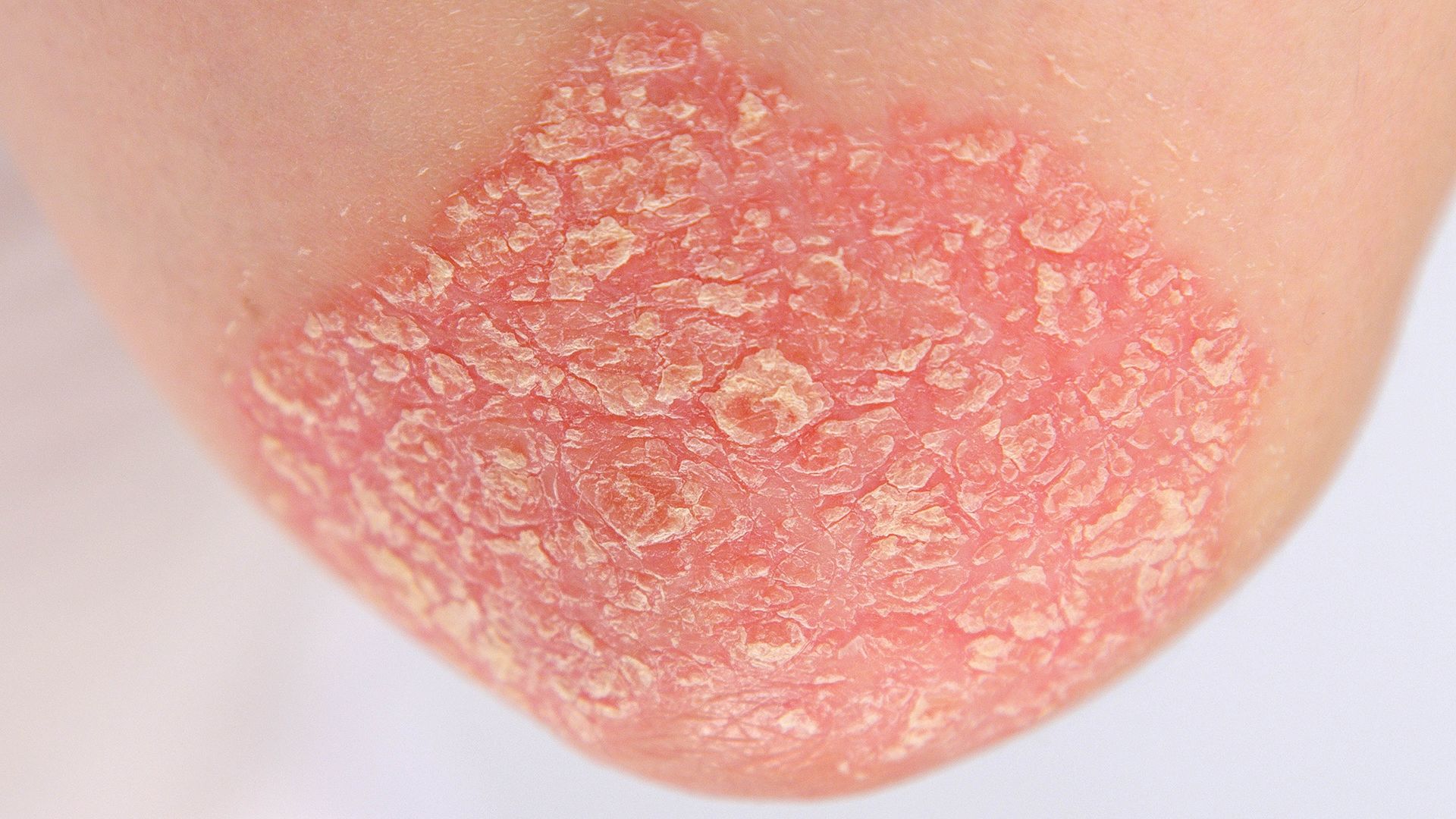
While the most well-known and common symptoms of psoriasis affect the skin, psoriatic disease can impact many different areas of the body. One example is psoriatic arthritis, a type of arthritis that affects up to 30 percent of people who have psoriasis. Both psoriasis and psoriatic arthritis are the result of abnormal immune system activity. With psoriasis, this abnormal immune system activity causes skin lesions, and with psoriatic arthritis, it causes inflammation in the joints.
Here, we look at an inflammatory eye condition called uveitis, which is a potential complication of psoriasis.
What is uveitis?
Uveitis is inflammation of the middle layer of the eye, which is called the uvea. Redness, pain, sensitivity to light, and visual disturbances are all symptoms of uveitis. These symptoms can progress suddenly or gradually. Uveitis can have a number of different causes—injuries, infections, medication side effects, certain cancers—or it can have no identifiable cause. Uveitis is also associated with autoimmune and inflammatory disorders. Treatment involves a combination of therapies to alleviate symptoms and therapies to treat the cause of uveitis—for example, medications to treat an infection, or medications to regulate an immune disorder.
What is the link between psoriasis and uveitis?
As mentioned in the previous paragraph, uveitis is associated with autoimmune and inflammatory disorders. There is some debate over whether psoriasis should be classified as an autoimmune disease, and “immune-mediated disease” is considered the more accurate term. Regardless of terminology, it is well established that psoriasis is a disorder of the immune system and that psoriasis is a systemic disease, meaning that it causes inflammation throughout the body. It is thought that uveitis occurs as a result of this systemic inflammation.
How common is uveitis?
Uveitis is rare, but is more prevalent among people who have psoriasis and psoriatic arthritis. It is estimated to affect between 7 and 20 percent of people who have psoriatic disease.
Can psoriasis cause other eye problems?
Healthcare researchers do not have a full understanding of the ways psoriatic disease can impact the eyes, but psoriasis is associated with a number of eye problems in addition to uveitis. These include conjunctivitis (commonly known as “pink eye”), blepharitis (inflammation of the eyelid), and dry eye.
Psoriasis lesions can also occur around the eyes and on the eyelids. This can cause the skin of the eyelids to become red, crusty, and scaled, and can cause pain and itching. Eyelid psoriasis or psoriasis lesions near the eyes are usually treated with special topical treatments. Not all topical treatments are safe to use around the eyes—the eyes are sensitive and the skin around the eyes is thinner and more delicate than skin in other areas of the body. Treatment must always be given under the guidance of a healthcare provider.
What can you do to keep your eyes healthy?
It is important to keep regular appointments with your healthcare providers. This includes the providers you see for psoriatic disease, such as a dermatologist or rheumatologist, as well as your eye doctor and primary care physician. Because these healthcare providers may need to communicate with one another when overseeing treatment, it helps to have your paperwork organized, including insurance information, your medical records, and any medications you take to treat psoriasis, eye problems, or other health conditions.
Remember that there are many conditions that can affect the eyes, which may or may not be related to psoriasis. Anytime you are experiencing symptoms that affect your eyes, it’s important to see a healthcare provider to get an accurate diagnosis and appropriate treatment.