Updated on July 7, 2025
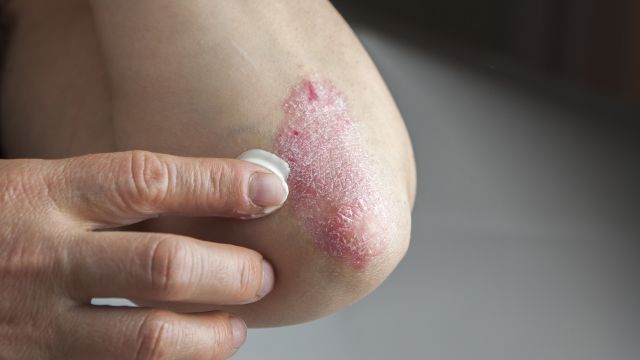
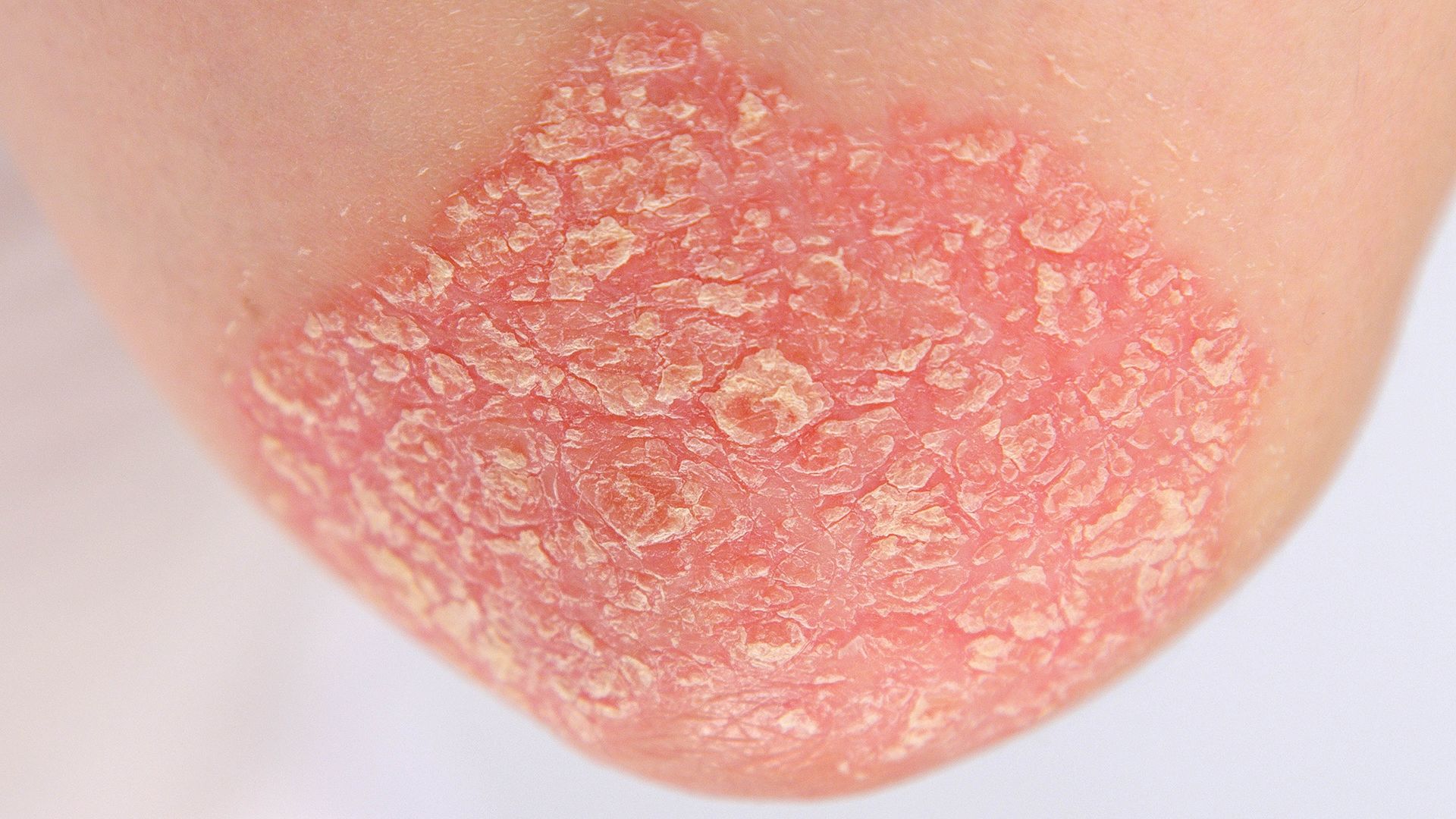
Psoriasis is a chronic inflammatory skin disorder that causes new skin cells to grow at a much faster rate than normal. Most people who have psoriasis have plaque psoriasis, which results in raised patches of discolored, scaled skin (called plaques). The elbows, knees, scalp, lower back, and around the belly button are common areas for plaques to appear. However, psoriasis can affect any and all areas of the body, and different types cause different symptoms.
It is not known why some people have psoriasis and others do not. What is known is that psoriasis occurs because of abnormal immune system activity that causes inflammation in the skin and other areas of the body.
If you are living with psoriasis, learning about inflammation can help you understand what is happening in your skin and the rest of your body, as well as how psoriasis treatments work to reduce inflammation and control symptoms.
Acute inflammation
Inflammation can be categorized as acute or chronic. Acute inflammation is a normal reaction to injury and infection. It occurs when an injury causes damage to cells or an infectious agent (like a virus) enters the body. Immune cells surround the affected area, break down any dead cells or cells that don’t belong, and start building new, healthy cells.
Inflammation is what causes the area around a cut to become discolored and puffy, or why your sinuses become congested when you have a cold. When the cut is healed or the cold resolves, inflammation stops.
Chronic inflammation
While acute inflammation is a necessary, healthy part of healing, chronic inflammation is abnormal and is damaging to the body. It is the result of the immune system causing inflammation in response to things other than injury and infection. It can last months or years and may never entirely go away.
Chronic inflammation is associated with numerous health conditions, including unresolved infections (such as hepatitis C) and autoimmune diseases (where the immune system attacks healthy cells). It is also linked to a variety of risk factors, including older age, stress, sleep problems, obesity, smoking, and eating a diet that contains large amounts of unhealthy fats and added sugars.
While the exact cause of psoriasis remains unidentified, research suggests that the condition occurs as a result of specific genetic mutations that become active when exposed to a trigger. A triggering event could be anything that causes a response by the immune system; injury, infection, drinking too much alcohol, smoking, and stressful events have all been associated with the onset of psoriasis.
Systemic inflammation
When a person has psoriasis, inflammation speeds up the growth of skin cells. While skin cells typically grow and shed over the course of a month, psoriasis causes cells to form over the course of a few days. But the skin is not the only area of the body that is affected when a person has psoriasis. People with psoriasis experience inflammation throughout the body. This is called systemic inflammation.
Systemic inflammation makes people with psoriasis more likely to have other inflammatory conditions, such as psoriatic arthritis and inflammatory bowel disease. It also makes a person more likely to develop illnesses like cardiovascular disease and type 2 diabetes.
Controlling inflammation
There is no cure for psoriasis, but the condition can be managed, and it’s possible for symptoms to go into remission. Therapies used to treat psoriasis work by preventing and/or reducing inflammation. Some medications act directly on the skin, while others act on the immune system to block specific inflammatory cells throughout the body. Lifestyle strategies like eating a healthy diet and avoiding smoking help keep inflammatory triggers from causing psoriasis flares.
Different people respond to different psoriasis treatments. A healthcare provider can guide you through finding the right combination of treatments that works for you.