Updated on February 2, 2023
Many people have vivid memories of childhood chickenpox infections—the itchy spots, the oatmeal baths, and the social isolation until you were no longer contagious. Maybe you had a mild case and weren’t bothered too much by symptoms, except for those itchy areas you were told not to scratch.
But you may not know that you are still at risk of developing a serious infection related to chickenpox, called shingles. Understanding shingles begins with shedding light on the source of chickenpox.
The chickenpox virus
Chickenpox is caused by the varicella-zoster virus, which spreads easily through direct contact and also via coughing or sneezing. Symptoms typically develop 10 to 21 days after infection. Though the reddish, raised itchy spots (“pox”) are one sign of illness, the chickenpox virus can also cause fever, loss of appetite, headache, and fatigue.
The stages of the chickenpox rash include the development of pink or red bumps, followed by small fluid-filled blisters and finally, crusts and scabs on the skin. These symptoms can last for up to 10 days and are usually mild. In some cases, however, skin lesions may be more severe and can affect the entire body, including the eyes and throat.
The best way to reduce your risk of chickenpox infection is by getting vaccinated. According to the Centers for Disease Control and Prevention (CDC), more than 90 percent of those who get the full vaccination are likely to be completely protected from infection.
Chickenpox affects adults, too
Although chickenpox is often considered to be a childhood disease, adults can be infected. You are at higher risk of contracting the virus if you were not infected with it as a child, have not been vaccinated for chickenpox, work in an environment with children (such as a school or childcare facility), or live with children.
Those at higher risk of complications from chickenpox include pregnant people who have not previously been infected, people with an impaired immune system (those with cancer, HIV, or other illnesses), and people who take steroid medications for asthma or other conditions.
Certain people cannot receive the chickenpox vaccine, including those who are pregnant, are severely immunocompromised, have a family history of immunodeficiency, or had a severe allergic reaction after a previous dose. In these cases, or if you are unsure if you should receive the vaccine, it’s best to speak with a healthcare provider about the best course of action.
The relationship between chickenpox and shingles
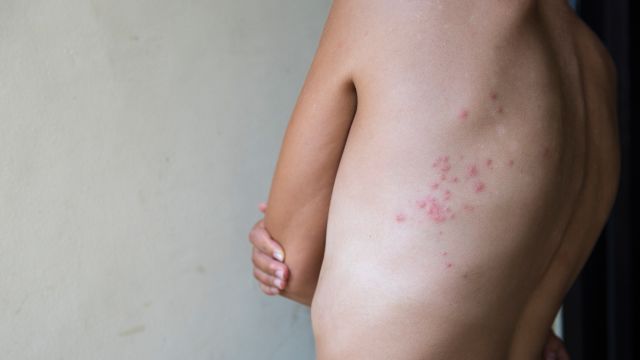
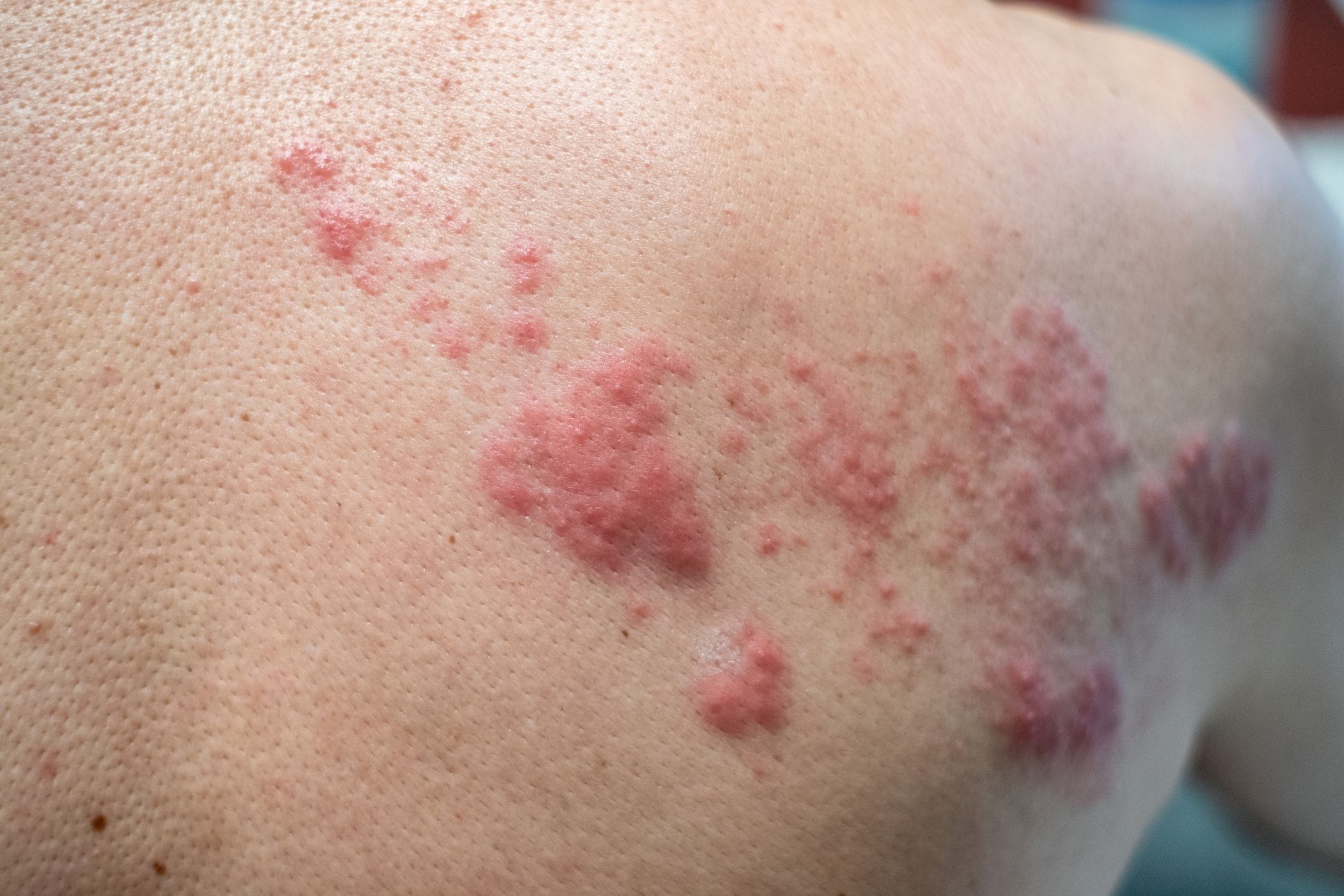
After you’ve recovered from chickenpox, some of the varicella-zoster virus may stay behind in your nerves. If the virus “reawakens” later in life, it can cause shingles, a condition characterized by painful skin blisters that usually develop on one side of the body or face. Other symptoms of shingles include fever, headache, chills, and an upset stomach.
It should be noted: If you receive the chickenpox vaccine and never develop the illness, you can still come down with shingles later on. However, shingles is far less common for vaccinated people than those who get chickenpox.
While you may not be as familiar with shingles as you are with chickenpox, nearly one out of every three people in the United States will develop shingles in their lifetime, according to the CDC. While shingles itself isn't contagious, you can develop chickenpox if you come into contact with fluid from a shingles rash. It is therefore important to cover the blisters and avoid touching them, to wash your hands often, and to avoid people at highest risk of infection, including those with impaired immune systems and pregnant people who have never been infected with chickenpox.
Shingles can also lead to complications, the most common of which is prolonged pain that remains after the blisters have healed, called postherpetic neuralgia (PHN). This can last from a few weeks to months, but the pain could still affect you years later. Other potential complications include vision loss or rarely, pneumonia, hearing issues, palsies (including Bell’s palsy), or brain inflammation.
How to manage shingles
Just as with chickenpox, the best way to prevent shingles is to get vaccinated, which the CDC recommends for healthy adults aged 50 years and older. This applies even if you’ve already had shingles, whether or not you’ve had chickenpox, or if you’ve received a previous version of the shingles vaccine. If you have any questions about shingles vaccination or your vaccination history, talk to your healthcare provider.
If you do develop shingles, there are treatments available that can help manage it. Antiviral medications can shorten the length of the infection and reduce the severity of symptoms; they’re most effective when taken as soon as the rash appears. Pain medications, wet compresses, calamine lotion, and oatmeal baths can help relieve pain and itching.
If you’ve had chickenpox in the past and think you might have developed shingles, be sure to call your healthcare provider about treatment right away.