia, a person must have pain in at least four of five areas such as the:
- Left upper region, including the arm, shoulder, or jaw
- Right upper region, including the arm, shoulder, or jaw
- Left lower region, including the buttock, hip, or leg
- Right lower region, including the buttock, hip, or leg
- Axial region, which includes the abdomen, chest, back, or neck
Along with pain, an HCP will also consider other potential fibromyalgia symptoms (such as fatigue or fibro fog) prior to making the diagnosis.
How is fibromyalgia treated?
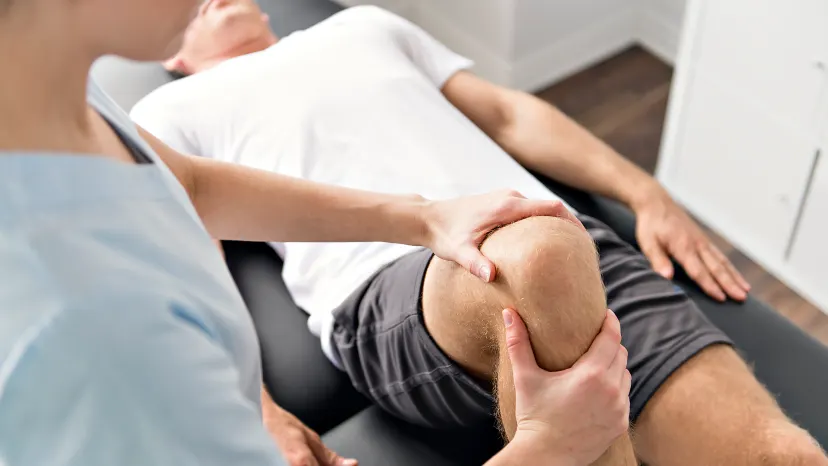
Although a cure hasn’t been discovered or developed yet, there are effective fibromyalgia treatment options to help alleviate pain and other symptoms. Because of the complexity of fibromyalgia symptoms and flare-up patterns, a fibro treatment plan is usually tailored to the person’s individual needs and involves a holistic and comprehensive approach to care.
The core of such a plan involves a strong partnership and trust between the treating HCP and the patient. This is particularly important because it may take time and trial and error to find the most effective treatment regimen.
The fibromyalgia treatment plan must also be practical and realistic. A person’s ability and willingness to carry out each aspect of the plan are also factored into it, as it may involve taking medicines, adding in complementary and alternative medicine (CAM) therapies, and making long-term lifestyle changes.
A primary care HCP—such as a family or internal medicine doctor or nurse practitioner—may refer you to a fibromyalgia specialist such as a rheumatologist or neurologist. They will work with you to develop a personalized care plan, which may change over time based on the type and severity of your symptoms, the treatment side effects experienced, cost concerns, and your treatment preferences.
Fibromyalgia medication
The type and severity of your fibromyalgia symptoms will determine which medicines to include in your treatment plan. Medicines that target chemicals and areas in the brain and spinal cord involved in pain processing have been shown to be effective at relieving fibromyalgia symptoms. These include antidepressants usually used to treat depression and anticonvulsants used to treat seizure disorders such as epilepsy.
In contrast, corticosteroids and nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, may be less effective at treating the full range of fibromyalgia symptoms. That’s because NSAIDs and steroids decrease tissue inflammation to lessen pain, and fibromyalgia doesn’t inflame tissue.
Therefore, your HCP may recommend a variety of medicines to treat your fibromyalgia symptoms. Note that some of these are prescribed off-label, meaning they’re not approved by the U.S. Food and Drug Administration (FDA) to treat fibromyalgia, as indicated on the drug’s FDA-approved package label or insert.
Off-label prescribing is a common and legal practice, but a patient’s HCP must take a thorough health history, conduct a comprehensive physical exam, and assess all the benefits and risks to the person carefully before prescribing a medication in this way. Only three medications are currently approved by the FDA to treat fibromyalgia: the antidepressants duloxetine and milnacipran and the anticonvulsant (antiseizure drug) pregabalin.
Antidepressants used for fibromyalgia
Antidepressants used to treat chronic pain, depression, and other fibromyalgia symptoms include:
Serotonin-norepinephrine reuptake inhibitors (SNRIs): Also called dual-reuptake inhibitors, duloxetine and milnacipran are SNRI antidepressants approved by the FDA to treat fibromyalgia. They work by keeping the neurotransmitters serotonin and norepinephrine from being pulled back into the neurons that released them—a process called reabsorption or reuptake. Doing so increases the levels of these neurotransmitters in the brain.
Tricyclic antidepressants (TCAs): These include amitriptyline and nortriptyline. They work by preventing the synapses (nerve endings) that release serotonin and norepinephrine from reabsorbing them back into their tissue, thereby raising levels of these neurotransmitters in the brain. They also block the action of the excitatory neurotransmitter acetylcholine. Low-dose TCAs taken before bedtime may help ease pain and improve sleep.
Selective serotonin-reuptake inhibitors (SSRIs): Although not as effective at relieving fibro pain as SNRIs or TCAs, SSRIs such as fluoxetine and paroxetine may also help relieve fibromyalgia pain and other symptoms. They work by blocking reuptake of serotonin to boost levels of the neurotransmitter in the brain.
Anticonvulsants used for fibromyalgia
Pregabalin is an anticonvulsant approved by the FDA to treat fibromyalgia. Anticonvulsants such as pregabalin and gabapentin also support better sleep and relieve fibro pain, especially nerve pain. They work by blocking the activity of neurons involved in pain transmission. Other anticonvulsants used for fibromyalgia treatment include lacosamide and levetiracetam.
Analgesics to relieve fibromyalgia pain
Analgesics such as the over-the-counter pain medicine acetaminophen may be added to your fibromyalgia treatment plan to provide short-term pain relief. An opioid analgesic called tramadol can also provide temporary relief of fibro pain. Tramadol is weaker than other medicines in this drug class and carries less risk of opioid addiction.
In general, long-term treatment of fibromyalgia with opioids isn’t recommended. Despite being potent pain relievers, opioids carry significant risks and side effects.
They’ve also shown very little benefit in treating fibromyalgia. Opioids can also make fibro worse, according to some evidence. This is called opioid-induced hyperalgesia. Therefore, if a short course of opioids is prescribed for you, it’s important to take them safely using the smallest dose needed to relieve pain for the shortest duration possible.
Muscle relaxants used for fibromyalgia
The muscle relaxant cyclobenzaprine has a chemical structure similar to TCAs. Although it doesn’t treat depression like a TCA, it can promote relaxation and support deeper sleep, thereby reducing sensitivity to pain. Tizanidine is another muscle relaxant commonly used to treat fibromyalgia symptoms.
Other medications for fibromyalgia treatment
Other medicines may also be prescribed to treat specific fibromyalgia symptoms or associated health conditions. For instance, a benzodiazepine (benzo) such as alprazolam may be used to treat anxiety.
Physical and occupational therapy for fibromyalgia
A physical therapist can work with you to build strength, flexibility, and endurance. They’ll show you how to move, stretch, and perform exercises safely, properly, and in ways that don’t aggravate your fibromyalgia symptoms.
An occupational therapist can teach you how to adjust your environment and work with adaptive tools that allow you to perform daily activities at home, work, and other settings without straining or stressing your body further.
Physiotherapy for fibromyalgia
A physiotherapist incorporates movement and exercise, manual therapies (such as massage), and education as part of a fibromyalgia treatment plan. The goal is to ease pain and other fibro symptoms, as well as improve physical function and quality of life.
Examples of physiotherapy approaches used to treat and manage fibromyalgia include:
Exercise for fibromyalgia
Exercise is one of the most effective ways to manage fibromyalgia, according to the ACR. Some people may believe that moving less will help them prevent fibro flare-ups, but leading a sedentary lifestyle can actually worsen fibromyalgia symptoms.
Studies have shown that regular exercise can ease fibro pain and fatigue and reduce reliance on medications for symptom relief. It can also improve sleep, boost mood, and support a more positive mindset when it comes to overall health.
Physiotherapists work with clients to design and carry out a personalized exercise plan. This often includes aerobic exercise and resistance or flexibility training performed at a moderate intensity to improve pain and sensitivity caused by fibro and to bolster physical functioning, cardiovascular fitness, and muscle strength and flexibility.
Manual therapy and massage for fibromyalgia
Manual therapy involves manipulation of soft and connective tissue (such as skin, fat, muscle, and joints) using rhythmic pressure to prevent and ease pain and to develop, maintain, rehabilitate, or increase physical function. In addition to helping alleviate fibromyalgia symptoms, manual therapies may help ease the symptoms of associated musculoskeletal, physical, and psychological disorders such as:
Around 75 percent of people with fibromyalgia use massage therapy to help ease symptoms. Though there’s limited scientific evidence to support its use for fibro symptom relief, many people believe in its potential benefits.
For some, it can improve fibromyalgia symptoms such as pain, anxiety, depression, and sleep disturbances. A physiotherapist is likely to recommend moderate over more aggressive forms of massage to provide maximum benefit without aggravating fibro pain.
Most types of massage have been shown to improve the quality of life in people with fibromyalgia, according to a 2022 review of studies published in Frontiers in Physiology. These include manual and massage therapies such as:
Myofascial release: A physiotherapist might employ myofascial release techniques during massage sessions. Myofascial tissue (or fascia) is the tough membrane that connects, supports, and wraps around the body’s muscles.
Fascia is usually flexible, stretchy, and able to move easily. But injury, trauma, or disease can affect these characteristics, making fascia tighter and more rigid and resulting in pain and loss of motion.
Also called myofascial trigger point therapy, this manual therapy uses gentle massage to release myofascial pain and tightness. It may also help with stiffness and may ease anxiety, depression, and fatigue. Overall, it’s uncertain whether and to what extent the technique can help with fibromyalgia symptoms since the scientific evidence to date has been limited.
Manual lymphatic drainage: Also called lymphatic drainage massage, this manual therapy helps relieve swelling caused by lymph collecting in tissues due to illness, disease, or injury. Lymph is the fluid left behind after the cardiovascular system (the heart and blood vessels) transports blood to the body’s tissues and organs.
The lymphatic system usually collects lymph and returns it to the heart via its network of lymph nodes and vessels. When this process is blocked, lymph collects in tissues and causes painful swelling.
Manual lymphatic drainage employs gentle massage to move lymph to the lymph nodes, thereby easing swelling and pain. Studies suggest it may be better than massage at easing stiffness and depression, as well as improving quality of life in some people with fibromyalgia.
Shiatsu: Originating in Japan, this massage method involves using the hands, thumbs, and other body parts to apply direct pressure on various points or meridians (also known as energy channels) in the body. Unlike other forms of massage, shiatsu is performed through loose clothing and doesn’t use oils.
It’s been described as a modified form of acupressure, which involves pressing specific points on the body (called acupuncture points) to improve the flow of blood and lymph and lessen tension and fatigue.
Studies have shown that shiatsu helps improve fatigue, sleep, and quality of life in some people with fibromyalgia. It also helps lessen pain while increasing the threshold for pain caused by pressure.
Self-management skills for fibromyalgia
Physiotherapists empower people with fibromyalgia to take control and responsibility for their own health. Fibro’s chronic nature often leads people to view the syndrome and its consequences in a negative way.
For example, patients may catastrophize the disease and view it as a life-threatening illness. But physiotherapists can help clients reframe this perspective in a more realistic way while still recognizing that fibromyalgia symptoms are real, legitimate, and not a figment of their imagination (as some people may believe).
Physiotherapists provide expert guidance on how to better control fibromyalgia symptoms and take measures to address poor lifestyle habits (such as poor diet or lack of exercise) that exacerbate fibro. They encourage people to actively participate in their fibromyalgia treatment plan.
In addition to providing information about fibromyalgia, treatment and management strategies, and expected outcomes, a physiotherapist also works with the patient to come up with or modify a written fibromyalgia action plan. Teaching people with fibromyalgia these self-management skills has been shown to improve fibromyalgia symptoms and increase adoption and adherence to the treatment plan.
Cognitive behavioral therapy to treat fibromyalgia
Cognitive behavioral therapy is a structured form of talk therapy. With the help of a mental health provider, people can unlearn negative thoughts and behaviors and learn to adopt healthier ways of thinking and behaving.
Multiple research reviews have found CBT to be an effective way to manage chronic pain. It’s been widely and successfully used to treat numerous other mental and physical health conditions in addition to depression and anxiety—from obsessive-compulsive disorder (OCD), post-traumatic stress disorder (PTSD), and eating disorders such as bulimia to IBS, insomnia, and migraines.
CBT is the psychological therapeutic approach of choice when it comes to fibromyalgia treatment. It combines educational components with opportunities to practice new thoughts and behaviors at home and during therapy sessions.
The practice is grounded in the notion that what people think or believe is the way they tend to behave. In other words, changing one’s mindset can yield lasting changes in behavior.
Techniques such as cognitive reframing (also called cognitive restructuring) are often practiced during CBT sessions. It involves changing thoughts, behaviors, and habits that create and intensify issues. The process allows people to discover, challenge, and alter or replace their negative, unrealistic, or unhelpful thoughts. This gives them the opportunity to cultivate more positive and useful thoughts and behavior patterns.
Other CBT techniques used for people with fibromyalgia might include setting goals for better long-term functioning and breaking these down into action steps. The approach helps reduce depression associated with fibro and improve pain by teaching people more effective ways of self-managing fibromyalgia symptoms.
Hyperbaric oxygen therapy to treat fibromyalgia pain
Growing evidence supports the use of hyperbaric oxygen therapy (HBOT) for treatment of fibromyalgia, according to a 2023 review and analysis of studies published in BMJ Open. HBOT involves intermittently breathing 100 percent oxygen in a pressure chamber.
Doing so helps raise the partial pressure of oxygen in alveoli—the tiny, balloon-shaped air sacs located at the end of the lung’s branching tubes. More oxygen is then delivered to the body’s tissues. As a result, HBOT reduces the activity of substances that cause inflammation and helps correct brain activities, potentially reducing fibromyalgia symptoms such as pain.
Complementary and alternative medicine for fibromyalgia
Some people turn to complementary and alternative medicine (CAM) to ease their fibromyalgia symptoms. They may do so because of the high cost of or limited access to conventional fibromyalgia treatments along with concerns that they may not work well enough.
In most instances, it’s best to integrate these CAM approaches into your care plan rather than use them to replace standard treatments. Talk with an HCP before making changes to your fibromyalgia treatment plan to be sure a CAM approach is safe for your symptoms and other health conditions you may have.
Acupuncture
Acupuncture is an ancient Traditional Chinese Medicine practice that’s been used for over 4,000 years. During the procedure, an acupuncturist inserts thin, sterile needles into certain points on the body. They may then use a specific hand manipulation technique or they may connect the needles to an electrical stimulation device to support the flow of Qi (vital life force energy), thereby improving health.
Multiple studies point to the benefits of acupuncture for fibromyalgia. It’s been shown to relieve fibro pain, ease depression, and improve quality of life.
Balneotherapy to alleviate fibromyalgia pain
Balneotherapy is a form of body immersion therapy used for centuries. It involves bathing in thermal mineral waters from natural sources such as peloids (mud or clay prepared and used for therapeutic purposes). How balneotherapy works isn’t fully understood, but it likely has to do with the effects of thermal stimulation, mineral bath salt composition, and the physical and chemical properties of peloids.
Studies have shown that balneotherapy decreases levels of interleukin 1, leukotriene B4, and prostaglandin E2. These are substances in the body associated with pain and inflammation. Moreover, combining aerobic exercise with balneotherapy reduces fibromyalgia pain more effectively than either intervention alone.
Mindfulness meditation to ease fibromyalgia symptoms
Mindfulness is a form of meditation that involves focusing on the present moment with acceptance, curiosity, and openness. It entails cultivating a nonjudgmental awareness of your body’s sensations, thoughts, consciousness, and environment.
The goal of mindfulness is to become less reactive toward unpleasant symptoms and experiences. It builds self-awareness while helping you regulate your thoughts and emotions, which can help you better manage stress associated with fibromyalgia.
Tai Chi for fibromyalgia
Tai chi is an ancient meditative practice rooted in TCM. It integrates deep breathing and relaxation techniques with a series of gentle and controlled postures.
The goal is to unify your behavior with elements of the mind, body, and spirit to increase inner harmony and to calm the mind and body. Practiced routinely, tai chi also helps increase flexibility and strengthen the soft tissues of the body to improve fibromyalgia symptoms and quality of life.
Yoga for fibromyalgia
Various types of yoga are often recommended for pain relief, stress management, and relaxation. Studies have shown that practicing yoga helps reduce fibromyalgia symptoms such as pain, fatigue, and anxiety. Like many forms of exercise, yoga stimulates the release of endorphins to help ease pain while helping to boost your mood and lift your spirits.
Natural remedies for fibromyalgia
Some people with fibromyalgia integrate natural remedies into their fibromyalgia treatment plan. These might include herbs, extracts, vitamins, minerals (such as zinc and iron), and other CAM options.
Be sure to talk with an HCP before adding any of these natural remedies to your treatment plan. An HCP can help you determine how much and how often to take these supplements and whether any of them interact with medicines you currently take.
Examples of some supplements shown to ease certain fibro symptoms include:
Coenzyme Q10 (CoQ10)
CoQ10 is an antioxidant naturally produced in the body. It helps convert food into energy and protects your brain, heart, and muscles. CoQ10 has been shown to reduce fibromyalgia pain and oxidative stress.
The pain reduction observed in some research was greater when the antioxidant was combined in a supplement that included vitamin D, magnesium, alpha-lipoic acid (another antioxidant), and tryptophan (an amino acid). Using CoQ10 along with pregabalin also helps reduce fibromyalgia symptoms such as pain and anxiety better than using pregabalin alone.
Selenium
Selenium levels are often low in people with fibromyalgia. The trace element helps regulate the function of the nervous system, including transmission of nerve impulses. It also helps with shoring up the body’s antioxidant defenses and helps reduce pain intensity, possibly due to its effects on the pain-processing pathways of the brain.
Folic acid
Folic acid is form of vitamin B that also has antioxidant properties. It supports immune system function and may help regulate pain sensation in people with fibromyalgia.
Capsaicin
This is the substance that makes chili peppers hot. Capsaicin may ease nerve pain caused by fibromyalgia. Products made with this ingredient come in various forms, including gels, creams, patches, and pills. Capsaicin is considered safe to use for fibromyalgia, but be aware that it can cause itching or burning in the area where you apply the product.
What are the complications of fibromyalgia?
Fibromyalgia symptoms such as chronic pain can sometimes feel debilitating. They can greatly impact patients’ quality of life and possibly lead to other complications, such as a higher likelihood of:
- Rheumatic disease: People with fibro are more likely to have other types of rheumatic disease such as OA, RA, and lupus.
- Hospitalization: The Centers for Disease Control and Prevention (CDC) notes that people with fibromyalgia are twice as likely to be admitted to the hospital for care compared to people without the condition.
- Depression: The rates of depression in adults with fibro are three times higher compared to adults without it.
- Death from suicide and injuries: People with fibromyalgia have higher rates of death due to suicide and associated injuries.
How does fibromyalgia affect pregnancy?
Many people assigned female at birth (AFAB) with fibromyalgia are able to conceive without issues. Some experience symptom improvement during pregnancy while others experience symptom flare-ups, especially during the first few months of pregnancy.
Various fibromyalgia symptoms may also feel worse for pregnant people with fibro. These include pregnancy symptoms also common to fibro, such as fatigue, mood shifts, and stress.
If you’re pregnant or trying to conceive, be sure to talk with your HCP about any needed adjustments to your fibromyalgia treatment plan. Doing so can help ensure a safe and healthy pregnancy.
When should you see a healthcare provider?

Be sure to let your HCP know if you’re experiencing new or unusual symptoms, as your fibromyalgia treatment plan may need to be adjusted. If your fibro symptoms are severe or growing worse despite following your treatment plan, be sure to talk with your HCP right away.
These include new or worsening symptoms such as severe headaches or migraines, fibro fog, and sleep issues. If you’re feeling depressed or have thoughts of suicide, reach out for immediate help from your HCP.
You can also reach a crisis counselor at the 988 Suicide & Crisis Lifeline by calling or texting 988. Call, text, or chat online with a 988 Lifeline counselor any time of day, any day of the week.
What is the outlook for fibromyalgia?
Although fibro doesn’t usually damage the body, it’s a chronic condition that requires consistent, lifelong care to be properly managed. Work with your HCP to develop and adjust your treatment plan as needed. This, coupled with a positive attitude, can help you better manage your condition and possibly prevent fibromyalgia symptom flare-ups.
Can fibromyalgia be prevented?
Because the exact cause of fibromyalgia has yet to be determined, there’s no scientifically proven way to prevent the condition at this time. But taking steps to support your overall health may help lower your risk for the disease and lessen the severity of symptoms.
Will fibromyalgia get better with time?
Most people continue to experience fibromyalgia symptoms throughout their lives, although they may come and go and differ in type and severity. How and to what degree fibro affects day-to-day function and mental and physical well-being varies from person to person.
Working closely with your HCP to understand and manage your fibromyalgia symptoms, learning and using helpful coping techniques, and having a strong social support system can greatly improve your short- and long-term quality of life.
How to live better with fibromyalgia
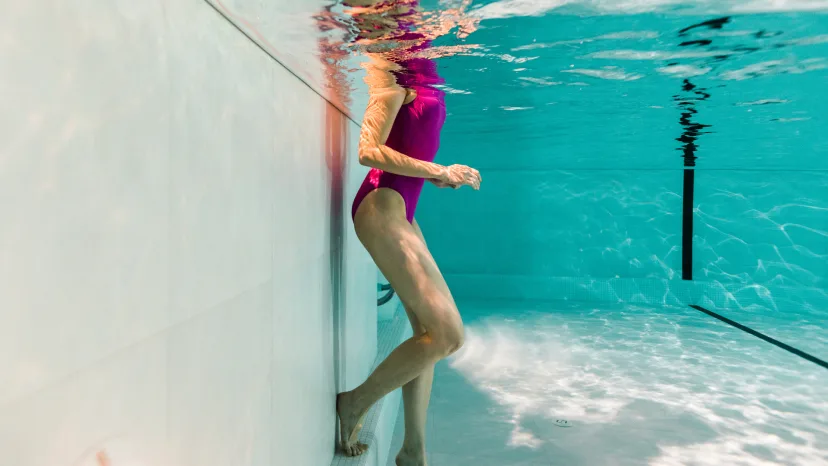
Self-care plays a central role in your fibromyalgia treatment plan. Effective self-care strategies often involve lifestyle measures such as:
Exercises for fibromyalgia
Being physically active can lessen fibromyalgia symptoms and support a better quality of life, as well as physical and psychological well-being. This includes reducing anxiety, depression, and sleep issues, as well as easing pain by stimulating the release of serotonin and the body’s natural opiates, such as endorphins.
Workout plans for people with fibromyalgia often entail water- or land-based aerobic exercises such as swimming laps or brisk walking performed three times a week coupled with twice-weekly strength or resistance training. In addition to lowering pain and stiffness and improving mood and quality of life, these activities help improve endurance, muscle strength, and physical function and mobility along with reducing the risk of falls—especially in older adults with fibromyalgia.
The authors of a 2022 review and analysis of studies published in Scientific Reports note that the amount and intensity of activity must be tailored to each person’s fitness level, experience performing each activity type, and fibromyalgia symptoms. The authors also note that people with fibro can initiate activity slightly below their usual physical capacity, with the goal of gradually building to moderate levels of intensity to prevent pain or keep it from getting worse.
Water workouts for fibromyalgia
In addition to swimming, water-based workouts might include cardio activities performed in waist-deep or chest-level water. These place less stress on the joints and help improve pain, stiffness, and muscle strength.
The effects of these exercises have been tied to the warmth and buoyancy of the water. For instance, aquatic physiotherapy is generally performed in water that’s heated to around 90-degrees Fahrenheit. While working out in water, the brain’s sensory stimuli compete with painful stimuli, thereby blocking and reducing pain sensations.
Water-based workout performed in warmer temperatures also cause vasodilation (opening of blood vessels). This helps increase blood flow, which helps relax stiff and tight muscles.
Dance workouts for fibromyalgia
In addition to its many physical benefits, dance promotes psychosocial benefits that improve mood and self-confidence. It’s been shown to substantially reduce the effects of depression and anxiety, and it gives people with fibromyalgia more confidence in their ability to cope with their illness. The improvements in fitness, conditioning, and physical appearance also help boost people’s confidence—especially people who are overweight or obese.
Many genres of dance can confer these physical and psychosocial benefits, from ballet to ballroom and hip-hop to hula. These can be structured dances such as those performed with choreography for a performance or competition.
Dance can also simply emphasize creativity and freedom of movement. These can be unstructured dances such as those performed for the purpose of dance therapy, or they can involve dance improvisation.
Studies have shown that dancing for 60 minutes or longer tends to provide the greatest benefit on pain management in people with chronic pain, with those approaching the general physical activity recommendation of 150 minutes of physical activity each week experiencing even greater reductions in pain.
Fibromyalgia diet
There’s no uniform approach to eating healthy with fibromyalgia. Although some studies have shown promising results, there’s no conclusive evidence to support any specific diet for fibromyalgia. More rigorous research is needed to make definitive recommendations.
That said, a 2021 review of studies published in the International Journal of Environmental Research and Public Health notes that a mostly plant-based diet may help reduce pain and other fibromyalgia symptoms in addition to improving markers of health such as total cholesterol and body weight.
The benefits of a plant-based eating style, such as a vegan or vegetarian diet, stem from high intake of nutrient-rich plant foods such as fruits, vegetables, nuts, seeds, legumes, and whole grains. A plant-based eating pattern can boost levels of fiber, vitamins (such as C and E), minerals, and antioxidants such as resveratrol. These nutrients may help ease pain and other fibromyalgia symptoms by counteracting the oxidative stress placed on the body due to poor nutrition.
Support for a plant-based diet has garnered further support from a 2023 review of studies published in Nutrients, which also found that this eating style helps significantly reduce pain in people with fibromyalgia compared to anti-inflammatory diets such as a gluten-free diet. The authors of the review posit that weight loss associated with following a plant-based eating pattern may also contribute to the reduction in pain. In contrast, a gluten-free diet may not result in weight loss.
Studies also show that avoiding certain foods may benefit some people with fibromyalgia. This includes foods that contain excitotoxins, which are food additives such as monosodium glutamate (MSG) found in processed foods such as packaged soup mixes and the sugar substitute aspartame, which is often added to drinks such as diet sodas or used as a standalone sugar substitute.
These chemical food additives can overstimulate neurons, which increases sensitivity to pain, oxidative stress, and the severity of fibromyalgia symptoms. On the other hand, a diet rich in omega-3 fatty acids may help prevent excess stimulation caused by excitotoxins. Foods rich in these healthy fats include fish and seeds and nuts, such as walnuts and flaxseeds.
Stress management and fibromyalgia
Find healthy ways to manage stress. Try not to overexert yourself both physically and emotionally—at home, work, or in other areas of your life.
This might mean planning out your day from a practical standpoint and sticking to your plan, as well as setting limits and simply saying no to invitations or obligations when necessary. It can also mean trying out various stress-management techniques to see which one best fits your needs and interests.
You can try listening to relaxing music to bring peace and comfort to your mind and spirit. If you feel up to it, crank up the beat and dance to release those feel-good endorphins.
Spend quality time with close friends and loved ones, put your phone down (or better yet, turn it off), and take a moment to simply enjoy each and every moment together. Or cuddle with your beloved pet to dial down your stress level.
Sleep hygiene and fibromyalgia
Restful and restorative sleep is essential to preventing fibromyalgia symptoms and flare-ups. Try winding your mind and body down at least a few hours before bedtime.
This might include turning off your phone, laptop, TV, and other light-emitting devices and taking a warm, relaxing bath or shower to soothe your senses. Or try some gentle stretches before climbing into bed.
If you can, try to go to sleep and wake up within an hour of your usual bedtime and wake time, even on weekends and days off. This helps support your body’s natural circadian rhythms and sleep-wake cycle, thereby helping to keep fibromyalgia symptoms at bay.
Featured fibromyalgia articles

988 Suicide & Crisis Lifeline. Talk to Someone Now. Substance Abuse and Mental Health Services Administration. Accessed May 15, 2023.
Almutairi NM, Hilal FM, Bashawyah A, et al. Efficacy of acupuncture, intravenous lidocaine, and diet in the management of patients with fibromyalgia: A systematic review and network meta-analysis. Healthcare (Basel). 2022;10(7):1176.
American College of Rheumatology. Fibromyalgia. Last updated February 2023.
Antunes MD, Marques AP. The role of physiotherapy in fibromyalgia: Current and future perspectives. Front Physiol. 2022;13:968292
Arthritis Foundation. Fibro Fog. Accessed May 9, 2023.
Assavarittirong C, Samborski W, Grygiel-Górniak B. Oxidative stress in fibromyalgia: From pathology to treatment. Oxid Med Cell Longev. 2022;2022:1582432.
Bhargava J, Hurley JA. Fibromyalgia. StatPearls [Internet]. Last updated Oct 10, 2022.
Chen X, You J, Ma H, Zhou M, Huang C. Efficacy and safety of hyperbaric oxygen therapy for fibromyalgia: A systematic review and meta-analysis. BMJ Open. 2023;13(1):e062322.
Cleveland Clinic. Cognitive Behavioral Therapy. Last reviewed August 4, 2022.
Cleveland Clinic. Fibromyalgia. Last updated December 1, 2022.
Cleveland Clinic. Lymphatic Drainage Massage. Last reviewed September 2, 2021.
Cleveland Clinic. Myofascial Release Therapy. Last updated August 15, 2022.
Cohen-Biton L, Buskila D, Nissanholtz-Gannot R. Review of fibromyalgia (FM) Syndrome Treatments. Int J Environ Res Public Health. 2022;19(19):12106.
Couto N, Monteiro D, Cid L, Bento T. Effect of different types of exercise in adult subjects with fibromyalgia: A systematic review and meta-analysis of randomised clinical trials. Sci Rep. 2022;12(1):10391.
Dalal DS. Fibromyalgia. Merck Manual Consumer Version. Last reviewed/updated April 2022.
Dalal DS. Fibromyalgia. Merck Manual Professional Version. Last reviewed/updated March 2022.
Goldenberg DL. Patient education: Fibromyalgia (Beyond the Basics). Last updated February 18, 2022.
Gyorfi M, Rupp A, Abd-Elsayed A. Fibromyalgia pathophysiology. Biomedicines. 2022;10(12):3070.
Harvard Health Publishing. What Causes Depression? Published January 10, 2022.
Hickman B, Pourkazemi F, Pebdani RN, Hiller CE, Fong Yan A. Dance for chronic pain conditions: A systematic review. Pain Med. 2022;23(12):2022-2041.
Islam Z, D'Silva A, Raman M, Nasser Y. The role of mind body interventions in the treatment of irritable bowel syndrome and fibromyalgia. Front Psychiatry. 2022;13:1076763.
Kocyigit BF, Sagtaganov Z, Yessirkepov M, Akyol A. Assessment of complementary and alternative medicine methods in the management of ankylosing spondylitis, rheumatoid arthritis, and fibromyalgia syndrome. Rheumatol Int. 2023;43(4):617-625.
Leça S, Tavares I. Research in mindfulness interventions for patients with fibromyalgia: A critical review. Front Integr Neurosci. 2022;16:920271.
Maddox EK, Massoni SC, Hoffart CM, Takata Y. Dietary effects on pain symptoms in patients with fibromyalgia syndrome: Systematic review and future directions. Nutrients. 2023;15(3):716.
Nadal-Nicolás Y, Miralles-Amorós L, Martínez-Olcina M, Sánchez-Ortega M, Mora J, Martínez-Rodríguez A. Vegetarian and vegan diet in fibromyalgia: A systematic review. Int J Environ Res Public Health. 2021;18(9):4955.
National Institute of Arthritis and Musculoskeletal and Skin Diseases. Fibromyalgia Basics. Last reviewed June 2021.
Office on Women’s Health. Fibromyalgia. U.S. Department of Health & Human Services. Last updated February 22, 2021.
Pelava CJ. Shiatsu. University of Minnesota. Accessed May 12, 2023.
Ruschak I, Montesó-Curto P, Rosselló L, Aguilar Martín C, Sánchez-Montesó L, Toussaint L. Fibromyalgia syndrome pain in men and women: A scoping review. Healthcare (Basel). 2023;11(2):223.
Stanford Medicine. Fibromyalgia. Accessed May 9, 2023.
Yepez D, Grandes XA, Talanki Manjunatha R, Habib S, Sangaraju SL. Fibromyalgia and depression: A literature review of their shared aspects. Cureus. 2022;14(5):e24909.
Zhang KD, Wang LY, Zhang ZH, et al. Effect of exercise interventions on health-related quality of life in patients with fibromyalgia syndrome: A systematic review and network meta-analysis. J Pain Res. 2022;15:3639-3656.





