Psoriatic arthritis
- What is psoriatic arthritis?
- Psoriatic arthritis symptoms
- What are the causes and risk factors for psoriatic arthritis?
- What are the different types of psoriatic arthritis?
- How is psoriatic arthritis diagnosed?
- Which psoriatic arthritis treatments ease symptoms?
- What are the stages of psoriatic arthritis?
- Living well with psoriatic arthritis
- Featured psoriatic arthritis articles
Introduction
Approximately 7.5 million adults in the United States have psoriasis, a chronic skin condition that can cause thick, painful patches to grow on the skin. Among psoriasis patients in the U.S. and Europe, as many as 30 percent will eventually develop psoriatic arthritis, a condition marked by achy and swollen joints. Though some patients may experience psoriatic arthritis first, the majority of those with both conditions develop this form of arthritis several years after the first skin symptoms of psoriasis appear.
Psoriatic arthritis can cause symptoms that affect your everyday life, even beyond the joint pain that is the hallmark of the condition. The good news is that there are a variety of psoriatic arthritis treatments and lifestyle strategies that can help you live well with the condition.
Learn more about the symptoms, causes, and risk factors of psoriatic arthritis, as well as ways your healthcare provider (HCP) can diagnose the condition and help you manage it over the long run.
What is psoriatic arthritis?
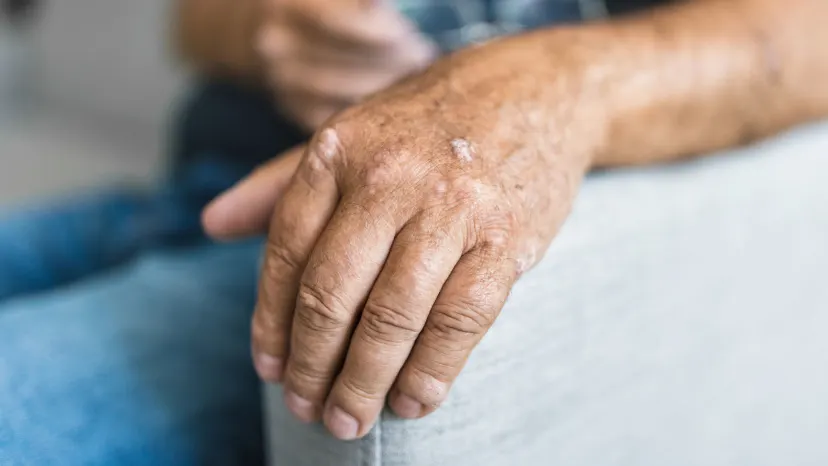
Psoriatic arthritis is a chronic joint disease closely linked with psoriasis. Together, both conditions constitute psoriatic disease.
Psoriatic arthritis is considered an inflammatory arthritis because the joint damage it may cause results from long-term, sometimes severe inflammation.
Is psoriatic arthritis an autoimmune disease?
Like psoriasis, psoriatic arthritis is an autoimmune disease. Your immune system ordinarily works to defend your body from viruses, bacteria, and other invaders. But when you have an autoimmune disease, your immune system attacks healthy tissue and cells by mistake.
Psoriatic arthritis symptoms

Having psoriatic arthritis can follow unpredictable cycles. These may involve intense symptoms called flare-ups or flares followed by periods of remission when you have mild symptoms or none at all. Psoriatic arthritis symptoms may appear and evolve in varied ways as well.
If you have both psoriasis and psoriatic arthritis, your symptoms of each condition may not coincide. For example, you may have severe psoriasis but mild psoriatic arthritis, or vice versa.
The symptoms you experience depend on the type of psoriatic arthritis you have. Symptom severity is also often influenced by how many joints are affected. Mild psoriatic arthritis involves up to four joints while moderate to severe forms of the disease impact more than four joints.
Common psoriatic arthritis symptoms include the following:
Joint symptoms of psoriatic arthritis
Psoriatic arthritis symptoms involving your joints may include:
- Painful, stiff, and swollen joints (often in your fingers, toes, wrists, ankles, knees, and spine, including your neck and lower back)
- Redness or discoloration, inflammation, or heat in the tissues around your joints
- Fingers and/or toes that take on the appearance of sausages (known as dactylitis)
- Joint damage that leads to deformity in fingers and/or toes
- Trouble moving or bending your joints and reduced joint range of motion
Skin symptoms of psoriatic arthritis
The condition can also affect your skin health. Skin-related psoriatic arthritis symptoms include:
- Dry, inflamed, and noncontagious skin patches called plaques that are often covered with silvery-white scales with raised edges
- A sensation of itching or burning on your skin
- Nails that crumble, appear pitted and discolored, or lift from their nail beds
Other psoriatic arthritis symptoms
Psoriatic arthritis can cause fatigue, a symptom reported by 78 percent of people with the condition in a 2022 study published in The Journal of Rheumatology that looked at people in the U.S. and Europe.
You may also experience extra-articular manifestations (EAMs). Although these don’t affect your bones, muscles, or joints, they are related to having psoriatic arthritis. These include psoriasis, psoriasis plaques, and psoriatic nail disease, as well as:
- Dry eye disease
- Conjunctivitis, commonly called pink eye (swelling and infection of the thin outer layer of your eye called the conjunctiva)
- Uveitis (swelling of your middle eye layer called the uvea)
Conditions related to psoriatic arthritis
Psoriatic arthritis can also raise your risk for several related health conditions, including
- Cerebrovascular diseases, such as stroke
- Coronary artery disease
- Eczema
- Fibromyalgia
- Hyperlipidemia (high cholesterol)
- Hypertension (high blood pressure)
- Inflammatory bowel diseases such Crohn’s disease and ulcerative colitis
- Liver disease
- Metabolic disorders such as diabetes and metabolic syndrome
- Mood disorders such as anxiety and depression
- Obesity
- Osteoporosis
- Peripheral artery disease (also called peripheral vascular disease)
When to contact your healthcare provider
If you notice any new or worsening psoriatic arthritis symptoms, EAMs, or symptoms of conditions related to psoriatic arthritis, it’s important to be evaluated by an HCP. Left untreated, these conditions can severely impair and damage your joints and affect other aspects of your health.
In some cases, your HCP may refer you to a rheumatologist. These HCPs specialize in diagnosing and treating diseases that affect your joints, muscles, and bones.
What are the causes and risk factors for psoriatic arthritis?
Scientists are working to uncover what causes psoriatic arthritis. Although the exact mechanism isn’t fully known, certain factors are likely at play.
The main risk factor for psoriatic arthritis is having psoriasis. Around 20 to 30 percent of people with psoriasis also develop psoriatic arthritis, according to a 2022 study published in the Journal of the American Academy of Dermatology. Some sources note that psoriatic arthritis may be underdiagnosed, which means these numbers may even be higher.
Moreover, around 72 percent of the time, people develop the skin disease an average of 7 to 8 years before psoriatic arthritis, according to a 2022 review of studies published in Psoriasis.
Other possible causes and risk factors include the following:
How your genes influence your psoriatic arthritis risk
Around 33 to 50 percent of people with psoriatic arthritis have at least one first-degree blood relative who also has it, suggesting that genes play a role.
There’s also a link between genetics and psoriasis, but the genes involved with this skin condition and psoriatic arthritis aren’t always the same.
How your immune system affects your psoriatic arthritis risk
When you have psoriatic arthritis, your immune system attacks healthy cells in your joints and skin. People who develop the autoimmune disease also have high levels of immune system proteins that promote inflammation called cytokines.
How environmental factors increase your psoriatic arthritis risk
Environmental factors that can raise your risk of developing psoriatic arthritis or trigger flares of existing disease include:
- Illness and infection: These include infections such as strep throat and HIV.
- Joint injury or trauma: Injuring your joints and bones increases the risk of psoriatic arthritis. This is known as the Koebner phenomenon.
- Obesity: Being overweight or obese can increase joint inflammation by raising the level of inflammatory cytokines in your blood.
- Smoking and drinking alcohol: Smoking tobacco and drinking too much alcohol can boost inflammation, especially if you have psoriasis, too.
What are the different types of psoriatic arthritis?
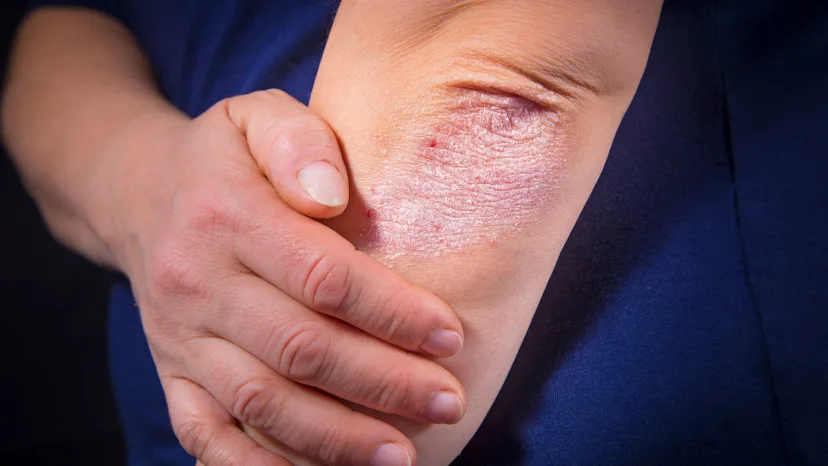
Psoriatic arthritis is often divided into five main types based on the patterns they follow.
What is asymmetric psoriatic arthritis?
Asymmetric psoriatic arthritis is the most common form of psoriatic arthritis. At least 60 percent of people with psoriatic arthritis have this type at first.
The defining characteristic of asymmetric psoriatic arthritis is that it can affect one joint (monoarthritis) or multiple joints (oligoarthritis) on one side of your body. Asymmetric arthritis often impacts fewer than five small or large joints.
For example, the condition can cause the entire length of your digits (fingers and toes) to become swollen and inflamed, a condition known medically as dactylitis or commonly as “sausage digit” or “sausage finger.” When your psoriatic arthritis is asymmetrical, only the digits on one side of your body tend to be affected.
What is symmetric psoriatic arthritis?
Symmetric psoriatic arthritis affects five or more joints on both sides of your body. The small joints in your fingers and toes are most often affected.
This subtype produces symptoms similar to those of rheumatoid arthritis (RA). While RA tends to affect the same general areas on each side of your body, with symmetric psoriatic arthritis, the affected joints may not be the same on each side of the body. For example, symmetric psoriatic arthritis can impact the joints near the base of your toes on one foot and the joints closer to the tips of your toes on the opposite foot.
What is distal psoriatic arthritis?
This psoriatic arthritis type causes swelling and stiffness for the most part in your distal interphalangeal (DIP) joints, those closest to the ends of your fingers and toes, which is why this type is also called DIP predominant psoriatic arthritis.
Distal psoriatic arthritis is associated with psoriatic nail disease (PND), a condition which causes nails to become warped, pitted, and discolored. They may also crumble or crack or separate from their nail beds, a condition called onycholysis.
What is spondylitis psoriatic arthritis?
This psoriatic arthritis type affects the joints of your spine, including your sacroiliac (SI) joints. Your SI joints connect your sacrum, which sits at the lowest part of your spine above your tailbone, to your pelvis. These joints support your body weight when you are standing.
Spondylitis psoriatic arthritis can cause pain, inflammation, and stiffness anywhere along your spine, from your neck to your lower back. It can also cause symptoms in other joints, including those in the arms, legs, hands, feet, and hips.
What is psoriatic arthritis mutilans?
Psoriatic arthritis mutilans (PAM) is the most severe and rare subtype. The exact prevalence is unclear, but research suggests that anywhere from 1 to 21 percent of people with psoriatic arthritis also have PAM. “Mutilans” comes from the Latin word for “mutilated” or “maimed,” and the subtype is so named because the disease deforms and destroys affected joints.
The condition most often affects the small joints in the wrists, hands, and feet. Less commonly, PAM can involve the spine. The subsequent damage to the spine can change your posture and impact mobility.
PAM causes enthesitis, or severe inflammation of the tendons and ligaments where they connect to bone, which can lead to the loss of connective tissue and bone. As a result, fingers or toes may retract or shorten. This phenomenon, known as digital telescoping or “opera-glass finger,” can cause deformation and loss of function in the affected joint. The joints may also become fused together, affecting your ability to move them; this condition is known as ankylosis.
Arthritis mutilans may also occur in people with rheumatoid arthritis.
How is psoriatic arthritis diagnosed?

Your HCP will start by talking with you about your psoriatic arthritis symptoms and your personal and family medical history. They may also give you certain tests to help confirm a diagnosis, including:
- Physical exam: Your HCP will look for swollen and painful joints, patterns common to various types of psoriatic arthritis, and related skin, nail, or eye problems.
- X-rays: This imaging test can spot injuries or damage to your joints.
- Computed tomography (CT), magnetic resonance imaging (MRI), ultrasound, or bone scan: If your HCP needs to look at your joints or bones in greater detail, they may also order one of these scans to assess for joint, soft-tissue, or bone loss and damage that can’t be seen with an X-ray.
- Lab tests: Your HCP may evaluate samples of your blood or fluids from your joints to check inflammation levels. These tests also help rule out other types of arthritis that produce signs and symptoms similar to psoriatic arthritis, such as gout, joint pain and swelling caused by Lyme disease, or RA.
- Skin biopsy: In some cases, your HCP may need to perform a skin biopsy to confirm or rule out psoriatic disease, which entails removing and analyzing a small sample of your skin.
Which psoriatic arthritis treatments ease symptoms?

Your psoriatic arthritis treatment plan depends on your treatment preferences and the severity of your condition.
Lifestyle approaches to treat psoriatic arthritis
Treatment may begin or coincide with non-drug, lifestyle therapies, which may include:
- Cold or heat therapy: Your HCP might recommend you apply a cold pack on the affected joint for 10 minutes at a time to lessen inflammation and alleviate pain. Moist heat, such as a warm bath or a paraffin bath for your hands and feet, can also help relieve stiff and sore joints and muscles.
- Occupational therapy or physical therapy: These can help ease pain, improve joint mobility, and make it easier to perform daily tasks.
- Exercises for psoriatic arthritis: These can keep your joints flexible, strengthen your muscles and bones, and help you lose excess weight. Just be sure to take breaks and get adequate rest if you experience pain.
- Smoking cessation: Quitting tobacco for good lets you eliminate this preventable risk factor for psoriatic arthritis.
- Weight management: If you are overweight or obese, losing just 10 percent of your body weight may improve the effectiveness of treatment.
- Acupuncture: The traditional Chinese medicine approach involves placing thin needles along pressure points to treat various health issues, including pain.
If you experience flare-ups or your condition gets worse, your HCP can recommend or prescribe therapies and medicines to help manage your psoriatic arthritis symptoms. These may include:
Nonsteroidal anti-inflammatory drugs (NSAIDs) for psoriatic arthritis
Your HCP may recommend an over-the-counter (OTC) nonsteroidal anti-inflammatory drug (NSAID) or prescribe a stronger version than those sold OTC. NSAIDs such as ibuprofen and naproxen help ease pain and swelling but they don’t slow disease progress. You may only need NSAIDs when your joints feel swollen or painful and can stop using them when you feel better.
Corticosteroid injections to ease psoriatic arthritis inflammation
Your HCP can inject steroid medicine (also called corticosteroids or glucocorticoids) into the affected joint. Oral steroids aren’t usually recommended for people with psoriatic arthritis because they can cause a severe form of psoriasis. They can also raise your risk of side effects such as weight gain, diabetes, and weak bones.
Disease-modifying antirheumatic drugs (DMARDs) for psoriatic arthritis
If non-drug therapies and NSAIDs don’t help, your HCP may prescribe a DMARD for your psoriatic arthritis symptoms. These drugs stop inflammation at the source by targeting specific immune system cells or their proteins. This can help slow and possibly prevent further joint damage.
DMARDs include:
- Traditional DMARDs: These are immunosuppressant drugs, which work to dampen the effects of your entire immune system. Immunosuppressants were initially developed to prevent organ transplant rejection, but some are now used to treat cancer and autoimmune diseases such as psoriatic arthritis, RA, and lupus. Traditional DMARDs may be used alone or in combination with biologic DMARDs or corticosteroids to ease symptoms.
- Biologic DMARDs (also called biologic response modifiers): These usually work more quickly than traditional DMARDs and are used to treat severe psoriatic arthritis. Biologics selectively block certain immune pathways and interfere with cytokine production. The three biologic DMARD classes include tumor necrosis factor alpha inhibitors, interleukin inhibitors, and selective co-stimulation modulators.
- Targeted synthetic DMARDs: These impede various steps of the body’s inflammatory process and can be used if traditional DMARDs or biologics don’t help.
Topical psoriatic arthritis treatments
Topical treatments are applied directly to the skin to help treat symptoms such as plaques and nail changes. They come in OTC and prescription-strength creams, ointments, and other products.
Topicals may include ingredients such as anthralin, coal tar, salicylic acid, steroid or nonsteroid medicines, and vitamin A.
Newer oral medications for psoriatic arthritis
Oral medications, such as apremilast, can also help ease inflammation. Apremilast works by inhibiting the action of the phosphodiesterase 4 enzyme in your body to reduce swelling and pain. This might be an option if you can’t or don’t want to use DMARDs or biologics to manage your psoriatic arthritis.
Phototherapy for psoriatic arthritis
During phototherapy (also called light therapy), your skin is exposed to ultraviolet (UV) light. A device equipped with light-emitting diodes provides controlled doses of UV light at varying wavelengths and strengths.
UV light consists of UVA and UVB wavelengths. Excessive exposure to either type is dangerous, as they are both linked to skin cancer, but moderate amounts of UVB causes changes to your skin and immune cells. This can:
- Alleviate itching
- Reduce inflammatory cytokines
- Stimulate production of vitamin D, which bolsters the skin’s barrier function and helps slow the rapid growth of skin cells that occurs with psoriatic disease
- Suppress your body’s autoimmune response
Although light therapy often involves the use of UVB lights due to their effectiveness and safety profile, UVA therapy may also be used in combination with the light-sensitizing agent psoralen in a treatment called PUVA.
Surgery to repair or replace joints
Surgery may be used to repair joints damaged by psoriatic arthritis. In some cases, joint replacement surgery may be needed. This involves removing the diseased joint and replacing it with an artificial prosthesis made of metal and plastic.
What are the stages of psoriatic arthritis?
Each patient’s experience with psoriatic arthritis is unique and disease progression is not inevitable. In many cases, receiving prompt and effective treatment—particularly with medications to reduce overactivity of the immune system, as needed—can ease symptoms and reduce the risk of long-term health issues.
For many patients, though, the disease progress in stages. Where you are in the course of your journey will likely influence your psoriatic arthritis treatment plan.
Early-stage or mild psoriatic arthritis
During the early stages of the disease, you tend to have mild psoriatic arthritis symptoms such as joint swelling and limited range of motion in the affected joint. You may also notice some skin plaques breaking out at the same time as these joint symptoms. Your HCP may recommend or prescribe NSAIDs during this stage.
Middle-stage or moderate psoriatic arthritis
If you have more moderate symptoms, your HCP will likely prescribe more advanced psoriatic arthritis treatments to ease your symptoms and help keep your condition from getting worse. Biologics and DMARDs are more likely to be used during this middle stage.
Late-stage or severe psoriatic arthritis
If you experience the late stage of the disease, you may have more profound disability as your joints, bones, and other connective tissue may have sustained severe damage. This can include joint deformity, erosion, or fusion. Your HCP will work with you to modify your psoriatic arthritis treatment plan as needed to manage your symptoms, repair or replace joints, and prevent further complications.
Be sure to consult with your HCP if any of your psoriatic arthritis treatments become less effective or stop working.
Living well with psoriatic arthritis
Psoriatic arthritis can take a toll on your physical and emotional health. Many of the challenges that come from living with psoriatic disease can affect other parts of your life—from your personal, family, and work obligations to your intimate and social relationships and everyday mental health.
These approaches can complement your treatment plan and help you feel more balanced in your experience with psoriatic arthritis:
- Ease stress. Find healthy ways to manage your stress with relaxation techniques such as deep breathing, meditation, or listening to relaxing music.
- Seek treatment for anxiety and depression. This might involve individual counseling with a licensed mental health provider, group counseling with other people living with psoriatic disease, and talking with your HCP to see if medications to treat mental health issues might be right for you.
- Stay active. Try low-impact workouts such as swimming, yoga, or cycling. Start slowly and pace the intensity and speed of your workouts to be easy on your joints. Rest and take breaks as needed to keep from straining or injuring your joints or triggering a flare-up.
- Manage your weight. Excess weight can place strain on your joints and fuel inflammation. Losing weight can reduce inflammation and improve the way your body responds to treatment.
Diet for psoriatic arthritis
Eating healthy, nourishing foods when you have psoriatic disease can help you shed excess weight and give you more energy. While there’s no specific diet for psoriatic arthritis, some foods and eating patterns (such as the Mediterranean diet) can help ease inflammation and support gut health, which can support your treatment plan.
Beneficial foods include:
- Colorful vegetables like broccoli, Brussels sprouts, cauliflower, and kale
- Fatty fish like mackerel, salmon, sardines, trout, and tuna
- Lean proteins, such as skinless chicken
- Nuts and seeds such as flaxseeds, pumpkin seeds, and walnuts
- Olive oil, which has phenolic compounds that counter inflammation, such as oleocanthal
Featured psoriatic arthritis articles

American Academy of Dermatology Association. Psoriatic Arthritis: Overview. Last updated November 28, 2022.
American College of Rheumatology. Psoriatic Arthritis. Last updated December 2021.
Arthritis Foundation. Beyond Joints: How Psoriatic Arthritis Affects the Body. Last reviewed April 21, 2021.
Arthritis Foundation. Light Therapy for Psoriatic Arthritis. Accessed March 13, 2023.
Arthritis Foundation. Psoriatic Arthritis. Accessed March 10, 2023.
FitzGerald O, Ogdie A, Chandran V, et al. Psoriatic arthritis. Nat Rev Dis Primers. 2021;7, (59).
Gladman DD, Ritchlin C. Patient Education: Psoriatic Arthritis (Beyond the Basics). Last updated March 24, 2022.
Gisondi P, Bellinato F, Maurelli M, et al. Reducing the Risk of Developing Psoriatic Arthritis in Patients with Psoriasis. Psoriasis (Auckl). 2022;12:213-220. Published 2022 Aug 10.
Gossec L, Walsh JA, Michaud K, et al. Effect of fatigue on health-related quality of life and work productivity in psoriatic arthritis: Findings from a real-world survey. J Rheumatol. 2022;49(11):1221-1228.
Hackett S, Coates LC. Outcome measures in psoriatic arthritis: Where next? Musculoskeletal Care. 2022;20 Suppl 1(Suppl 1):S22-S31.
Jin JQ, Elhage KG, Spencer RK, et al. Mendelian randomization studies in psoriasis and psoriatic arthritis: A systematic review. J Invest Dermatol. 2023;S0022-202X(22)02844-5.
Katsimbri P, Korakas E, Kountouri A, et al. the effect of antioxidant and anti-inflammatory capacity of diet on psoriasis and psoriatic arthritis phenotype: Nutrition as therapeutic tool? Antioxidants. 2021;10(2):157.
Krakowski P, Gerkowicz A, Pietrzak A, et al. Psoriatic arthritis—New perspectives. Arch Med Sci. 2019;15(3):580-589.
Kumthekar A, Ogdie A. Obesity and psoriatic arthritis: A narrative review. Rheumatol Ther. 2020;7:447–456.
Mayo Clinic. Psoriatic Arthritis. Last updated October 2, 2021.
Mistegård J, Gudbjornsson B, Lindqvist U, et al. Comorbidities in a cohort of 66 patients with psoriatic arthritis mutilans–Results from the Nordic PAM study. Front Med). 2021;8:629741.
National Institute of Arthritis and Musculoskeletal and Skin Diseases. Psoriatic Arthritis. Last reviewed March 2021.
Novelli L, Lubrano E, Venerito V, et al. Extra-articular manifestations and comorbidities in psoriatic disease: A journey into the immunologic crosstalk. Front Med. 2021;8:737079.
Ogdie A, Harrison RW, McLean RR, et al. Prospective cohort study of psoriatic arthritis risk in patients with psoriasis in a real-world psoriasis registry. J Am Acad Dermatol. 2022;87(6):1303-1311.
National Psoriasis Foundation. About Psoriatic Arthritis. Last updated June 2, 2022.
National Psoriasis Foundation. Rheumatologist. Accessed March 13, 2023.
National Library of Medicine. Psoriatic Arthritis. MedlinePlus
Pittam B, Gupta S, Harrison NL, Robertson S, Hughes DM, Zhao SS. Prevalence of extra-articular manifestations in psoriatic arthritis: A systematic review and meta-analysis. Rheumatology. 2020;59(9):2199-2206.
Rath L. Everything You Need to Know About Immunosuppressants. Arthritis Foundation. Published December 8, 2022.
Tiwari V, Brent LH. Psoriatic Arthritis. StatPearls [Internet]. Last updated August 11, 2022.
Watson S. Treatment options for Psoriatic Arthritis. Arthritis Foundation. Published June 17, 2022.
DMARDS. Arthritis Foundation. Accessed March 22, 2023.
Zhao SS, Bellou E, Verstappen SMM, et al. Association between psoriatic disease and lifestyle factors and comorbidities: Cross-sectional analysis and Mendelian randomization. Rheumatology (Oxford). 2023;62(3):1272-1285.
Alinaghi F, Calov M, Kristensen LE, et al. Prevalence of psoriatic arthritis in patients with psoriasis: A systematic review and meta-analysis of observational and clinical studies. J Am Acad Dermatol. 2019;80(1):251-265.e19.





