Each year, more Americans die as a result of lung cancer than any other cancer. The American Lung Association estimates the disease is responsible for roughly a quarter of all cancer deaths.
Most patients aren’t aware they have lung cancer until symptoms appear, at which point the cancer is considered to be advanced. When the illness has progressed to these later stages, conventional treatments like chemotherapy, radiation therapy, and surgery are often less effective than they are at earlier stages. Fortunately, a newer and evolving treatment called immunotherapy is helping some patients feel better and live longer.
Immunotherapy uses medicine to improve your immune system’s ability to identify and destroy cancer cells. Immunotherapies can be used alone or combined with other treatments. Here’s what you should know about these promising drugs.
What is immunotherapy?
There are two main kinds of lung cancer—non-small cell lung cancer (NSCLC), which makes up 80 to 85 percent of cases, and small cell lung cancer (SCLC), which comprises 10 to 15 percent. Immunotherapy drugs called immune checkpoint inhibitors are used to treat certain types of NSCLC.
Here’s how checkpoint inhibitors work: On their surface, some immune system cells have “checkpoints,” or certain proteins that prevent them from attacking normal cells. Cancer cells can also have these proteins, which enable them to avoid detection and attack by the immune system. Checkpoint inhibitors block the proteins, taking the leash off immune cells and allowing them to better tackle the cancer.
The decision to treat with immunotherapy and the type of immunotherapy drug to use (as well any additional treatments used in combination with immunotherapy) will depend on the individual circumstances of your diagnosis. Testing your biomarkers, or your biological indicators of disease, can help predict if you will benefit. Other important factors include the stage of your lung cancer, your general health, cancer treatments you have used in the past, and your current treatment goals.
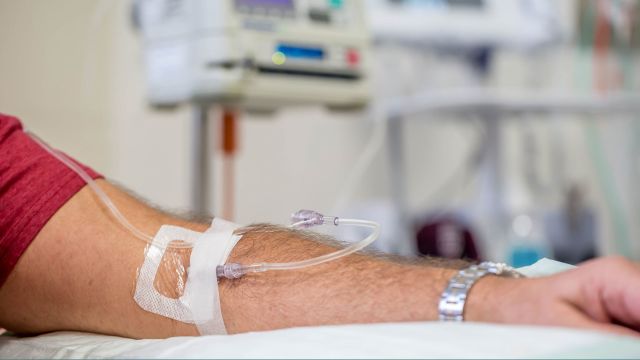
Immunotherapy medications are given intravenously—via an IV—about every two or three weeks, often for several months. It’s considered an outpatient treatment, meaning an overnight hospital stay is usually not necessary. Patients typically receive the drugs in their healthcare provider’s office, a local clinic, or a hospital.
It’s important to note that there may be side effects to immunotherapy. These include fatigue, coughing, nausea, skin issues, appetite loss, constipation, and diarrhea, as well as muscle, bone, or joint pain. Patients may also develop inflammation in different parts of the body, such as the lungs, colon, liver, and thyroid.
Speaking with your healthcare provider
Before you begin, and after you’ve started immunotherapy, it’s important to keep an open line of communication with your cancer care team, and to understand each specialist’s role, so you know who to reach out to with problems. Be sure to ask questions and report issues to your providers, including any side effects.
Also of note: Many promising immunotherapy medicines are currently undergoing clinical trials. You may be eligible to participate and benefit from these treatments; ask your healthcare provider for more information.