Rosacea
- What is rosacea?
- What are the signs and symptoms of rosacea?
- What are the types of rosacea?
- What are the stages of rosacea?
- What causes rosacea?
- What are the risk factors for rosacea?
- How is rosacea diagnosed?
- When should you see a healthcare provider?
- How is rosacea treated?
- What are the possible complications of rosacea?
- Can you prevent rosacea?
- What is the outlook for rosacea?
- Living with rosacea
- Featured rosacea articles
Introduction
More than 415 million people around the world have rosacea. This includes around 16 million people in the United States. It tends to occur more often in people assigned female at birth (AFAB) than in people assigned male at birth (AMAB).
Although it is fairly common, the skin disorder isn’t well understood and it may be confused with other common skin conditions such as acne vulgaris (commonly called acne or pimples) or a naturally ruddy complexion (a reddish skin tone or skin that appears mildly sunburned).
Rosacea may be underdiagnosed or go unrecognized in people with darker skin as it may be harder to recognize skin discoloration such as redness or patches of darker skin. For these reasons and others, many people with rosacea don’t receive the care they need to ease symptoms and manage the condition.
Learn about rosacea, what causes it, and how it’s diagnosed. Discover science-backed treatments that can help improve symptoms and boost your overall skin health. And find tips for living better with this lifelong skin condition.
What is rosacea?
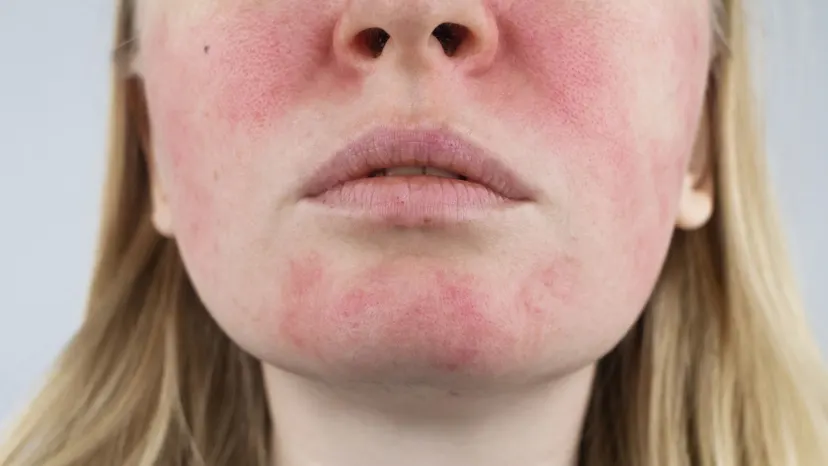
Rosacea (also called acne rosacea) is a chronic but treatable condition that can cause patches of sensitive, red, and inflamed skin. (Note that on darker skin tones, affected skin may appear dusky brown or a darker shade than other areas of skin.) It may also contribute to broken or visible blood vessels and small, pus-filled bumps that appear similar to but aren’t acne vulgaris pimples.
It mainly affects the skin on the central areas of the face, usually starting in the cheeks and spreading to the nose, chin, and forehead. At times, it may also affect the scalp, ears, neck, chest, and back. The eyes can also be affected.
Earlier in the course of the disease, facial redness may sometimes fade. But as the disease progresses, skin discoloration may become more prominent and last for longer periods of time. In some cases, discoloration may become permanent as rosacea can cause small blood vessels (called capillaries) in the face to dilate (expand), allowing for more blood to flow to affected areas.
What are the signs and symptoms of rosacea?
Some rosacea signs and symptoms occur alone while others appear alongside others. These follow a relapsing-and-remitting course, which means that symptom flare-ups (lasting from a few weeks to months) are followed by remission periods when no symptoms are present.
Main rosacea symptoms
The main signs and symptoms of rosacea include:
Red face: Often resembling blushed or sunburned skin, facial redness that persists is the most common sign of rosacea. This may be harder to see in people with darker skin tones, as discoloration may appear dusky brown or a darker shade. People with darker complexions are also more prone to postinflammatory hyperpigmentation (areas of discolored skin) once rosacea skin growths (see below) heal. This can further mask facial redness.
Skin flushing: A common occurrence and early sign of rosacea is facial blushing or flushing for no known reason, which may also be accompanied by a feeling of warmth, heat, or a burning sensation that comes and goes in affected areas.
Skin growths: Small, firm bumps called papules or pus-filled sores called pustules can form just beneath the skin, which can ooze and eventually crust. These may look similar to pimples caused by acne vulgaris, but unlike acne vulgaris, rosacea isn’t associated with excess oil produced by the skin and doesn’t cause blackheads. Instead, rosacea may sting or burn. Over-the-counter (OTC) acne medicines can also make these rosacea symptoms worse.
Telangiectasia (chronic or long-term dilation of capillaries): This occurs in the capillaries around the central areas of the face such as the cheeks and bridge of the nose, leading to persistent discoloration of the skin.
Thickened skin: Over time, excess tissue may cause the skin to grow thicker, especially the skin on the nose (a condition called rhinophyma, a type of phymatous rosacea as described below). This can make the nose appear reddish or discolored and bulbous. Severe rhinophyma can also obstruct airflow through the nasal passageways, making it harder to breathe.
Ocular rosacea: This is rosacea that affects the eyes, which often accompanies rosacea that affects the skin. Ocular rosacea often produces inflamed eyelids. It can cause the eyes to look red and bloodshot. It may also cause:
- Burning
- Conjunctivitis, commonly known as pink eye (inflammation of the thin outer skin of the eye called the conjunctiva)
- Dry eyes
- Crusty or scaly eyelids and eyelashes
- Foreign body sensation (feeling like something’s stuck in the eye)
- Itching
- Light sensitivity
- Tearing
Styes (clinically known as hordeolum) are also more frequent, as rosacea causes inflammation around various areas of the eyes such as the:
- Eyelids
- Conjunctiva (thin, clear membrane that lines and covers the white part of the eyes called the sclera)
- Cornea (clear, dome-shaped outer tissue layer that covers the iris and pupil)
- Pupil (black opening encircled by the iris)
- Sclera
Blood vessels around the eyelid edges may also appear more visible. Left untreated, severe ocular rosacea can damage the cornea and reduce visual acuity (vision clarity and sharpness).
Other rosacea symptoms
Other symptoms may also accompany primary rosacea symptoms, such as:
- Dry, scaly skin: The skin around the affected areas may feel rough and scaly, even though some people with rosacea have oily skin overall.
- Edema (swelling): Edema, particularly around affected areas of the face, may occur alongside or independently of other rosacea symptoms.
- Plaques: Rosacea can also cause these raised, discolored patches to form on the skin.
- Stinging or burning: Affected skin may burn, sting, itch, or feel tight.
What are the types of rosacea?
The four rosacea subtypes defined by the National Rosacea Society include:
Erythematotelangiectatic rosacea (ETR)
ETR can cause persistent redness and flushing of facial skin, which may occur with or without telangiectasia (prominent blood vessels just beneath the skin). Left untreated, ETR can spread beyond the face and become permanent. In a 2022 review and analysis of studies published in JAMA Dermatology, nearly 57 percent of the more than 9,000 people included had this rosacea subtype.
Papulopustular rosacea (PPR)
Slightly more than 43 percent of people included in the 2022 JAMA Dermatology review had this rosacea subtype. With PPR, papules or pustules form on the skin, which may occur with or without ETR. Often mistaken for pimples caused by acne vulgaris, these skin blemishes tend to form on the central areas of the face such as the cheeks, chin, and forehead but may also spread to other areas such as the neck, scalp, back, or chest. Up to 40 slow-healing PPR blemishes may be present at a given time.
Ocular rosacea
Just over 11 percent of people included in the 2022 JAMA Dermatology analysis had this rosacea subtype. It can lead to a number of eye health issues such as one that causes inflammation of the eyelids called blepharitis. Ocular rosacea can occur with or without visible symptoms that affect the skin.
Phymatous rosacea (PhR)
More than 7 percent of people included in the 2022 JAMA Dermatology analysis had phymatous rosacea. This somewhat rare rosacea subtype tends to affect people assigned male at birth (AMAB) more often than people assigned female at birth (AFAB). It causes the skin to grow thicker, making it look and feel bumpy and swollen. Scarring and skin discoloration may also occur. Rhinophyma, which causes a bulbous nose, is the most common PhR type.
What are the stages of rosacea?
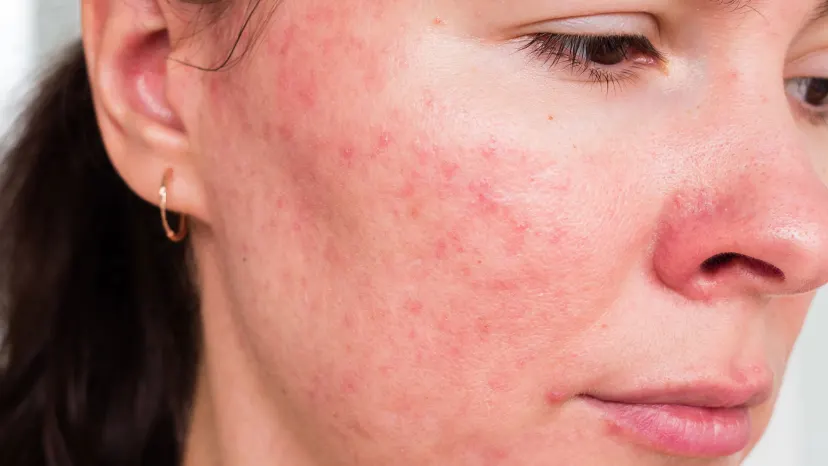
Rosacea tends to occur in stages or phases, which produce symptoms that remit and relapse and range from mild to severe. Although these phases tend to occur in sequence, some people may bypass earlier phases (phase 1 and 2) and go straight to the inflammatory phase (phase 3) of rosacea. With proper treatment, some may return to an earlier rosacea phase and keep from progressing to the late stage (phase 4) of the disease.
Phase 1: Pre-rosacea phase
Temporary bouts of flushing, blushing, and sometimes stinging of the skin, particularly across the cheeks and nose, may occur during this phase. Facial redness or dusky brown discoloration tends to subside with time.
Phase 2: Vascular rosacea phase
Long-term capillary dilation may cause flushing and facial redness or discoloration that can persist after the rosacea trigger (see below) is no longer present or active. Telangiectasia (prominent blood vessels) may also be visible.
Phase 3: Inflammatory rosacea phase
Papules or pustules may form during this phase. Facial redness or discoloration may persist even longer than earlier phases and telangiectasia may be more pervasive in areas that are flushed.
At this stage, severe damage to blood vessels can lead to permanent dilation of affected capillaries, causing chronic inflammation. These changes can also trigger formation of new blood vessels, which also allow more blood to flow to affected areas. Facial swelling may also occur as fluid and proteins leak out of broken capillaries into the skin.
Phase 4: Late rosacea phase
By this stage, rosacea symptom flare-ups have likely grown severe. Intense and extended bouts of facial flushing due to widespread damage of facial capillaries are often accompanied by severe swelling, profound facial pain, tissue overgrowth, and burning or stinging sensations that can feel debilitating. Many papules or pustules may be present and phymatous rosacea, particularly rhinophyma, may have set in as well.
What causes rosacea?
The precise cause of rosacea isn’t clear, but research points to various factors. These might include factors acting alone or in combination with others, such as:
Environmental exposure may contribute to rosacea
This might include too much exposure to ultraviolet (UV) light such as from sunbathing outdoors or using indoor tanning beds.
Genetics may contribute to rosacea
Some people may inherit certain gene mutations that make them more prone to rosacea. Rates of rosacea tend to be higher among people with closely related blood relatives (such as a parent or sibling) with the condition.
Researchers have identified various human leukocyte antigen (HLA) gene mutations that may play a role in the development of rosacea. These are part of a gene family that code for a group of proteins called the HLA complex, which play a significant role in the body’s immune response. These same HLA gene mutations have also been tied to several autoimmune diseases, including type 1 diabetes and celiac disease.
Infection may cause rosacea
Rosacea may also have links to digestive health. For instance, a type of bacteria that lives in the gut called Helicobacter pylori (H. pylori) may affect more than half of the world’s population, sometimes causing long-term or persistent infections.
H. pylori is known to cause multiple health issues such as stomach ulcers, stomach cancer, and possibly pancreatic cancer. It’s also implicated in the development of various skin disorders along with rosacea such as psoriasis and urticaria (hives).
Because gut bacteria can influence functions within the body such as inflammation, immune regulation, and vasodilation (blood vessel expansion), scientists suspect that H. pylori may cause rosacea symptoms such as skin flushing and inflammation.
The connection between gut bacteria and rosacea is further supported by a 2023 study published in Advanced Biomedical Research, which concluded that treatment and eradication of H. pylori may improve rosacea symptoms. Although the study was small, nearly 64 percent of the 60 participants with rosacea experienced remission after the bacterial infection was cleared.
Malfunction of the skin barrier may contribute to rosacea
Ordinarily, the outer layer of your skin, known as the skin barrier, serves as a shield against potentially harmful agents in the environment. But in some people with rosacea, the function of the skin barrier may be disrupted or the barrier itself may be compromised. This can lead to dry, scaly skin or skin that burns or becomes more sensitive and easily irritated—all of which can make the skin more prone to rosacea.
Microbiome changes may contribute to rosacea
People may also be more prone to rosacea due to changes in the microbiome (the community of microbes such as bacteria, fungi, and viruses that live in various parts of the body like the skin and gut). For instance, a certain number of Demodex skin mites (both D. folliculorum and D. brevis) naturally live on areas of the skin including the hair follicles of the face.
Rosacea may be more likely to occur when people have excess numbers of these skin mites or are overly sensitive to the bacteria they carry, Bacillus oleronius. It isn’t clear, however, whether rosacea results from excess Demodex mites on the skin or if rosacea causes the increase in these skin mites.
Other bacteria, such as Cutibacterium acnes and Staphylococcus epidermidis, have also been implicated in the development of rosacea.
Overactive blood vessels may contribute to rosacea
Some people with rosacea may have overactive capillaries in the face and other affected areas, which may lead to greater dilation of these blood vessels. This may occur in response to external triggers that cause the release of brain chemicals that play a role in blood vessel dilation, such as substance P, pituitary adenylate cyclase-activating peptide, and calcitonin gene-related peptide. In turn, increased blood flow to these areas can cause a red face or patches of darker or dusky brown skin and other rosacea symptoms.
What are the risk factors for rosacea?
One or more of the following characteristics may raise the risk for rosacea:
Age: Rosacea is most often diagnosed in adults between 30 and 50 years old.
Family medical history: People with a family history of rosacea or severe acne vulgaris (such as cystic or nodular acne, which develop deep in the skin and cause pain) are more likely to develop rosacea themselves.
Personal medical history: Rosacea is also more likely to develop in people with a history of severe acne vulgaris, including those who have had acne nodules and cysts.
Race/ethnicity: Rosacea most often affects people with fair skin, and more than 10 percent of white people have the skin condition. Many people who have rosacea are of Celtic or Northern and Eastern European descent.
The condition can also occur in people with darker skin, but some studies have found disparities in diagnosis. Some rosacea symptoms, such as flushed skin, may be masked in people with darker complexions, as their skin may not appear red when this occurs. Rather, it may appear a darker shade.
Sex assigned at birth: Rosacea occurs more often in people assigned female at birth (AFAB) compared to people assigned male at birth (AMAB).
What can trigger rosacea?
Rosacea symptoms may also flare up due to certain triggers. Because these can vary for each person, one way to pinpoint your triggers is to start a rosacea diary.
Track when symptoms flare up, noting details such as your diet, emotions, activities, and weather at the time these symptoms appear. Also jot down how intense these symptoms feel and how long each of them last.
Common rosacea triggers include:
Sun exposure can trigger rosacea
Of all the potential triggers for rosacea, sun exposure is the most common. Being exposed to the UV rays of the sun for even a few minutes can trigger rosacea symptoms such as skin flushing.
Drugs may trigger or exacerbate rosacea symptoms
These might include vasodilators (drugs that expand blood vessels) such as some blood pressure medications. Using topical steroids on the skin for too long may also lead to rosacea flare-ups. But the risk of this happening is low when this medication is used properly, which often entails using the lowest effective dose for the shortest duration possible. Other examples of medicines that can aggravate rosacea symptoms include some used to treat anxiety, glaucoma, and migraines.
Foods and beverages may trigger or exacerbate rosacea symptoms
It’s best to work with your healthcare provider (HCP) or registered dietitian nutritionist (RDN) to confirm or rule out your trigger foods. An RDN can also help you come up with an eating plan that allows you to eat foods that nourish your body and support healing (such as from papulopustural breakouts) without triggering flare-ups.
Types of foods and drinks that might trigger a rosacea flare-up include:
- Spicy and hot foods
- Drinks such as hot coffee and tea
- Fermented foods like sauerkraut
- Foods high in niacin (found in many animal and plant sources such as poultry, beef, fish, nuts, legumes, and grains)
- Foods high in histamine (a chemical released by the immune system that triggers inflammation and is found in foods such as cured and air-dried meat products)
Specific foods that can trigger rosacea flare-ups include:
- Alcohol
- Avocados
- Bananas
- Broad-leaf beans and pods, like peas and lima and navy beans
- Cheese, with the exception of cottage cheese
- Chocolate
- Citrus fruits such as grapefruits, lemons, and oranges
- Eggplant
- Fatty fish like anchovies, herring, salmon, sardines, mackerel, and tuna
- Figs
- Liver
- Raisins
- Red plums
- Sour cream
- Soy sauce
- Spinach
- Tomatoes
- Vanilla
- Vinegar
- Yeast extract (although bread may be fine)
Emotions may trigger or exacerbate rosacea symptoms
These include persistent or profound emotions such as:
- Anger
- Anxiety, including social anxiety that causes people to blush when they feel embarrassed
- Shame or guilt
- Stress
Health-related issues may trigger or exacerbate rosacea symptoms
Being more prone to frequent skin flushing may trigger rosacea flare-ups, as can having a fever, cold, chronic or persistent cough, high blood pressure, caffeine withdrawal, or going through menopause.
Physical activity may trigger or exacerbate rosacea symptoms
These can include activities that cause the body temperature to rise and blood vessels to dilate, such as cardio exercise or activities that require heavy lifting.
Irritating substances may trigger or exacerbate rosacea symptoms
These might include cosmetic, skin, hair, hygiene, and cleaning products that can irritate the skin or cause it to sting, burn, or become inflamed. These irritating ingredients may include:
- Acetone
- Alcohol
- Camphor
- Eucalyptus
- Fragrances
- Fruit, glycolic, or lactic acids
- Menthol
- Mint
- Sodium lauryl sulfate
- Urea
- Witch hazel
Excessive heat may trigger or exacerbate rosacea symptoms
Overheating or exposure to excessive heat may trigger or exacerbate a rosacea flare-up. In addition to hot flashes that may occur before, during, and after menopause, this might include being in a hot environment or climate, taking a hot bath, or sitting in a sauna or jacuzzi for too long. Furthermore, prolonged exposure to extreme heat can take a toll on mental and emotional health, which can also trigger or exacerbate rosacea symptoms.
Weather extremes may trigger or exacerbate rosacea symptoms
In addition to hot temperatures, other weather extremes such as high humidity, strong winds, and frigid temperatures can also lead to flare-ups or make them worse. For instance, windburn can trigger a rosacea flare-up just as easily as a sunburn.
How is rosacea diagnosed?
A clinical diagnosis of rosacea is made by your healthcare provider (HCP). Lab and other tests aren’t used to confirm the diagnosis, although they may be ordered to rule out other conditions with similar symptoms such as various types of psoriasis, eczema (including a type of eczema called seborrheic dermatitis), lupus, and sarcoidosis (an inflammatory disease of the immune system). Instead, your HCP will likely talk with you about your symptoms, personal and family medical history, current medications, and work and lifestyle factors.
This will likely include a discussion of when you first noticed possible rosacea symptoms. Your HCP will ask if these tend to come and go and if you’re aware of specific triggers that make your symptoms worse.
Your HCP may also ask whether you’re frequently exposed to the sun because of your job or lifestyle. Although a red face or darkened skin and visible capillaries may be caused by damage from UV rays, it may also be due to rosacea in some cases.
A skin examination usually follows, during which your HCP will look for features of rosacea such as:
- Dilated, prominent, or broken capillaries
- Facial redness or discoloration, flushing, and swelling
- Papules, pustules, and/or reddish to brownish scaly skin patches on your face
- Thickened skin, including rhinophyma (red, bulbous nose)
- Watery, red, and bloodshot eyes, which may also appear crusty or scaly
Your primary HCP might also refer you to a dermatologist, a medical doctor who specializes in diagnosing and treating skin conditions. If you have signs and symptoms of ocular rosacea, especially if they are severe or they impair your vision, you’ll likely be referred to an ophthalmologist, a medical doctor who specializes in diagnosing and treating eye conditions.
When should you see a healthcare provider?
It’s best to consult with your HCP if you notice any possible signs or symptoms of rosacea, especially if these persist, are severe, or flare up after you are exposed to certain triggers.
What questions should you ask your healthcare provider?
If you’ve been diagnosed with rosacea, be sure to ask an HCP such as your primary care doctor or dermatologist any questions you have about the condition. These might include:
- How do you know I have rosacea? What factors led to your diagnosis?
- Which rosacea treatment options might work best for me? What are the risks and benefits of each treatment?
- How long will I need to take these treatments? How long do their effects last?
- Can my rosacea symptoms get better without treatment?
- How do I prevent rosacea flare-ups and keep my condition from getting worse?
- Are there any lifestyle interventions you’d recommend to complement my medical treatment plan?
- Which skincare routine would you recommend for me?
How is rosacea treated?
Although there isn’t a cure for the skin condition, various rosacea treatments can help manage symptoms and flare-ups. These include:
Topical medications to treat rosacea
Topical medications are applied on the skin to help treat mild to moderate rosacea symptoms. These include:
Antibiotics: These may reduce inflammation and papulopustular rosacea (PPR) breakouts, helping the skin appear less red (or discolored) and swollen. Examples of antibiotics used to treat rosacea include:
- Benzoyl peroxide
- Clindamycin
- Erythromycin
- Metronidazole
- Minocycline
- Sulfas
Azelaic acid: Available as an OTC or prescription cream, foam, or gel, azelaic acid is part of a drug class called dicarboxylic acids. It’s a naturally occurring byproduct of the yeast Malassezia furfur (also known as Pityrosporum ovale) found in grains such as barley, rye, and wheat.
Azelaic acid may help ease redness and PPR blemishes. It can cause side effects such as itchy, dry skin, which tend to subside with continued use.
Brimonidine gel or oxymetazoline cream: These are part of a drug class called alpha-adrenergic agonists, which help reduce facial flushing and redness by temporarily constricting (narrowing) blood vessels under the skin.
Ivermectin cream: This medicine is part of a class of drugs called anthelmintics, which help treat infections caused by parasites such as Demodex mites.
Retinoids: Derived from vitamin A, retinoids such as tretinoin and adapalene can help prevent and treat papules and pustules caused by rosacea. In some people with rosacea, these medicines can irritate the skin. However, once rosacea is under control, applying a retinoid can help prevent flare-ups.
They also help reduce fine lines and wrinkles and improve skin tone by boosting collagen production and the rate at which cells on the surface of the skin regenerate.
Sodium sulfacetamide/sulfur: This is a combination of an antibiotic called sodium sulfacetamide (a type of sulfa antibiotic) and the keratolytic (peeling agent) sulfur. It helps prevent and treat papules, pustules, and rough, scaly skin caused by rosacea.
Oral medications to treat rosacea
Oral antibiotics may be prescribed to treat moderate to severe PPR and ocular rosacea. They can help clear PPR blemishes and ease redness and swelling.
For instance, your HCP might prescribe a low dose of a specific antibiotic to keep the dose below the antibiotic threshold, which means the medicine isn’t potent enough to stop bacterial growth but it can still decrease inflammation caused by rosacea. These low antibiotic doses can be prescribed for long-term use without raising the risk for antibiotic resistance.
Examples of oral antibiotics used to treat rosacea symptoms include tetracycline antibiotics such as doxycycline, minocycline, and tetracycline and macrolide antibiotics such as azithromycin and erythromycin. Some (such as doxycycline and tetracycline) may be used to treat inflammation caused by phymatous rosacea (PhR).
Blood pressure medications to treat flushing
Certain blood pressure medications may also be prescribed to reduce facial flushing, although the effects of these medicines occur throughout the body and aren’t limited to the face. Examples include carvedilol, clonidine, and propranolol.
Isotretinoin to treat rosacea
Isotretinoin may help treat papules and pustules. It may also help reduce inflammation caused by PhR. Isotretinoin belongs to a drug class called retinoids, which are derived from vitamin A.
More commonly known by and previously sold under the brand name Accutane, the retinoid is now only prescribed as generic oral isotretinoin. Because of the risk of severe side effects, such as liver toxicity and birth defects, this medication is usually considered only if other rosacea treatments aren’t effective.
The medication may be prescribed for a few weeks to months, but your HCP will likely follow up with you each month or as often as needed to assess how well it’s working and to determine whether to proceed with treatment. Blood tests are often required to help monitor side effects such as liver toxicity.
Because the medication carries a serious risk of birth defects, people prescribed isotretinoin in the U.S. must register with the U.S. Food and Drug Administration’s iPLEDGE Risk Evaluation and Mitigation Strategy (REMS) program prior to filling the prescription. People assigned female at birth (AFAB) must also agree to use birth control while being treated with this medicine.
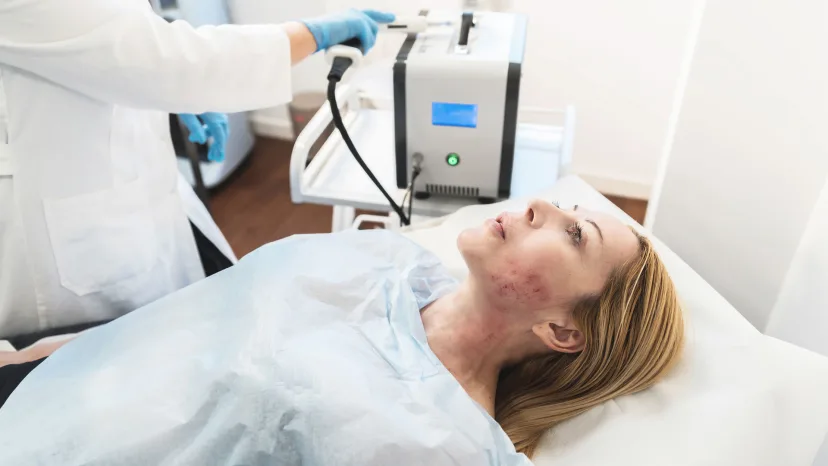
Laser therapy for rosacea
Your HCP may recommend laser therapy to help:
- Decrease the size and appearance of visible capillaries
- Ease redness and swelling
- Lighten scars
- Remove thickened outer layers of skin caused by PhR, such as rhinophyma
These rosacea treatments may be ablative or non-ablative. Ablative lasers remove the top and thinnest layer of skin called the epidermis. Non-ablative lasers heat up the middle and thickest layer of skin called the dermis without heating the epidermis, thereby keeping this outermost layer cool and intact.
While ablative lasers tend to produce more noticeable results with fewer treatment sessions, some people may opt to go with non-ablative therapies as these generally require less recovery time and carry a lower risk of side effects such as itching, discoloration, tightness, and pain in treated areas of the skin. Lasers can also burn or scar the skin.
Examples of laser and light devices used to treat rosacea include:
Carbon dioxide (CO2) laser: This ablative laser is used to diminish scarring and remove layers of thickened skin caused by phymatous rosacea, including rhinophyma. CO2 lasers resurface or reshape skin by cutting out or evaporating affected tissue layers.
Erbium laser: Examples of these laser types include erbium-doped yttrium-aluminum-garnet (Er:YAG) and neodymium:YAG (Nd:YAG). Erbium lasers may be ablative or non-ablative.
They help rearrange the skin’s connective tissue, a process known as collagen remodeling. This may help improve skin texture, firmness, and structure while helping to diminish scarring and skin discoloration. Erbium lasers may also help improve the appearance of visible blood vessels and remove excess tissue caused by PhR.
Intense pulse light (IPL) therapy: A less aggressive form of therapy compared to ablative lasers, this non-ablative therapy uses multiple wavelengths of light to stimulate collagen production and help heal wounds, unlike other laser devices which often use a single, focused laser. IPL may help with skin discoloration and scarring caused by rosacea.
Pulsed dye laser (PDL): This non-ablative treatment uses organic dyes to create an array of laser beam colors, which produce varying wavelengths of light depending on the dye used. PDL converts light into heat energy, which is absorbed by oxyhemoglobin (oxygen bound to the hemoglobin protein in red blood cells) to reduce facial discoloration and flushing caused by erythematotelangiectatic rosacea (ETR).
The heat from PDL lasers also destroys damaged blood vessels while helping to reduce the formation of new blood vessels. The body then absorbs damaged blood vessels and reroutes the flow of blood through undamaged blood vessels.
Potassium titanyl phosphate (KTP) laser: Like PDL, this is a non-ablative laser that’s mainly absorbed by oxyhemoglobin in blood, thus minimizing damage to surrounding structures and tissue. An Nd:YAG laser is used to illuminate a KTP crystal to create a green laser beam, which passes through the skin to penetrate, shrink, or destroy damaged blood vessels, reduce redness, discoloration, and flushing caused by ETR, and inhibit the formation of new blood vessels.
Laser therapy for darker skin
Various laser and light therapies, such as those noted above, may be used to treat rosacea in people with darker skin. A more conservative approach, including the use of lower settings, is often employed to minimize the risk of scarring and postinflammatory hyperpigmentation (in which skin becomes darker after treatment).
Surgery for rosacea
Electrosurgery involves trimming down excess tissue caused by phymatous rosacea (PhR) with the help of a thin wire that has a weak electrical current running through it. Placing the current directly on affected blood vessels can cause them to shrink, clot, and form small scabs that heal within a few days.
Severe PhR may require surgical resection (removal) of excess skin. This is likely the case with severe rhinophyma, especially if it obstructs breathing.
Dermabrasion for rosacea
Severe PhR may also be treated with dermabrasion. This procedure involves the use of a rapidly rotating device equipped with an abrasive metal head to effectively sand off (or abrade) the top layers of affected skin. The procedure aims to produce a smoother layer of new skin once the abraded skin heals. In the case of rhinophyma, dermabrasion may help shave off extra layers of skin to sculpt the nose closer to its former shape.
Ocular rosacea treatment
Conservative (or non-surgical) management of ocular rosacea may entail:
- Clearing the crusts, scales, and oils around the eyelids and lash line with clean cotton swabs dipped in a gentle cleansing solution (like a few small drops of unscented baby shampoo mixed with a cup of warm water)
- Applying warm compresses to closed eyelids
- Using artificial tears (eye drops) to lubricate and ease dry eyes
- Avoiding contact lens use if the eyes are irritated, inflamed, or infected
- Taking omega-3 fatty acid supplements as recommended by your HCP. These have been reported to help with dry, inflamed eyes along with helping to prevent facial redness or discoloration, flushing, and inflammation caused by erythematotelangiectatic rosacea.
If needed, ocular rosacea may also be treated with:
- Topical antibiotics such as azithromycin, bacitracin, erythromycin, fusidic acid, metronidazole, or polymyxin B
- Oral antibiotics, including tetracyclines like doxycycline, macrolides like erythromycin, or antibiotics like flucloxacillin to treat styes (as the infection is most often caused by the Staphylococcus aureus bacteria)
- Topical nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen
- Topical steroids (a short course is usually prescribed, as long-term use may raise the risk of eye diseases such as cataracts and glaucoma)
- Topical calcineurin inhibitors such as ciclosporin (an immunosuppressant medication), if ocular rosacea hasn’t improved with topical steroids
- Oral isotretinoin, which may be taken in low doses to reduce the risk of adverse effects, including infections, dry eye, and other issues that affect the eyes
- Surgery to remove styes that don’t get better with warm compresses or antibiotics
- Keratoplasty, which is surgery to repair corneal perforation (tear) or opacification (scarring). These may be caused by rosacea keratitis, a condition that leads to inflammation of the cornea.
What are the possible complications of rosacea?
Without proper treatment, rosacea can cause permanent scarring, thickened skin (in the case of phymatous rosacea, including rhinophyma), and a range of eye conditions associated with ocular rosacea, such as:
- Blepharitis: Inflammation of the eyelid edges
- Chalazion: A lump or cyst in the eyelid, which tends to be caused by blocked and inflamed oil glands
- Conjunctival injection: Dilation and inflammation of the blood vessels that flow through the conjunctiva. The condition is also known as conjunctival hyperemia or bloodshot eyes.
- Conjunctival telangiectasias: Dilation of the tiny blood vessels that supply the conjunctiva, making these blood vessels appear more prominent
- Conjunctivitis (pink eye): Inflammation of the conjunctiva
- Iritis: Also called anterior uveitis, this causes Inflammation of the iris.
- Keratitis: Also referred to as a corneal ulcer (open sore), this condition is caused by inflammation of the cornea.
- Scleritis: Inflammation of the sclera
- Stye: An infection and inflammation that often starts at the root of an eyelash
Can you prevent rosacea?

Since the exact cause of rosacea is unknown, there’s no foolproof way to prevent it. But pinpointing your rosacea symptom triggers and avoiding them may help keep flare-ups at bay. If you don’t know which triggers affect you, work with your HCP to figure these out safely. The National Rosacea Society also provides a free diary you can download and print to track your rosacea triggers.
In addition to following your rosacea treatment plan and adjusting it as needed with guidance from your HCP, these recommendations from the American Academy of Dermatology Association (AAD) might help prevent flare-ups:
Protect your skin from the elements
Be sure to protect your skin from the sun, wind, and cold. This may include these steps:
Apply a gentle sunscreen: Apply a fragrance-free, broad-spectrum sunscreen with an SPF of 30 or higher before going outdoors, and reapply as needed. Note that “fragrance-free” and “unscented” aren’t the same thing. (A “fragrance-free” product does not contain chemical fragrances or masking scents. An “unscented” product may contain chemicals that mask the odors of other ingredients.)
Look for one that contains silicone (sometimes listed as dimethicone, cyclomethicone, or orcyclomethicone). This ingredient creates a barrier-like coating over the skin to bolster UV protection and improve water resistance. Choose a sunscreen that has physical blockers like zinc oxide, titanium dioxide, or both, as these are less likely to irritate rosacea-prone skin compared to chemical screens.
Don a wide-brimmed hat: Wear your hat anytime you’re outdoors during the day.
Seek shelter and shade: Try to stay out of the midday sun, as this is when the sun’s UV rays are strongest. While outdoors during the day, try to spend most of your time in a shady or covered area.
Cover your face with a scarf in windy or cold weather: Cover much of your face, except for your eyes, with a silk or acrylic scarf. Stay away from rough, irritating fabrics (such as wool), as these may trigger a rosacea flare-up.
Use gentle cosmetic and hygiene products and methods
Work with an HCP such as a dermatologist to create or modify your rosacea skin care plan. This might include:
- Carefully reviewing the ingredients in skin, hair, hygiene, and cosmetic products and avoiding ones that contain irritating substances that are likely to trigger a flare-up
- Testing these products by dabbing a small sample of it near the areas of your skin affected by rosacea, making sure not to use it again if irritation occurs within 72 hours
- Staying away from facial toners and astringents
- Moisturizing your skin daily (or as recommended by your HCP) with a gentle, fragrance-free emollient or barrier-repair cream (instead of a lotion or gel)
- Applying this gentle emollient cream to your skin before applying any cosmetics
- Using a gentle and lightweight liquid foundation that’s easy to spread and wash off (instead of a heavy, thick, or waterproof foundation that may require makeup remover to take off)
- Shaving with an electric razor (instead of a dull razor blade), using a gentle, fragrance-free shaving cream or lotion that doesn’t irritate your skin. After shaving, apply a soothing, fragrance-free balm or moisturizer to your skin instead of a harsh aftershave.
Be sure to gently wash your face twice daily with a mild, fragrance-free cleanser (not soap), following these steps:
- Use your fingertips to gently apply the cleanser to your skin, moving your fingers in a circular motion around your face. Be sure not to scrub or rub your skin or use sponges, washcloths, or exfoliating devices.
- Rinse the cleanser off your face thoroughly with lukewarm water and your fingertips.
- Gently pat your face dry with a clean, cotton towel.
Dial down the body heat
Bringing your body temperature down and avoiding overheating can also reduce rosacea flare-ups:
- Dress in layers, taking off extra clothing as needed if you start to feel too hot.
- Place a cold, wet compress or cloth against areas with large blood vessels such as your neck, armpits, or groin area.
- Sip cold or cool beverages.
- Turn on the air conditioner or fan, if available.
- If a heating device such as a space heater or fireplace is on, sit far enough away from it so that you don’t feel the heat directly.
Stay cool when working out
The following tips may help keep you from overheating and experiencing a flare-up during your workout:
- Go low-intensity. You can still get an effective workout with low- or medium-intensity workouts such as barre, walking, or yoga.
- Work out in a cool environment. Exercise in an air-conditioned environment or under a shady area or path during the coolest time of day.
- Let the waters cool you. Try water aerobics or go for a swim in an indoor or covered pool in which the water feels cool (not heated).
- Keep cooling and hydration supplies nearby. This includes drinking from a bottle filled with ice water and dabbing a clean towel dipped in cold water around your face and body and draping it around your neck. An ice pack or ice cubes wrapped in a clean cloth may also be helpful.
Avoid your food triggers
Although you may be more sensitive to certain types of foods, this doesn’t mean you have to avoid them altogether unless you’re certain they contribute to your flare-ups. Start by tracking your foods or keeping a diary of your diet and noting when your condition flares up.
Share your food diary with your HCP or RDN. They can work with you to safely determine which of these foods are triggers you’ll need to avoid.
Cool your beverages
Stay away from hot drinks such as hot coffee or tea. Drink them iced or let them cool down to a lukewarm temperature before taking your first sip.
Avoid alcohol
Rosacea symptoms such as facial flushing may be triggered by drinking alcohol. If you drink, it’s therefore a good idea to:
- Limit the amount of alcohol you consume.
- Add club soda or seltzer to your beverage to dilute the alcohol.
- Don’t drink alcohol on an empty stomach.
- Drink a large glass of cold water after you finish your drink.
You can also choose not to drink alcohol at all, as this is the only way to fully eliminate this trigger.
Go with less spice
Spicy foods can also trigger rosacea symptoms such as facial flushing. If you like spicy foods, opt for mild versions of these.
If you have a taste for ghost-pepper chicken wings or habanero salsa, try going with less spicy flavors that still satisfy your palate. If your rosacea symptoms continue to flare up even after you tone down the spice, it’s likely best to avoid spicy foods altogether.
Manage stress
Find healthy ways to relieve your stress. Whether this entails taking slow, deep breaths during stressful moments, practicing tai chi or meditation, or engaging in carefree play, it can help to find a meaningful outlet for your stress that brings you joy and helps you relax and unwind.
Discuss your medicines with your healthcare provider
Review your current medication list with your HCP to see if any of them could be a potential trigger. This includes going over all dietary supplements, herbs, and essential oils you take or use, as some (such as vitamin B3, also known as niacin) may cause rosacea flare-ups.
If you suspect one of your medicines or supplements could be a trigger, don’t stop taking them without speaking with your HCP first. If a medication is triggering your rosacea, your HCP may be able to prescribe or recommend a different formula or supplement.
What is the outlook for rosacea?
Rosacea is a chronic condition, with symptoms that come and go in an unpredictable pattern. Your skin’s appearance may change over time and new symptoms may develop as the disease progresses. A cure for rosacea has yet to be discovered, but staying away from triggers and following a comprehensive and personalized treatment plan can help prevent and ease flare-ups and the complications associated with the disorder.
Rosacea doesn’t affect everyone in the same manner and it often takes time and effort to figure out the best treatment plan and lifestyle strategies to manage your condition. To improve outcomes and quality of life, it’s best to start treatment as early as possible instead of waiting until symptoms become severe.
Living with rosacea

Rosacea can take a toll on one’s mental health beyond its physical impact. Constantly needing to avoid triggers can limit activities and lifestyle. Over time, the stress of living with the disorder can raise the risk of or worsen mental health issues such as anxiety and depression.
In fact, rates of anxiety and depression may be at least twice as high among people with rosacea as those without, according to a 2021 review and analysis of studies published in Dermatology and Therapy. Of the more than 14,000 people included in the analysis, nearly 20 percent of those with rosacea experienced depression while more than 15 percent experienced anxiety.
Anxiety and depression commonly occur among people with skin disorders such as psoriasis and atopic dermatitis, the most common type of eczema. The physical manifestations of rosacea (such as a flushed face, papular and pustular breakouts, and rhinophyma) can impair body image and decrease self-esteem. It can also lead to social isolation, as some people may minimize or avoid interactions with others due to feeling stigmatized or embarrassed of how they look.
Mind your mental health
If the emotional weight of living with rosacea feels like it’s too much to bear, know you’re not alone. Reach out to people you trust for support. This might be a close family member, friend, or spiritual advisor.
Seeking counseling from a licensed mental health provider may also be helpful. Joining an in-person or online support group can also help you find support from others living with rosacea.
Featured rosacea articles

Aghaei M, Aghaei S, Behshadnia F, et al. Association between the treatment of rosacea and eradication of Helicobacter Pylori infection. Adv Biomed Res. 2023;12:173.
American Academy of Dermatology Association. 6 Rosacea Skin Care Tips Dermatologists Give Their Patients. Accessed August 28, 2023.
American Academy of Dermatology Association. How to Prevent Rosacea Flare-Ups. Accessed September 6, 2023.
American Academy of Dermatology Association. Lasers and Lights: How Well Do They Treat Rosacea? Accessed September 6, 2023.
American Academy of Dermatology Association. People With Darker Skin Tones Can Get Rosacea. Last updated January 11, 2023.
American Academy of Dermatology Association. Retinoid or Retinol? Accessed September 25, 2023.
American Academy of Dermatology Association. Rosacea: Diagnosis and Treatment. Accessed September 6, 2023.
American Academy of Dermatology Association. Rosacea Treatment: Eye Problems. Accessed September 8, 2023.
American Academy of Family Physicians. Rosacea. familydoctor.org. Last updated January 29, 2021.
Barakji YA, Rønnstad ATM, Christensen MO, et al. Assessment of frequency of rosacea subtypes in patients with rosacea: A systematic review and meta-analysis. JAMA Dermatol. 2022;158(6):617-625.
Cedars-Sinai. Rosacea. Accessed August 8, 2023.
Cices A, Alexis AF. Patient-focused solutions in rosacea management: Treatment challenges in special patient groups. J Drugs Dermatol. 2019;18(7):608-612.
Cleveland Clinic. Rosacea. Last reviewed April 12, 2023.
Dai R, Lin B, Zhang X, Lou Y, Xu S. Depression and anxiety in rosacea patients: A systematic review and meta-analysis. Dermatol Ther (Heidelb). 2021;11(6):2089-2105.
Daou H, Paradiso M, Hennessy K, Seminario-Vidal L. Rosacea and the microbiome: A systematic review. Dermatol Ther (Heidelb). 2021;11(1):1-12.
Dick MK, Patel BC. Rhinophyma. StatPearls [Internet]. Last updated August 8, 2023.
Drake L. Exercise. National Rosacea Society. Accessed September 6, 2023.
Farshchian M, Daveluy S. Rosacea. StatPearls [Internet]. Last updated August 8, 2023.
Guarneri C, Ceccarelli M, Rinaldi L, Cacopardo B, Nunnari G, Guarneri F. Helicobacter pylori and skin disorders: A comprehensive review of the available literature. Eur Rev Med Pharmacol Sci. 2020;24(23):12267-12287.
Hu XM, Li ZX, Zhang DY, et al. Current research and clinical trends in rosacea pathogenesis. Heliyon. 2022;8(10):e10874.
Hrubisko M, Danis R, Huorka M, Wawruch M. Histamine intolerance—The more we know the less we know. A review. Nutrients. 2021;13(7):2228.
Institute for Quality and Efficiency in Health Care (IQWiG). Rosacea: Overview. InformedHealth.org [Internet]. Last updated September 10, 2020.
Johns Hopkins Medicine. Rosacea. Accessed August 28, 2023.
Keri JE. Rosacea. Merck Manual Consumer Version. Last updated September 2022.
Keri JE. Rosacea. Merck Manual Professional Version. Last updated September 2022.
Kunovsky L, Dite P, Jabandziev P, et al. Helicobacter pylori infection and other bacteria in pancreatic cancer and autoimmune pancreatitis. World J Gastrointest Oncol. 2021;13(8):835-844.
Kuo A. Rosacea. DermNet. Last updated March 2022.
Li Y, Wang R. Efficacy comparison of pulsed dye laser vs. microsecond 1064-nm neodymium:yttrium-aluminum-garnet laser in the treatment of rosacea: A meta-analysis. Front Med (Lausanne). 2022;8:798294.
Maliyar K, Abdulla SJ. Dermatology: How to manage rosacea in skin of colour. Drugs Context. 2022;11:2021-11-1.
National Institute of Arthritis and Musculoskeletal and Skin Diseases. Rosacea. Last reviewed May 2021.
National Institutes of Health Office of Dietary Supplements. Niacin Fact Sheet for Health Professionals. Last updated November 18, 2022.
National Rosacea Society. Coping With Common Rosacea Triggers. Accessed September 7, 2023.
National Rosacea Society. Coping With Rosacea. Accessed August 28, 2023.
National Rosacea Society. Coping With Rosacea: Identifying Your Individual Rosacea Triggers. Accessed August 28, 2023.
National Rosacea Society. Factors That May Trigger Rosacea Flare-Ups. Accessed September 6, 2023.
National Rosacea Society. For Men: Shaving Tips for Skin With Rosacea. Accessed September 8, 2023.
National Rosacea Society. Information for Patients. Accessed August 28, 2023.
National Rosacea Society. Rosacea Diary Booklet. Accessed September 8, 2023.
National Rosacea Society. Standard Management Options for Rosacea Patient Handout. Accessed September 6, 2023.
National Rosacea Society. What to Do Now. Accessed September 6, 2023.
National Rosacea Society. When to See a Doctor About Rosacea. Accessed September 6, 2023.
NHS Inform. Rosacea. Last updated February 22, 2023.
New York University Langone Health. Diagnosing Rosacea. Accessed September 6, 2023.
New York University Langone Health. Medical & Surgical Procedures for Rosacea. Accessed September 6, 2023.
New York University Langone Health. Oral Medication for Rosacea. Accessed September 6, 2023.
New York University Langone Health. Rosacea. Accessed August 28, 2023.
New York University Langone Health. Topical Treatment for Rosacea. Accessed September 6, 2023.
Searle T, Ali FR, Carolides S, Al-Niaimi F. Rosacea and diet: What is new in 2021? J Clin Aesthet Dermatol. 2021;14(12):49-54.
Sharma A, Kroumpouzos G, Kassir M, et al. Rosacea management: A comprehensive review. J Cosmet Dermatol. 2022;21(5):1895-1904.
Shen S, Yan G, Cao Y, et al. Dietary supplementation of n-3 PUFAs ameliorates LL37-induced rosacea-like skin inflammation via inhibition of TLR2/MyD88/NF-κB pathway. Biomed Pharmacother. 2023;157:114091.
Stanford Medicine. Acne Rosacea. Accessed September 6, 2023.
Stanford Medicine. Differentiating Acne Vulgaris Vs. Acne Rosacea. Accessed September 25, 2023.
Stanford Medicine. Pulsed Dye Laser Treatments. Accessed September 7, 2023.
Sobkowska D, Szałapska A, Pawlaczyk M, et al. The role of cosmetology in an effective treatment of rosacea: A narrative review. Clin Cosmet Investig Dermatol. 2023;16:1419-1430.
University of Texas Southwestern Medical Center. Rosacea. Accessed September 5, 2023.
van Zuuren EJ, Arents BWM, van der Linden MMD, Vermeulen S, Fedorowicz Z, Tan J. Rosacea: New concepts in classification and treatment. Am J Clin Dermatol. 2021;22(4):457-465.
Wilkin J, Dahl M, Detmar M, et al. Standard classification of rosacea: Report of the National Rosacea Society Expert Committee on the classification and staging of rosacea. J Am Acad Dermatol. 2002;46(4):584-587.
Yale Medicine. Rosacea. Accessed August 29, 2023.
Yang X, Cai M. New insights into the mutual promotion of rosacea, anxiety, and depression from neuroendocrine immune aspects. Clin Cosmet Investig Dermatol. 2023;16:1363-1371.
Yumeen S, Hohman MH, Khan T. Laser Erbium-Yag Resurfacing. StatPearls [Internet]. Last updated July 10, 2023.
Zhang H, Tang K, Wang Y, Fang R, Sun Q. Rosacea treatment: Review and update. Dermatol Ther (Heidelb). 2021;11(1):13-24.
Zhu W, Hamblin MR, Wen X. Role of the skin microbiota and intestinal microbiome in rosacea. Front Microbiol. 2023;14:1108661.



