Sleep apnea
- What is sleep apnea?
- What are the types of sleep apnea?
- How common is sleep apnea?
- What are the symptoms of sleep apnea?
- What causes sleep apnea?
- What are the risk factors of sleep apnea?
- When should you see a healthcare provider for sleep apnea?
- What are the possible complications of sleep apnea?
- How is sleep apnea diagnosed?
- How is sleep apnea treated?
- Can you prevent sleep apnea?
- Living with sleep apnea
- Featured sleep apnea articles
Introduction
Sleep apnea is the most common of all sleep-disordered breathing (SDB) conditions. These are sleep disorders that disrupt or disturb breathing during sleep. Sleep apnea causes brief episodes in which your breathing slows down significantly or stops altogether while you sleep. These episodes can occur multiple times during sleep without you noticing or remembering them.
If you wake up feeling groggy or exhausted after a seemingly full night’s rest, sleep apnea could be the cause. There are several approaches to treating sleep apnea, including continuous positive airway pressure (CPAP) therapy, oral appliances, medicine, and surgery.
Understand the types, causes, risk factors, and symptoms of sleep apnea. Find out how it’s diagnosed and which therapies and lifestyle changes can help you prevent, treat, and manage this sleep disorder.
What is sleep apnea?

“Apnea” is a Greek word for “breathless.” Sleep apnea occurs when your breathing becomes very slow and shallow (known as hypopnea) or stops completely (apnea) for periods that may last from 10 seconds to a few minutes at a time while you sleep. These episodes can occur 30 times or more over the course of an hour.
If you have sleep apnea, you may sleep through pauses in your breathing or wake up gasping for breath. You may not remember waking up in some instances. Even if you manage to sleep through these lapses in breathing, you’ll likely feel tired or drowsy the following day.
What are the types of sleep apnea?
Sleep apnea is categorized by what causes the breathing disruptions. There are three main types of sleep apnea:
Obstructive sleep apnea (OSA)
The most common type of sleep apnea is obstructive sleep apnea (OSA). About 1 billion people worldwide have OSA. This includes around 30 million people living in the United States. Of those 30 million, only 6 million are diagnosed with the condition, according to the American Medical Association. This is most likely due to a lack of awareness about sleep apnea and its symptoms.
OSA occurs when the muscles that support the soft tissues at the back of your throat relax and block the upper airway, obstructing all or nearly all air flow and oxygen to the lungs. Your brain eventually recognizes the lack of airflow and oxygen, which triggers its survival instinct. This can cause gasping, choking, or snorting that may jostle you awake. OSA is generally characterized by having five or more of these breathing disruptions per hour of sleep.
Central sleep apnea (CSA)
Central sleep apnea results from a miscommunication between your brain and the muscles that manage breathing. It’s an uncommon condition that’s usually related to an underlying health issue such as Parkinson’s disease or congestive heart failure (CHF).
Usually, your brain controls your breathing when you’re awake and asleep. Central sleep apnea occurs when your brainstem—which connects your brain to your spinal cord—doesn’t properly signal your muscles to keep controlling breathing while you sleep. This may be due to damage to the nerve pathways that manage breathing. CSA may also occur when the brain stem fails to respond to rising carbon dioxide (CO2) levels in the blood.
The brain stem tends to be highly sensitive to changes in the level of CO2 in the blood. When CO2 levels are high, it usually cues respiratory muscles to breathe deeper and faster to remove excess CO2 each time you exhale. But with CSA, the brain stem fails to do this. As a result, you may experience episodes of hypopnea or apnea during sleep.
Treatment-emergent central sleep apnea (TECSA)
Formerly known as complex or mixed sleep apnea, TECSA involves both obstructive and central sleep apnea. Although uncommon, CSA temporarily develops or worsens after a patient receives treatment for OSA in which the airway is opened, such as during CPAP therapy or surgical placement of a tracheostomy. A tracheostomy is an opening (stoma) made in the front of the neck into the windpipe (trachea) to help facilitate the passage of air to and from the lungs.
How common is sleep apnea?
An estimated 5 to 10 percent of people around the world have sleep apnea. Anyone can develop this condition, but it’s more common in people assigned male at birth (AMAB) than people assigned female at birth (AFAB) and usually affects middle-aged and older adults.
What are the symptoms of sleep apnea?
The hallmark symptom of OSA is loud snoring that’s occasionally interrupted by choking or gasping sounds. You may have OSA if your partner says you frequently snore loudly or if your snoring wakes you up at night. OSA can also cause nocturia (frequent urge to urinate at night) and dry mouth upon waking.
Central sleep apnea is more closely associated with Cheyne-Stokes breathing (CSB), an abnormal breathing pattern that occurs during sleep. This may involve breathing that speeds up and gets deeper, slows down and becomes shallower, and then stops for a few seconds before breathing resumes. Shortness of breath can also result from central sleep apnea.
Other common sleep apnea symptoms include:
- Insomnia
- Waking up frequently during the night
- Excessive daytime sleepiness (EDS)
- Headaches, often in the morning
- Disruptions in cognitive (brain) function, which can lead to forgetfulness and trouble thinking and focusing
- Snoring loudly
- Mood changes, such as depression, anxiety, and increased irritability
- Sexual dysfunction (difficulties) and decreased libido (sex drive)
What causes sleep apnea?
Obstructive sleep apnea occurs when the throat muscles that support the tongue, tonsils, and the end of the soft palate (the roof of your mouth) relax too much during sleep. This can cause tissues toward the back of the mouth to collapse and the upper airway to become narrowed when you inhale, resulting in pauses in airflow that can last for 10 seconds or more at a time. For instance, your tongue can fall backwards when you sleep and disrupt breathing.
The causes of central sleep apnea are usually more complex than the factors behind OSA. Central sleep apnea can result from a variety of issues that impact your brain stem’s ability to regulate breathing muscles during sleep. It’s often associated with:
Cheyne-Stokes breathing: Also known as Cheyne-Stokes respiration, this rhythmic breathing pattern involves a slow and steady increase in breathing effort (crescendo) followed by a decrease in breathing effort (decrescendo), and sometimes an absence of breathing effort and airflow. Heart failure, stroke, and kidney disease are some of the health conditions associated with this abnormal breathing pattern.
Drug-induced apnea: Opioid medications like codeine, morphine, and oxycodone can disrupt regular breathing patterns and cause central sleep apnea.
High-altitude periodic breathing: Exposure to elevations around 15,000 feet above sea level or higher can cause a breathing pattern similar to Cheyne-Stokes breathing. However, high-altitude periodic breathing is tied to lower oxygen levels at these altitudes rather than a specific health condition. Breathing tends to get better once you move to a lower altitude.
Medical condition-induced sleep apnea: Certain health conditions can contribute to central sleep apnea, including stroke and kidney failure (also called end-stage kidney disease or end-stage renal disease).
Sometimes, the cause of central sleep apnea is unknown. These cases are referred to as idiopathic or primary CSA.
What are the risk factors of sleep apnea?

Although anyone at any age can develop sleep apnea, certain factors can make you more vulnerable. While having one or more of these risk factors can increase the likelihood of developing the sleep disorder, it’s also possible to experience sleep apnea without having any known risk factors.
Obstructive sleep apnea risk factors
Risk factors for obstructive sleep apnea include:
Obesity: Obesity is closely linked to OSA. For instance, fatty deposits around a person’s neck can block the upper airway and contribute to breathing problems during sleep.
Age: The risk of OSA rises with age. This is partially due to an increased tendency for older adults to develop fatty deposits around the neck and tongue.
Genes and family history: Genetic traits like the size and shape of the skull, face, and upper airway can play a role in a person’s OSA risk. Having certain genes can also raise the risk of health conditions that may lead to sleep apnea, such as the chromosomal disorder Down syndrome.
Sex assigned at birth: People AMAB are two to three times more likely to develop OSA than people AFAB (prior to menopause). People AMAB are also more likely to experience sleep apnea at a younger age.
Heart and kidney disease: OSA is present in as many as 40 to 80 percent of people with hypertension, coronary artery disease, heart failure, atrial fibrillation, stroke, and pulmonary hypertension (high blood pressure in the vessels leading from the heart to the lungs), according to the American Heart Association. Like heart failure, kidney failure can cause fluid buildup in the neck, which can obstruct the upper airway.
Hormone and endocrine disorders: Hormone levels can affect the size and shape of the airway, tongue, and face. People who have low thyroid hormone levels or elevated growth hormone levels are more likely to develop OSA. High insulin levels due to type 2 diabetes, increased levels of androgen (often classified as a male hormone) and hormones related to polycystic ovary syndrome (PCOS) can also raise the risk for OSA.
Unhealthy habits: Unhealthy lifestyle choices like drinking alcohol in excess and smoking can increase the risk of OSA. Alcohol tends to relax muscles in the back of the mouth, and smoking cigarettes can trigger inflammation in the upper airway and impact breathing.
Chronic nasal congestion: People who frequently experience nasal congestion at night are twice as likely to develop OSA than those who don’t.
Large tonsils: Having large tonsils can make a person more likely to develop OSA, as can having a large tongue.
Thick neck: Having a large neck circumference (bigger than 17 inches for people AMAB and 16 inches for people AFAB) is associated with an increased risk of OSA.
Underbite and small lower jaw: Having retrognathia (an underbite) or micrognathia (an unusually small lower jaw) can raise the risk for OSA.
Central sleep apnea risk factors
Risk factors associated with central sleep apnea include:
Age: Central sleep apnea most often affects people older than 60.
Sex assigned at birth: People AMAB have a higher risk of central sleep apnea than people AFAB.
Opioid use: Taking opioid medications such as oxycodone, morphine, and codeine can influence how your brain controls sleep and contribute to central sleep apnea.
Premature birth: Babies who are born before 37 weeks of gestation have an elevated risk of central sleep apnea, although the condition typically resolves in childhood.
Genetics: People with inherited conditions such as congenital central hypoventilation syndrome (a disorder that causes shallow breathing) have an increased risk of central sleep apnea.
Health conditions: Along with heart failure and stroke, a handful of other health conditions are associated with a heightened risk of central sleep apnea, including:
- Myasthenia gravis (an autoimmune disease that affects communication between nerves and muscles)
- Atrial fibrillation (which involves a fast, quivering heart rhythm)
- Amyotrophic lateral sclerosis (also known as ALS or Lou Gehrig's disease, the nervous system disorder affects nerve cells in the brain and spinal cord, causing progressive loss of muscle control)
- Brain tumor or brain stem lesion
When should you see a healthcare provider for sleep apnea?
Good sleep is essential to good overall health, so it’s important to see a healthcare provider (HCP) if you’re experiencing sleep apnea symptoms, if your partner says you snore loudly or gasp during sleep, or if you’re having trouble falling or staying asleep.
It’s especially important to seek medical care if you have heart disease, diabetes, or asthma, or if your symptoms make it difficult to attend school, work, or enjoy time with loved ones. If left untreated, sleep apnea can lead to potentially serious complications.
What are the possible complications of sleep apnea?

Not getting enough quality sleep due to sleep apnea or another issue can cause daytime fatigue, trouble concentrating, poor memory, and irritability that may spill over into your personal or professional life. The consequences of untreated or poorly managed sleep apnea can be serious and potentially life-threatening.
Increased risk of motor vehicle accidents
A 2022 study published in Sleep Medicine found a significantly higher risk of motor vehicle accidents among people with OSA. The study, which followed more than 48,000 participants with OSA for up to 24 years, also found that those with OSA were involved in more severe accidents. Additionally, a 2022 review and analysis of studies published in the Journal of Medicine found that working adults with OSA are more than twice as likely to be involved in a car accident, compared to members of the general population. These higher accident rates might be due to sleep apnea symptoms such as excessive daytime sleepiness, inattention, decreased alertness, and falling asleep while driving.
Links to heart disease
More research from the American Heart Association points to a strong link between heart disease and sleep apnea, particularly obstructive sleep apnea. OSA can worsen existing cardiovascular diseases, which in turn can exacerbate sleep apnea. For instance, OSA is a risk factor for atrial fibrillation and is present in 30 to 50 percent of people with high blood pressure. OSA is also associated with type 2 diabetes, worse outcomes for heart failure, and sudden cardiac death.
Connections to mental and other physical health issues
Poor sleep health from OSA is also connected to health issues like anxiety, depression, poor cognitive function, worsening asthma, and even damage to the brain from a lack of oxygen. The wide-ranging complications of sleep apnea underline the importance of promptly speaking with an HCP if you’re experiencing symptoms of this condition or are concerned about your sleep health.
How is sleep apnea diagnosed?
To diagnose sleep apnea, your HCP will likely start by asking you a series of questions about your:
- Sleep habits
- Symptoms
- Personal and family medical histories
- Medications, including any essential oils and dietary and herbal supplements you’re currently taking
Your HCP may also perform a physical exam to check for factors that could contribute to obstructive sleep apnea, such as the circumference of your neck, the size and position of your tongue, and whether you have excess tissue or other abnormalities around the back of your mouth, throat, or nose.
Based on the details of your symptoms, personal and family health history, and physical exam, your HCP may refer you to a sleep specialist—such as a doctor who specializes in sleep disorders called a somnologist—for more detailed assessment and testing. A sleep study is usually necessary to definitively diagnose sleep apnea.
Polysomnography (PSG)
Polysomnography is a type of sleep study that’s performed overnight at a clinic or sleep center. During the study, you’ll be connected to equipment that monitors your breathing as you sleep, as well as your heart rate, eye movements, muscle activity, brain activity, and blood oxygen levels. This information is used to diagnose sleep apnea and determine its severity. Polysomnography can also help rule out other sleep disorders, such as periodic limb movements and narcolepsy (sudden periods of sleep).
Home sleep study
A home sleep study is a portable version of polysomnography that involves wearing a small device with recording equipment and sensors as you sleep in your own bed. This small device measures your breathing patterns, airflow, blood oxygen levels, and heart rate during sleep. The collected information is then evaluated by a sleep specialist.
A home sleep study isn’t appropriate in every case. It’s usually recommended for people who are displaying symptoms of obstructive sleep apnea but are otherwise healthy. If you have an underlying health condition or your HCP suspects you may have central sleep apnea, polysomnography will likely be recommended instead of or in addition to a home sleep study.
How is sleep apnea treated?
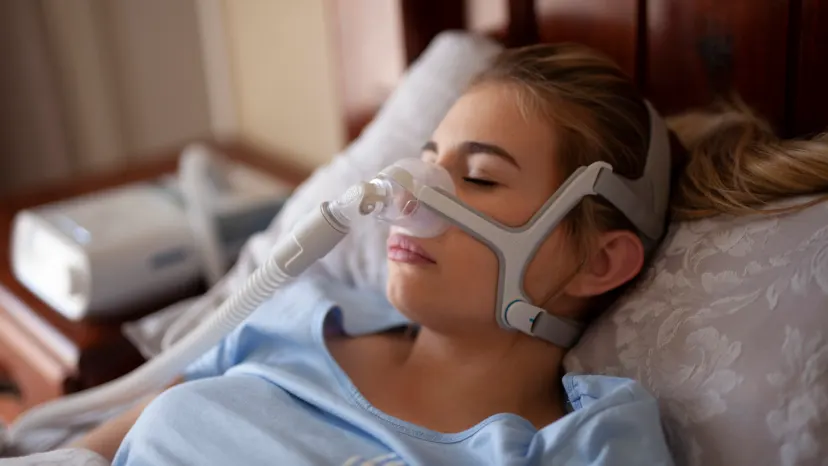
There are multiple approaches to sleep apnea treatment. Your best course of care will depend on what type of sleep apnea you have, its severity, and your overall health. While sleep apnea isn’t curable, taking steps to manage the condition can significantly improve sleep quality, minimize symptoms, and prevent complications.
Continuous positive airway pressure (CPAP) therapy
Continuous positive airway pressure (CPAP) is largely considered the “gold standard” of sleep apnea treatment. It involves wearing a CPAP device, a mask connected to a small machine that delivers constant air pressure to your throat to help keep your airway open as you sleep. The machine delivers the precise amount of air pressure you need, as determined by the results of your sleep study.
The CPAP mask comes in a variety of configurations, including styles that cover your nose, mouth, or both. Compact, battery-operated CPAP devices designed for travel are also available.
Auto-adjusting positive airway pressure (APAP) therapy
Auto-adjusting positive airway pressure (APAP) adjusts air pressure based on your breathing patterns as you sleep. In contrast, standard CPAP machines emit a fixed amount of air pressure. APAP technology is sometimes incorporated into CPAP machines (known as auto-CPAP).
Your HCP can set upper and lower air pressure limits on your APAP device, but the machine will adjust the amount of air pressure on its own based on your breathing patterns as you sleep. For example, you may need less air pressure to keep your airway open when you sleep on your side than when you lie on your back.
Bilevel positive airway pressure (BPAP) therapy
Bilevel positive airway pressure (BPAP) delivers two fixed levels of air pressure—one for when you inhale and one for when you exhale. These air pressure levels are programmed into the BPAP machine based on the results of your sleep study. Some BPAP devices can also deliver a breath if you haven’t inhaled for a certain number of seconds.
BPAP is typically recommended for people with obstructive sleep apnea that doesn’t improve with CPAP therapy. It’s not recommended for people with central sleep apnea related to heart failure.
Oral appliances
Your HCP may suggest sleeping with a custom oral appliance if you don’t tolerate positive airway pressure therapy well or if your sleep apnea symptoms aren’t severe. There are two main types of oral appliances, both of which work to keep the airway open:
- Tongue retaining devices, which keep the tongue in a forward position to prevent it from falling backwards.
- Mandibular repositioning mouthpieces, which help expand the airway by holding the upper and lower jaw in a certain position.
The U.S. Food and Drug Administration (FDA) recently approved a new type of oral appliance that can be worn during the day. The removable DNA (daytime-nighttime appliance) oral device provides electrical muscle stimulation that strengthens the tongue muscle, helping to keep it forward and the airway open during sleep. Treatment involves wearing the DNA device 20 minutes every day for six weeks, among other steps.
Medication
Some cases of central sleep apnea may be treated with medications like acetazolamide, which help encourage breathing during sleep. Your HCP may recommend medication if you don’t respond well to CPAP therapy.
Your HCP might also recommend changing certain medicines you take if they’re making your sleep apnea symptoms worse. These include pain medicines such as opioids.
Supplemental oxygen
Wearing a device that supplies supplemental oxygen to your lungs while you sleep may be helpful if you have central sleep apnea.
Lifestyle changes
Certain lifestyle changes can go a long way toward improving sleep for many people with sleep apnea. These changes include:
- Losing excess weight (research shows that losing just 10 percent of body weight can significantly improve sleep apnea in overweight individuals)
- Exercising regularly, but not too close to bedtime (a workout-fueled adrenaline rush may keep you awake)
- Limiting caffeine to earlier in the day instead of close to bedtime
- Quitting smoking
- Limiting or avoiding alcohol, especially in the evening
- Sleeping on your side or stomach instead of your back to help keep your airway open
- Avoiding medicines or substances that induce sleep such as sedatives, as these can disrupt breathing by relaxing the muscles in the back of your throat
Surgery
If persistent or severe sleep apnea doesn’t respond to nonsurgical treatment, surgery to help improve breathing may be recommended. The main types of surgery for sleep apnea include:
- Adenotonsillectomy: Large adenoids (lymphatic tissue at the back of the throat) or tonsils are removed.
- Uvulopalatopharyngoplasty (UPPP): Tissue at the back of the throat that may block the airway is removed, sometimes along with adenoids or tonsils.
- Jaw surgery: The upper jaw (maxilla) or lower jaw (mandible) are repositioned to enlarge the airway.
- Upper airway stimulation: A small implant (hypoglossal nerve stimulator) is placed under the skin in the chest area to monitor breathing patterns and stimulate tongue movement, when necessary. Similarly, treatment that stimulates the phrenic nerves—which connect the diaphragm to the spinal cord and help control breathing—is an option for central sleep apnea.
- Somnoplasty: Soft tissue around the back of the throat is reduced using heat (radiofrequency ablation).
- Septoplasty: Soft tissue in the nose is straightened to improve airflow through the nasal passages.
- Tracheostomy: In severe, life-threatening cases, a small opening is made in the neck to accommodate a metal or plastic tube through which you’ll breathe when sleeping.
Can you prevent sleep apnea?
Sleep apnea can’t always be prevented, but implementing healthy lifestyle habits can lower your risk for this sleep disorder and prevent symptoms. Aim to:
- Practice habits that support sound sleep (sometimes referred to as sleep hygiene)
- Manage any health conditions you might have that raise the risk for sleep apnea, such as type 2 diabetes, high blood pressure, heart failure, and high cholesterol
- See your HCP at least once a year for a routine check-up
Living with sleep apnea

Sleep plays a vital role in your overall health and quality of life, so living with sleep apnea or any condition that impacts your sleep can be a challenge. Thankfully, there are several science-backed ways to control manage your sleep apnea and improve your sleep health.
Living well with sleep apnea begins with carefully following the treatment plan provided by your HCP. If you have any questions or concerns about your prescribed treatments (for example, how to keep your CPAP machine clean or what to do if an oral appliance isn’t improving your sleep apnea), be sure to reach out to your HCP for guidance.
Other ways you can help improve your sleep (and in turn, your overall health) include:
- Turning you room into a sleep sanctuary by decorating with soothing colors, installing blackout curtains, or investing in a white noise machine
- Stick to a regular sleep schedule, including setting times for showering, brushing your teeth, going to bed, and waking up—even on weekends, vacations, and holidays
- Powering down your smartphones and other light-emitting devices at least 30 minutes before bed
- Avoiding eating large meals late at night or drinking caffeine within six to eight hours of going to bed
If the effects of your sleep apnea include anxiety or depression, sharing your feelings with a loved one or joining an online or in-person sleep apnea support group can help. You may also want to consider speaking with a licensed mental health provider. With the proper treatment and support, you can manage your sleep apnea symptoms and enjoy an active, healthy life.
Featured sleep apnea articles

American Medical Association. What Doctors Wish Patients Knew About Sleep Apnea. Published April 1, 2022.
American Sleep Apnea Association. Sleep Apnea. Sleephealth.org. Accessed May 30, 2023.
Benjafield AV, Ayas NT, Eastwood PR, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: A literature-based analysis. Lancet Respir Med. 2019;7(8):687-698.
Cleveland Clinic. CPAP Machine.
Cleveland Clinic. Obstructive Sleep Apnea. Last updated November 15, 2022.
Cleveland Clinic. Sleep Apnea. Last reviewed November 15, 2022.
European Lung Foundation. Sleep Disordered Breathing. Last updated May 17, 2023.
Gottlieb, D.J., Ellenbogen, J.M., Bianchi, M.T. et al. Sleep deficiency and motor vehicle crash risk in the general population: A prospective cohort study. BMC Med 16, 44 (2018).
Gomase VG, Deshmukh P, Lekurwale VY. Obstructive sleep apnea and its management: A narrative review. Cureus. 2023;15(4):e37359.
John Hopkins Medicine. Obstructive Sleep Apnea. Accessed May 29, 2023.
Luzzi V, Mazur M, Guaragna M, et al. Correlations of obstructive sleep apnea syndrome and daytime sleepiness with the risk of car accidents in adult working population: A systematic review and meta-analysis with a gender-based approach. J Clin Med. 2022;11(14):3971.
Mayo Clinic. Central Sleep Apnea. Updated August 7, 2021.
Mayo Clinic. Obstructive Sleep Apnea. Updated July 27, 2021.
Mayo Clinic. Sleep Apnea. Updated April 6, 2023.
Milicic Ivanovski D, Milicic Stanic B, Kopitovic I. Comorbidity profile and predictors of obstructive sleep apnea severity and mortality in non-obese obstructive sleep apnea patients. Medicina (Kaunas). 2023;59(5):873.
National Institute of Neurological Disorders and Stroke. Sleep Apnea. Last reviewed January 20, 2023.
National Heart, Lung, and Blood Institute. Sleep Apnea: Causes and Risk Factors. Last updated March 24, 2022.
National Heart, Lung, and Blood Institute. Sleep Apnea: Diagnosis. Last updated March 24, 2022.
National Heart, Lung, and Blood Institute. Sleep Apnea: Treatment. Last updated March 24, 2022.
Roberts EG, Raphelson JR, Orr JE, LaBuzetta JN, Malhotra A. The pathogenesis of central and complex sleep apnea. Curr Neurol Neurosci Rep. 2022;22(7):405-412.
Sheikh Shoib, Irfan Ullah, Sachin Nagendrappa, Anab Rehan Taseer, Domenico De Berardis, Manjeet Singh, Muhammad Sohaib Asghar. Prevalence of mental illness in patients with obstructive sleep apnea – A cross-sectional study from Kashmir, India,
Annals of Medicine and Surgery. Volume 80, 2022, 104056, ISSN 2049-0801.
St-Onge MP, Tasali E. Weight Loss Is Integral to Obstructive Sleep Apnea Management. Ten-Year Follow-up in Sleep AHEAD. Am J Respir Crit Care Med. 2021;203(2):161-162.
Strohl KP. Sleep Apnea. Merck Manual Consumer Version. Last reviewed October 2022.
Badr, M Safwan. Central Sleep Apnea. UpToDate. Last updated September 30, 2021.
Kline, Lewis R. Clinical Presentation and Diagnosis of Obstructive Sleep Apnea in Adults. UpToDate. Last updated January 13, 2023.
Udholm N, Rex CE, Fuglsang M, Lundbye-Christensen S, Bille J, Udholm S. Obstructive sleep apnea and road traffic accidents: a Danish nationwide cohort study. Sleep Med. 2022;96:64-69.
Yeghiazarians Y, Jneid H, Tietjens JR, et al. Obstructive sleep apnea and cardiovascular disease: A scientific statement from the American Heart Association [published correction appears in Circulation. 2022 Mar 22;145(12):e775]. Circulation. 2021;144(3):e56-e67.
Zeineddine S, Badr MS. Treatment-emergent central apnea: Physiologic mechanisms informing clinical practice. Chest. 2021;159(6):2449-2457.