Shingles
- What is shingles?
- What are the symptoms of shingles?
- What are the causes and risk factors for shingles?
- Who can get the shingles vaccine?
- When to see a healthcare provider for shingles
- How is shingles diagnosed?
- What are the stages of shingles?
- How is shingles treated?
- Living with shingles
- Featured shingles articles
Introduction
Nearly one in every three people in the United States will develop shingles in their lifetime, according to the Centers for Disease Control and Prevention (CDC). Shingles—also called herpes zoster (HZ)—causes a painful, blistering rash that may be itchy. This infection can affect anyone at any age, although shingles most often occurs in adults over the age of 50. The best way to reduce your risk of shingles is to get vaccinated.
Learn what shingles is and what causes it, how to spot the warning signs and symptoms, how the disease is diagnosed and treated, and what it means to live with a shingles infection.
What is shingles?
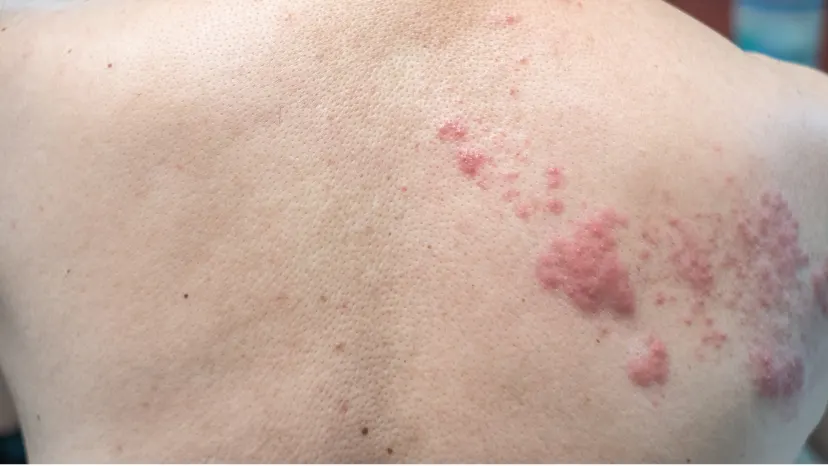
Shingles is a viral infection of the nerves right below the skin. It’s caused by the varicella-zoster virus (VZV), the same virus responsible for chickenpox. If you’ve ever had chickenpox, you’re at risk for shingles.
More than 99 percent of people in the U.S. born before 1980 have had chickenpox even if they don’t remember it, according to the CDC. Chickenpox infections are sometimes very mild, so cases may go unnoticed or undiagnosed.
The varicella-zoster virus is also known as human herpes virus 3 and it is a member of the herpes family of viruses. But shingles isn’t a sexually transmitted infection (STI) like genital herpes or oral herpes (commonly known as cold sores). These STIs are caused by herpes simplex virus 1 (HSV-1) and 2 (HSV-2).
How common is shingles?
Around one million people are diagnosed with shingles in the U.S. every year, and it’s becoming increasingly common, the CDC reports. Rates are rising most notably in young and middle-aged adults, while new cases have leveled off among older adults.
What does shingles look like?
Shingles may look slightly different from person to person. In many cases, a shingles rash appears as a red or discolored band of skin, often with small blisters. Shingles rashes typically appear on one side of the torso, neck, or face, though people with weakened immune systems are more likely to have widespread rashes that cover a large portion of the body.
What are the symptoms of shingles?

The main symptom of shingles in people with lighter skin is a red rash, sometimes with small bumps or fluid-filled blisters that may rupture and crust over. A shingles rash in someone with darker skin may appear more purple, pink, dark brown, or grey than red.
In addition to a rash, the infection can trigger symptoms that affect other parts of the body.
Most common shingles symptoms
Shingles symptoms usually include a combination of the following:
- Pain in a localized area or on one side of the body that may feel sharp, stabbing, or dull
- Burning or tingling sensations
- Increased sensitivity to touch
- Itchiness
The first signs of shingles typically occur two to five days before the rash develops. These signs may include numbness or tingling, pain, sensitivity to touch, or itchiness around the area where the rash eventually appears.
Although it can occur anywhere on the body, a shingles rash most often develops on one side of the torso, face, or neck. The shingles rash clears up in two to four weeks for most people. It’s possible to experience more than one outbreak of shingles in your lifetime, although this is uncommon.
Shingles symptoms throughout the body
In addition to skin-related symptoms, some people with shingles also experience:
- Fever
- Chills
- Increased sensitivity to light
- Headaches
- Upset stomach
- Fatigue
Internal shingles
For some people, a classic shingles rash may never develop but pain, sensitivity, and other symptoms are still present. Shingles without a rash is known as internal shingles, or zoster sine herpete. Possible symptoms of internal shingles include:
- A deep, twisting pain in muscles or joints
- A sharp, stabbing pain
- Burning sensations beneath the skin
- Abdominal pain
- Lesions on the cornea of the eye
- Sore throat
- Ear pain
In rare cases, internal shingles symptoms may lead to encephalitis and meningitis. Encephalitis is a condition involving inflammation of brain tissue. Meningitis involves inflammation of the meninges, which are the protective membranes that cover the brain and spinal cord.
When encephalitis or meningitis occur, symptoms include neck stiffness, severe headache, and altered mental status (AMS). AMS refers to a change in mental function, which may affect awareness or consciousness, movement, or behavior.
What are the causes and risk factors for shingles?
Shingles occurs in a person when the varicella-zoster virus that previously caused chickenpox reactivates in that person’s body.
After a person recovers from chickenpox, the virus becomes dormant—or goes to sleep—in certain parts of the nervous system. Specifically, the virus dwells in dorsal root ganglia, the parts of nerves that connect them to the spinal cord. Essentially, shingles occurs if the virus later “wakes up.” This allows the virus to replicate once again, making it more likely that shingles symptoms will appear.
The exact reason why the varicella-zoster virus reactivates in some people but not in others is unclear. But researchers think that the immunity that people once had against the virus that they gained through a case of chickenpox may fade over time.
Common risk factors for developing shingles include:
- Older age, with the likelihood of getting shingles being 10 times higher in adults over the age of 60 compared to children younger than 10
- Having a weakened immune system from taking immunosuppressant medications or due to conditions such as HIV and AIDS, certain cancers such as leukemia and lymphoma, severe psoriasis, and advanced psoriatic arthritis
- Having a family history of shingles
- Receiving a bone marrow transplant or solid organ transplant such as a heart transplant, kidney transplant, or liver transplant
- Taking medications that weaken the immune system such as steroids (also called corticosteroids or glucocorticoids), organ transplant rejection medicines, and chemotherapy drugs
- Experiencing severe psychological stress, which can weaken the immune system and allow the varicella-zoster virus to reactivate
Is shingles contagious?
Shingles itself is not contagious, but the varicella-zoster virus that causes the infection is. You can spread the shingles virus to another person who has never had chickenpox or who has never received the varicella (chickenpox) vaccine. Transmission occurs through direct contact with fluid from a blistered rash. Someone who contracts the varicella-zoster virus in this way will get chickenpox, not shingles.
The incubation period for the varicella-zoster virus ranges from 10 to 21 days. (Incubation describes the time it takes for an infection to develop and symptoms to appear following initial exposure to a disease-causing organism, such as a virus or bacteria.)
The varicella-zoster virus becomes contagious when the shingles rash blisters. Therefore, it’s important to keep your rash and sores fully covered until they heal to avoid potentially infecting other people.
What are the potential complications of shingles?
Long-term nerve pain, called postherpetic neuralgia (PHN), is a type of nerve damage and the most common complication of shingles. PHN can cause pain around the area of the shingles rash for several months or even years after the rash clears. It’s most likely to trigger severe and long-lasting pain in older adults and is rarely seen in people younger than 40.
Other potential shingles complications include:
- Vision problems and blindness if shingles affects the eyes (known as herpes zoster opthalmicus)
- Organ inflammation, including encephalitis
- Cellulitis, a type of bacterial skin infection.
- Facial paralysis, changes in hearing, or vertigo from Ramsay Hunt syndrome (also known as herpes zoster oticus), which occurs when shingles affects a facial nerve around one of your ears
In rare cases, shingles complications can be fatal. Don’t delay speaking with an HCP if you’re experiencing potential symptoms of shingles or its complications.
Shingles and pregnancy
During pregnancy, the varicella-zoster virus can spread through the placenta to the fetus, but shingles rarely causes complications for the fetus. A pregnant person infected with varicella-zoster virus is, however, at higher risk of pneumonia.
Although you can’t get vaccinated for shingles while pregnant, you may be able to get an injection of varicella zoster immunoglobulin (VZIG). VZIG contains antibodies to the virus that may help lower the risk of chickenpox or lessen its severity.
Although getting shingles during pregnancy is unlikely to be dangerous to the fetus, acquiring chickenpox during the first 20 weeks of pregnancy can lead to a group of symptoms collectively known as congenital varicella syndrome (CVS). Newborns affected with CVS can experience complications including blindness, intellectual disability, low birth weight, malformed and paralyzed limbs, microcephaly (smaller head size compared to infants of the same age and sex), muscle and bone conditions, premature birth, scars on the skin from chickenpox rash, and seizures.
If you’re exposed to someone with shingles or chickenpox during pregnancy, talk with your HCP right away about your treatment options.
Who can get the shingles vaccine?
The best way to protect yourself and others from the shingles virus is to receive the recombinant zoster vaccine, also called Shingrix or, simply, the shingles vaccine. Shingrix is different from the chickenpox vaccine that’s recommended for children, adolescents, and those who’ve never had chickenpox. It also differs from the live zoster virus vaccine (Zostavax), which is no longer available in the U.S.
The CDC encourages adults ages 50 and older to receive two doses of the shingles vaccine, separated by two to six months, to prevent shingles and its complications. Adults ages 19 and older who have a weakened immune system should also consider receiving two doses of the shingles vaccine.
If you’re eligible to receive the shingles vaccine, the CDC recommends you get vaccinated even if you already had shingles or chickenpox or received Zostavax or the chickenpox vaccine. If you have any questions regarding shingles vaccination and whether it’s right for you, be sure to consult with an HCP.
Can you get shingles from the vaccine?
You can’t get shingles from the shingles vaccine. In fact, Shingrix is more than 90 percent effective at preventing shingles. Although it’s possible to develop shingles after getting vaccinated, your symptoms will likely be less severe than if you had not received the shingles vaccine.
Although some people may be concerned about getting shingles from Shingrix, the vaccine only contains a small part of the varicella-zoster virus and doesn’t contain any live virus components.
When to see a healthcare provider for shingles
It’s important to promptly speak with a healthcare provider about shingles if you are experiencing potential symptoms, if you believe you may be at risk, or if you’ve already been diagnosed and your symptoms are getting worse. This is especially true if:
- You’re older than 50
- Your shingles rash is very large or causes severe pain
- Your shingles rash occurs near your eyes
- You or someone you live with has a weakened immune system
How is shingles diagnosed?
Your HCP may be able to diagnose shingles by simply looking at your rash. They may also ask you about other symptoms you are experiencing, as shingles is typically accompanied by pain, itching, or increased sensitivity to touch in one specific area or side of the body.
Some cases of shingles can appear similar to other skin conditions such as hives, rosacea, and different types of psoriasis and eczema. Therefore, a small tissue sample may be taken from the rash and tested for the varicella-zoster virus to confirm a shingles diagnosis.
Diagnosing internal shingles, or shingles without a rash, involves a few more steps. After evaluating your symptoms and discussing your medical history, your HCP may recommend a saliva polymerase chain reaction (PCR) test to screen for the DNA of the varicella-zoster virus and to confirm or rule out shingles.
What are the stages of shingles?
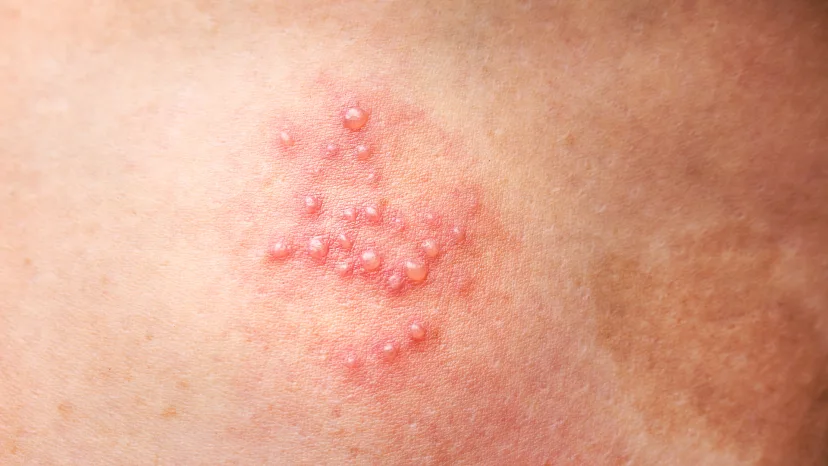
The stages of shingles may look slightly different from person to person. That said, the disease typically progresses in three phases:
- Pre-eruptive stage: This first phase usually involves burning or pain that occurs at least two days before a shingles rash develops. You may also experience headaches, fatigue, and increased sensitivity to light.
- Acute eruptive stage: A rash emerges during the active stage of shingles. This phase usually lasts two to four weeks and is characterized by the presence of a rash that may contain fluid-filled blisters. Severe pain may also be present. It’s possible to pass the varicella-zoster virus to others during this stage.
- Chronic stage: This stage of shingles refers to postherpetic neuralgia (PHN), which affects between 10 and 18 percent of people with shingles. PHN can cause lingering pain, which may be severe and can persist for at least four weeks after the shingles rash goes away.
How long does shingles last?
Most cases of shingles lasts around three to five weeks, although the pain of postherpetic neuralgia can linger. Contact your HCP if you have any questions or concerns about the duration or severity of your shingles.
How is shingles treated?
Viral infections like shingles can’t be cured, but early treatment can help clear up a shingles rash faster and keep pain from getting worse. Several treatments and home remedies can help soothe a shingles rash and better equip your immune system to overcome the infection.
Medication for shingles
Antiviral medication is the primary form of treatment for shingles. When taken shortly after symptoms appear, an antiviral medication can help:
- Shorten the duration of the infection
- Reduce the severity of the shingles rash and associated symptoms
- Lower your risk of complications like PHN
The most commonly prescribed antiviral medicines for shingles include acyclovir, valacyclovir, and famciclovir. It’s important to speak with an HCP as soon as possible if you believe you may have shingles, as antiviral medications are most effective when taken within 72 hours of symptom onset—preferably within the first 24 hours.
Your HCP may also recommend an over-the-counter medication to ease pain, such as acetaminophen or ibuprofen. If your shingles pain is severe, a prescription medication in pill, topical, or injection form can help. Depending on your condition and symptoms, your HCP may prescribe:
- A gel, cream, spray, or patch with a numbing agent, such as lidocaine
- An anticonvulsant medication like gabapentin
- A corticosteroid injection with a local anesthetic
- Capsaicin topical patches
- Tricyclic antidepressants, such as amitriptyline
Home remedies for shingles
Home remedies can play a big role in managing shingles symptoms. In addition to treatment from your HCP, the following self-care measures can ease shingles-related discomfort and help you feel more like yourself again:
- Place a cool, wet compress on your blisters to soothe pain and itching.
- Apply calamine lotion—an over-the-counter anti-itch medicine—to calm skin irritation. (Don’t use so much that it cakes on your rash, though.)
- Take a cool shower or bath to keep your rash clean and to ease pain. The CDC suggests trying colloidal oatmeal baths, or lukewarm bath water mixed with ground-up oatmeal.
- Keep your rash covered with loose-fitting clothing made from natural fibers like cotton and linen.
Additionally, be sure to avoid scratching, rubbing, or touching your shingles rash. The relief you feel will be short-lived, and scratching your skin can break open blisters and allow infection-causing bacteria to enter your skin. If you do touch your rash, be sure to wash your hands well for at least 20 seconds with soap and clean water.
It’s important to check in with your HCP before applying lotions or taking over-the-counter medicines to treat shingles. They can provide guidance on what home remedies are best for your specific needs.
Living with shingles

Medicines and HCP-approved home remedies can effectively treat the infection and ease symptoms, but how can you maintain a good quality of life while recovering from shingles? Since the infection may take several weeks to resolve, it’s important to prioritize your physical and emotional health when living with shingles. These tips may help:
Limit stress
Not only can stress incite a shingles outbreak, but it can also make symptoms worse. If possible, avoid or postpone stressful tasks or responsibilities until you’re feeling better. It’s also a good idea to incorporate stress-relieving practices into your daily routine, including:
- Deep breathing to ease pain and stress
- Engaging in a relaxing hobby you enjoy
- Journaling
- Listening to soothing or feel-good music
- Meditation or other mindful practices
Stay active
A shingles infection can drain your energy. But, if you’re able, practicing gentle stretching or walking can help ease pain and stress. Just be sure to avoid gyms and group exercise classes until your rash has healed and check in with your HCP before trying any new or vigorous exercises.
Be mindful of your diet
Some foods and beverages can hinder your immune system and trigger inflammation, neither of which is good for an infection like shingles. While you’re healing, try to avoid the following:
- Alcohol
- Foods high in saturated fats, such as butter, bacon, lard, sausage, coconut oil, palm oil, and other fatty meats
- Processed, pre-packaged snacks
- Sodas and other sugar-sweetened drinks
- Refined carbohydrates, such as white bread, potatoes, candy, rice, and sugary cereals
As much as possible, try to eat whole, nutrient-rich foods that nourish your body and help it heal. It’s a good idea to seek foods that are rich in B vitamins—particularly vitamin B12—which aid the nervous system and can help protect against the effects of postherpetic neuralgia. These include lean, grass-fed beef, eggs, chicken, and cultured dairy products. Foods that contain vitamin C—such as citrus fruits, tomatoes, broccoli, strawberries, and red and green peppers—are other great options if you’re dealing with shingles because the vitamin can help boost the immune system.
Do things you enjoy
Now is the time to rewatch your favorite movie, start a new book, or call up an old friend. Doing things you enjoy can help take your mind off shingles.
Finally, don’t hesitate to reach out to your HCP or a licensed mental health provider if you’re struggling to cope with the emotional or physical effects of a shingles infection. Shingles can be painful and having a rash can feel embarrassing.
Just remember that shingles is a very common condition and there are ample resources—including shingles support groups—that can help you better navigate this condition and maintain your quality of life.
Featured shingles articles

American Academy of Dermatology Association. Shingles: Causes. Accessed April 28, 2023.
American Academy of Dermatology Association. Shingles: Overview. Accessed April 28, 2023.
American Academy of Dermatology Association. Shingles: Diagnosis and Treatment. Accessed May 3, 2023.
Burnett T. What Are the Risks Associated With Chickenpox and Pregnancy? Mayo Clinic. Last updated November 9, 2022.
Centers for Disease Control and Prevention. Shingles (Herpes Zoster): Clinical Overview. Last reviewed October 5, 2020.
Centers for Disease Control and Prevention. Shingles (Herpes Zoster): Complications of Shingles. Last reviewed July 1, 2019.
Centers for Disease Control and Prevention. Shingles (Herpes Zoster): Diagnosis & Testing – For Healthcare Professionals. Last reviewed September 19, 2019.
Center for Disease Control and Prevention. Shingles (Herpes Zoster). Last reviewed February 3, 2022.
Centers for Disease Control and Prevention. Shingles (Herpes Zoster): Signs & Symptoms. Last reviewed July 1, 2019.
Centers for Disease Control and Prevention. Shingles (Herpes Zoster): Transmission. Last reviewed July 1, 2019.
Centers for Disease Control and Prevention. Shingles (Herpes Zoster): Shingles Burdens and Trends. Last reviewed August 14, 2019.
Centers for Disease Control and Prevention. Shingles Vaccination. Last reviewed May 24, 2022.
Cleveland Clinic. Calamine Lotion. Last reviewed June 24, 2022.
Cleveland Clinic. Shingles. Last reviewed February 2, 2022.
Cohen EJ, Jeng BH. Herpes zoster: A brief definitive review. Cornea. 2021;40(8):943-949.
Curhan SG, Kawai K, Yawn B, Rexrode KM, Rimm EB, Curhan GC. Herpes zoster and long-term risk of cardiovascular disease. J Am Heart Assoc. 2022;11(23):e027451.
Harvard Health Publishing. Foods That Fight Inflammation. Published November 16, 2021.
Horsager-Boehrer R. What Women Should Know About Chickenpox, Vaccination, and Pregnancy. Published April 5, 2022.
John Hopkins Medicine. Shingles. Accessed May 1, 2023.
Marra Y, Lalji F. Prevention of herpes zoster: A focus on the effectiveness and safety of herpes zoster vaccines. Viruses. 2022;14(12):2667.
Mayo Clinic. Ramsay Hunt Syndrome. Last updated August 20, 2022.
Mayo Clinic. Shingles. Last updated August 20, 2022.
MedlinePlus. Shingles. Last updated March 29, 2023.
Mother To Baby | Fact Sheets [Internet]. Brentwood (TN): Organization of Teratology Information Specialists (OTIS); 1994-. Herpes Zoster (Shingles) 2021 Apr 1.
National Foundation for Infectious Diseases. Shingles Myths and Facts. Accessed April 28, 2023.
National Health Service. Shingles. Last reviewed July 1, 2021.
National Institute of Neurological Disorders and Stroke. Shingles. Last reviewed March 13, 2023.
National Institute on Aging. Shingles. Last reviewed October 12, 2021.
NHS Inform. Shingles. Last updated February 13, 2023.
Patil A, Goldust M, Wollina U. Herpes zoster: a review of clinical manifestations and management. Viruses. 2022;14(2):192.
Piedmont Healthcare. Can Stress Trigger Shingles? Accessed May 11, 2023.
Nair PA, Patel BC. Herpes Zoster. StatPearls [Internet]. Last updated September 5, 2022.
Stanford Medicine Children’s Health. Chickenpox (Varicella) and Pregnancy. Accessed May 8, 2023.
UC Davis Health. 5 Things That Can Weaken Your Immune System. Published November 9, 2022.
Wang JY, Wu YH, Liu SJ, Lin YS, Lu PH. Vitamin B12 for herpetic neuralgia: A meta-analysis of randomised controlled trials. Complement Ther Med. 2018;41:277-282.
World Health Organization. Herpes Simplex Virus. Last updated April 5, 2023.
Yang Y, Mahmood T, Siddiqui AH, Aziz MA. Zoster Sine Herpete: Two unusual cases of varicella-zoster reactivation with atypical complaints of acute chest pain and severe headache. BMC Infect Dis. 2023;23(1):239.
Zhou J, Li J, Ma L, Cao S. Zoster sine herpete: A review. Korean J Pain. 2020;33(3):208-215.





