Psoriasis
- What is psoriasis?
- What are the common symptoms of psoriasis?
- What causes psoriasis?
- What are the main risk factors for psoriasis?
- What triggers psoriasis?
- What are the different types of psoriasis?
- What potential complications are related to psoriasis?
- Diagnosing psoriasis
- What types of psoriasis treatments can improve skin health?
- How to live well with psoriasis
- Featured psoriasis articles
Introduction
Approximately 3 percent of U.S. adults—more than 7.5 million Americans—have psoriasis. It’s one of the most common skin conditions globally, as well, affecting around 60 million adults.
What is psoriasis and how does it develop? Are some people at greater risk than others? Is there a cure?
Learn about psoriasis causes, types of psoriasis, risk factors, and triggers, as well as the latest research on treatments that can help improve your skin health. Understand why people with psoriasis are at greater risk for other health issues and why psoriasis is often mistaken for eczema, another chronic skin condition.
What is psoriasis?

Psoriasis is a chronic skin condition that causes new skin cells to grow too fast.
Ordinarily, it takes several weeks for new skin cells to fully develop and replace old skin cells as part of the body’s natural process of regeneration. But when you have psoriasis, this growth cycle is accelerated and takes only a few days. As a result, your skin becomes inflamed and thick lesions called plaques often form on its surface. Meanwhile, old skin cells continue to shed, which causes these patches of dry skin to become flaky and scaly and often sore and swollen.
Psoriasis is not infectious or contagious and you cannot spread it to other people. While there is no cure for the condition, it can be managed and treated.
What are the common symptoms of psoriasis?
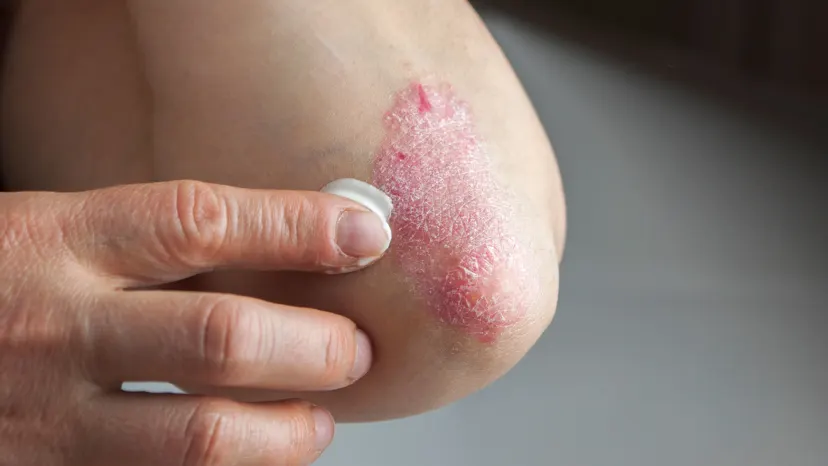
Psoriasis is considered mild, moderate, or severe based on the symptoms you may experience. These symptoms can vary, depending on the type of psoriasis you have.
Some of the more common psoriasis symptoms include:
- Discolored patches of skin
- Dry, flaky, or cracked skin that can feel itchy or may bleed
- Sore, inflamed skin that may burn at or near the affected site
- Joint pain
- Thick, pitted, and cracked nails
The appearance of psoriasis may vary depending on one’s skin type. For example, on people with darker skin, it may appear dark brown or purple with grayish scale on top. On people with lighter skin, psoriasis typically appears red with a silvery scale.
Symptoms tend to cycle between periods when your skin flares up and when your psoriasis symptoms go into remission. This means you may sometimes get a break from symptoms.
What causes psoriasis?
Researchers are working to determine the exact causes of psoriasis, but like a number of other chronic skin diseases, psoriasis is considered to be an autoimmune disease.
Autoimmune diseases occur when your immune system attacks your body’s healthy tissue.
When your immune system is working properly, its white blood cells (WBCs) make antibodies that protect you against pathogens such as bacteria, viruses, and fungi. In the case of psoriasis, WBCs called T lymphocytes (or T cells) trigger the rapid overgrowth of cells in the outermost layer of your skin.
Researchers have identified certain genes that are linked to psoriasis. Having these genes or a family history of psoriasis could increase your risk for the condition. Not everyone who carries these genes goes on to develop psoriasis, however, and some people may develop psoriasis even if they have no family history of the condition. Experts believe that certain health issues or aspects of your environment may also influence whether you develop the disease and have symptoms.
What are the main risk factors for psoriasis?
Along with a family history of the disease, there are several factors that are associated with an increased risk of developing psoriasis. Some of them are considered intrinsic, meaning they originate within the body or from other conditions you may have. These include:
- Obesity
- Diabetes
- High cholesterol
- High blood pressure
Other risk factors that come from your environment or habits are known as extrinsic factors. These may include:
- Smoking and alcohol use
- Certain drugs and medications
- Injuries or infection
- Air pollution or sun exposure
The way in which risk factors influence psoriasis is complicated, and researchers continue to untangle their influence. Though children may develop psoriasis, it occurs mostly in adults and affects men and women equally.
What triggers psoriasis?
Some of the factors that increase one’s risk of developing psoriasis in the first place may also cause symptoms to flare if you already have the condition. Common psoriasis triggers include:
- Medications, such as some used to treat high blood pressure, malaria, and bipolar disorder
- Drinking alcohol
- Dry, cold weather
- Hypocalcemia (low levels of calcium in your blood)
- Obesity
- Infections and illnesses such as bronchitis, cold and flu, HIV, and strep throat
- Smoking tobacco and exposure to secondhand smoke
- Trauma or injury to the skin such as scrapes, burns, cuts, puncture wounds, tattoos, and piercings
- Psychological and emotional stress
What are the different types of psoriasis?
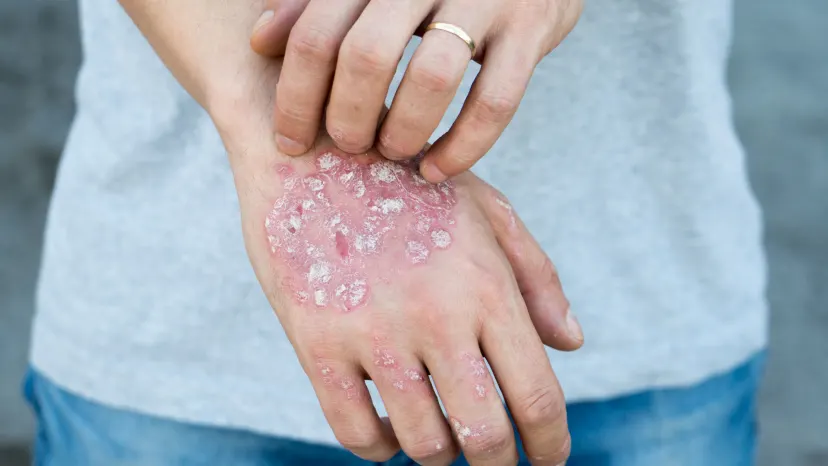
If you have psoriasis, you’ll likely experience only one kind. It is possible, though, to develop more than one type of psoriasis. These might include:
Plaque psoriasis
This is the most common type of psoriasis, affecting about 80 to 90 percent of people with the condition. Also known as psoriasis vulgaris, it’s characterized by thick, raised, scaly patches of skin known as plaques. Psoriasis plaques can break out anywhere, but they tend to form on the back, elbows, face, knees, palms, and scalp.
Scalp psoriasis
Scalp psoriasis can result in thick, crusted plaques or fine scales that resemble dandruff. It can affect your entire scalp or parts of it, such as your hairline and forehead or the skin at the back of your neck or around your ears. It’s the second-most common type of psoriasis. Around 45 to 56 percent of people with psoriasis have this type.
Inverse psoriasis
This type produces smooth or shiny lesions in areas of your body that are creased, such as the skin folds of your armpits, breasts, knees, or buttocks, genitals, and groin area.
Erythrodermic psoriasis
Erythrodermic psoriasis is the rarest type, but it can lead to severe and possibly life-threatening complications. It produces painful and itchy rashes over large areas of the body. These rashes can peel and leave your skin looking and feeling burned.
The condition may cause the body to have a hard time regulating its fluid balance and temperature, which can lead to shivering and edema (swelling). This may place you at higher risk for serious health issues such heart failure and pneumonia.
Guttate psoriasis
Guttate psoriasis produces small, raised, drop-shaped spots called papules. These papules usually appear on your arms, legs, and torso but they can also emerge on your ears, face, and scalp.
Pustular psoriasis
Painful sores called pustules are the hallmark of this form of psoriasis. These white or yellow bumps are filled with pus and the skin around them appears inflamed or discolored.
Pustular psoriasis can affect large swaths of the body or specific areas such as the palms of the hands, base of the thumbs, soles of the feet, sides of the heels, or the tips of fingers and toes and nails.
Nail psoriasis
Psoriasis can discolor your nails and cause pitting or horizontal ridges (also known as Beau’s lines) to form. This can leave your fingernails and toenails looking warped or deformed. Also called psoriatic nail disease, the condition can cause your nails to crumble or separate from their nail bed (an issue called onycholysis).
The affected areas may feel tender and painful. This can make it hard to stand, walk, or move your fingers and toes without discomfort.
What potential complications are related to psoriasis?
Complications related to psoriasis may include:
- Cardiac events such as heart attack or stroke
- Discolored skin and scarring
Having psoriasis may also be associated with an increased risk of other health conditions, including:
- Anxiety and depression
- Asthma
- Atherosclerosis, high blood pressure, or high cholesterol
- Cancer, such as bladder cancer, lung cancer, nonmelanoma skin cancer, and lymphoma
- Celiac disease, diverticulitis, or inflammatory bowel disease (including ulcerative colitis and Crohn’s disease)
- Cirrhosis
- Diabetes and metabolic syndrome
- Gout
- Hyperthyroidism and hypothyroidism
- Kidney disease
- Migraine
- Multiple sclerosis
- Non-alcoholic fatty liver disease
- Overweight and obesity
- Parkinson’s disease
- Sleep disorders such as obstructive sleep apnea
- Uveitis (inflammatory eye disease)
- Secondary infections, such as staph infections
What is psoriatic arthritis?
Close to one-third of all people with psoriasis also have psoriatic arthritis (PsA). Like rheumatoid arthritis, PsA is a chronic autoimmune disease that causes joints to become stiff, swollen, tender, and painful. Frequent and severe symptoms can result in permanent joint deformity and disability.
Diagnosing psoriasis
If you’re experiencing any of the symptoms of psoriasis, it’s important to see a healthcare provider (HCP) to receive a proper diagnosis. Your provider may refer you to a dermatologist for a skin examination and to discuss your family history of skin diseases or any other risk factors you may have.
A diagnosis of psoriasis is typically reached based on a physical examination. In some cases, such as if your symptoms are unclear, your HCP may wish to take a biopsy of your skin. This is a simple in-office procedure in which your HCP numbs an area of your skin and takes a small sample. The sample is sent to a lab to confirm the diagnosis and to rule out other possible conditions.
What is the difference between psoriasis and eczema?
You may have heard of eczema, another chronic skin condition with symptoms similar to psoriasis. While some symptoms may be common, there are several important differences between psoriasis and eczema worth recognizing.
For one, psoriasis is an autoimmune disorder in which the body attacks its own tissues. While eczema does involve inflammation and the immune system, it is not technically an autoimmune disorder. Rather, eczema tends to crop up when irritants in the environment (such as soaps or allergens) directly affect the skin.
People with psoriasis and eczema may experience rash, discolored skin, and discomfort, but eczema flare-ups tend to be more itchy while psoriasis plaques tend to produce more burning, pain, and soreness. Eczema tends to appear as thinner patches, while psoriasis plaques are usually thicker. Lastly, while both psoriasis and eczema can appear in both children and adults, psoriasis patients tend to first experience their symptoms in adulthood while eczema typically manifests in childhood.
A dermatologist can distinguish between the two conditions and give you the right diagnosis to help you get the treatment you need.
What types of psoriasis treatments can improve skin health?
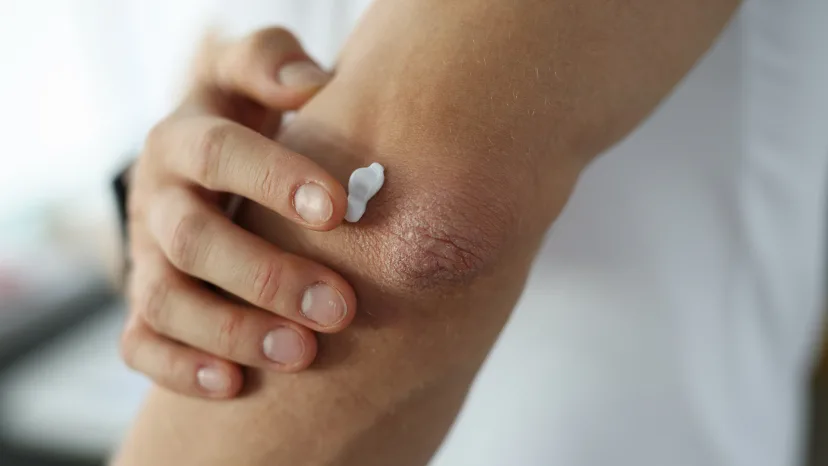
While there is no cure for psoriasis, there are many effective treatments that can help you prevent and tame flare-ups. Some of the main psoriasis treatments include:
Topical psoriasis medications
These include prescription and over-the-counter (OTC) creams and ointments applied to your skin. Ingredients may include:
- Coal tar
- Corticosteroids
- Roflumilast cream
- Synthetic vitamin D (also called vitamin D analogue)
- Salicylic acid
- Tapinarof cream
- Tazarotene
Some OTC psoriasis creams and ointments may also include compounds such as aloe vera, capsaicin, jojoba, and zinc pyrithione to help soothe inflamed skin, ease dryness and itching, and exfoliate scales.
Phototherapy for psoriasis
Your HCP may recommend adding phototherapy to your psoriasis treatment plan. This noninvasive treatment involves using a device equipped with light-emitting diodes to expose your skin to controlled amounts of ultraviolet (UV) light.
There are two types of UV light, UVA and UVB. While excessive exposure to either type is dangerous (they are both linked to skin cancer), moderate amounts of UVB can help ease psoriasis by regulating the T cells that contribute to the overgrowth of skin cells. UV treatments can help:
- Dissolve scales
- Ease inflamed, itchy skin
- Slow down the rapid growth of skin cells
- Suppress an overactive immune system
Systemic psoriasis treatments
Your HCP may also prescribe a psoriasis medication that works throughout the body rather than simply targeting breakouts in specific areas. These include the following FDA-approved treatments:
- Acitretin (a type of retinoid)
- Apremilast
- Biologics (which block the overactive part of your immune system that causes psoriasis symptoms)
- Cyclosporine
- JAK inhibitors
- Methotrexate
How to live well with psoriasis
Psoriasis can not only affect your physical health but also your general sense of well-being. But you can take charge of your health and make choices to live better and thrive with psoriasis.
The first step is to work closely with your HCP to develop a treatment plan and to coordinate closely on any adjustments you may need to make along the way.
How can I manage my psoriasis flare-ups?
Not everyone has the same psoriasis triggers. Knowing how to keep yours in check can reduce the frequency and severity of flare-ups. Your psoriasis management strategy might include these steps:
- Keeping your skin moisturized as much as possible
- Maintaining a healthy weight
- Quitting smoking if you smoke and avoiding secondhand smoke
- Quitting or limiting how much alcohol you drink
- Getting a small amount of sunlight each day
- Managing your stress with activities such as journaling, meditation, or yoga
- Avoiding any additional psoriasis triggers you have identified, such as cold weather or certain medications
Psoriasis can make people feel isolated or embarrassed of their appearance and can take a toll on their mental health. As a result, patients may be at higher risk for anxiety and depression. If you find it difficult to cope emotionally with your condition, ask your HCP for a referral to a counselor or a mental health professional. It may also help to join a psoriasis support group to share coping strategies and to find common cause with other psoriasis patients.
Can certain foods help reduce psoriasis flare-ups?
Your HCP may recommend that you adopt a specific eating plan, depending on your experience with psoriasis. If losing weight may help your psoriasis, you may be advised to follow a low-calorie diet.
Since psoriasis is linked to inflammation, you may also be advised to follow an anti-inflammatory diet that emphasizes fruits and vegetables, whole grains, beans and legumes, lean meats, and healthy fats from foods like nuts and fish. The antioxidants in fresh produce and the omega-3 fatty acids in fish and certain nuts and vegetable oils can help reduce inflammation and the risk of psoriasis flare-ups. You’ll also want to reduce intake of foods that are linked to increased inflammation in the body, such as alcohol, added sugar, refined grains, dairy products, and saturated fats from red and processed meats.
Diets in this mold include plant-based eating styles such as vegetarian or vegan diets or the Mediterranean diet.
Should I follow a gluten-free diet if I have psoriasis?
Some research suggests that people with psoriasis may also have higher rates of celiac disease. Celiac is an autoimmune condition in which gluten—a protein found in wheat, barley, and rye—triggers the body to attack the tissue that lines the small intestine. If you have psoriasis and celiac disease, eliminating gluten from your diet may reduce symptoms of both conditions.
Some people with psoriasis who have a sensitivity to gluten but not celiac disease may also benefit from eliminating gluten-containing foods from their diet. But experts note that if you don’t have celiac or a gluten sensitivity, eliminating gluten from your diet is unlikely to ease your psoriasis symptoms.
Changing your diet in addition to managing your psoriasis is no small task, so check in with your HCP for guidance. They may recommend you consult with a dietitian to learn how to integrate simple dietary strategies into your overall psoriasis treatment plan. You can start with small steps—like reducing your intake of processed foods—before gradually cutting more foods and introducing new ones into your eating plan.
Featured psoriasis articles

American Academy of Dermatology Association. Healthy Diet and Other Lifestyle Changes That Can Improve Psoriasis. Accessed February 21, 2023.
American Academy of Dermatology Association. Psoriasis: Diagnosis and Treatment. Accessed February 21, 2023.
American Academy of Dermatology Association. Psoriasis: Overview. Accessed February 22, 2023.
American Academy of Dermatology Association. Are Triggers Causing Your Psoriasis Flare-Ups? Accessed January 30, 2023.
Armstrong AW, Mehta MD, Schupp CW, Gondo GC, Bell SJ, Griffiths CEM. Psoriasis prevalence in adults in the United States. JAMA Dermatol. 2021;157(8):940-946.
Bu J, Ruilian D, Liangjia Z, Xiangmin C, Erxia S. Epidemiology of psoriasis and comorbid diseases: A narrative review. Front Immunol. 2022;13.
Cleveland Clinic. Nail Psoriasis. April 25, 2022.
Cleveland Clinic. Psoriasis. Updated September 15, 2022.
Kocaaga A, Kocaaga M. Psoriasis: An immunogenetic perspective. Glob Med Genet. 2022;9(2):82-89.
Mayo Clinic. Psoriasis. Updated October 8, 2022.
Musumeci ML, Nasca MR, Boscaglia S, Micali G. The role of lifestyle and nutrition in psoriasis: Current status of knowledge and interventions. Dermatol Ther. 2022;35(9):e15685.
Nair PA, Badri T. Psoriasis. StatPearls [Internet]. Updated April 6, 2022.
National Institute of Arthritis and Musculoskeletal and Skin Diseases. Psoriasis. Last reviewed September 2020.
National Psoriasis Foundation. About Psoriatic Arthritis. Accessed February 21, 2023.
National Psoriasis Foundation. Causes and Triggers. Accessed February 21, 2023.
National Psoriasis Foundation. Complementary and Integrative Medicine. Accessed February 22, 2023.
National Psoriasis Foundation. Erythrodermic Psoriasis. Accessed February 22, 2023.
National Psoriasis Foundation. Guttate Psoriasis. Accessed February 22, 2023.
National Psoriasis Foundation. Psoriasis Guidelines. Accessed February 22, 2023.
Ramessur R, Corbett M, Marshall D, et al. Biomarkers of disease progression in people with psoriasis: A scoping review. Br J Dermatol. 2022;187(4):481-493.
The search for measurable predictors linked with negative health complications in psoriasis. Br J Dermatol. 2022;187(4):e158-e167.
World Health Organization. Global Report on Psoriasis. Accessed February 17, 2023.
Parisi R, Iskandar IYK, Kontopantelis E, et al. National, regional, and worldwide epidemiology of psoriasis: systematic analysis and modelling study. BMJ. 2020;369:m1590. Published 2020 May 28.
Kamiya K, Kishimoto M, Sugai J, Komine M, Ohtsuki M. Risk Factors for the Development of Psoriasis. Int J Mol Sci. 2019;20(18):4347. Published 2019 Sep 5.
Arthritis Foundation. Light Therapy for Psoriatic Arthritis. Accessed March 7, 2023.
National Psoriasis Foundation. Psoriasis or Eczema? Accessed March 7, 2023.
National Psoriasis Foundation. Related Conditions of Psoriasis. Last updated on October 8, 2020.
American Academy of Dermatology Association. Can Psoriasis Affect More Than My Skin? Accessed March 7, 2023.
American Academy of Dermatology Association. What’s The Difference Between Eczema And Psoriasis? Accessed March 7, 2023.
National Psoriasis Foundation. Life with Psoriasis. Last updated on November 17, 2022.
Sahi FM, Masood A, Danawar NA, Mekaiel A, Malik BH. Association Between Psoriasis and Depression: A Traditional Review. Cureus. 2020;12(8):e9708. Published 2020 Aug 13.
Garbicz J, Całyniuk B, Górski M, et al. Nutritional Therapy in Persons Suffering from Psoriasis. Nutrients. 2021;14(1):119. Published 2021 Dec 28.
Acharya P, Mathur M. Association between psoriasis and celiac disease: A systematic review and meta-analysis. J Am Acad Dermatol. 2020;82(6):1376-1385.
National Psoriasis Foundation. Dietary Modifications. Last updated on December 21, 2022.
American Academy of Dermatology Association. What Should I Eat If I Have Psoriasis? Last updated November 11, 2020.





