7 things that can cause spotting between periods
Are you noticing spotting off schedule? Here are some possible reasons—and when to see a healthcare provider.
Updated on January 4, 2024

There may be months when you think your period is over, only to notice spots of blood in your underwear a few days later. This is more common than many people think and there are several reasons why it may happen.
First, the basics: Menstrual cycles usually last between 24 and 38 days, with a typical period running anywhere from a few days to about a week. If you bleed between periods, it’s considered irregular. Depending on how heavy the blood flow is, it can be referred to as spotting or intermenstrual bleeding.
“Spotting can happen at any point in the cycle, but it’s not a steady flow,” says Ma.Lourdes Mina, MD, an OBGYN in Macon, Georgia. Spotting can appear as pink blood on toilet paper after you urinate or have sex or spots of blood in your underwear either before or after your period. It’s considered spotting if the blood is so light it wouldn’t require the use of a panty liner.
Although most reasons for spotting (such as switching birth control methods) are considered benign, others may be more serious. Spotting along with certain other symptoms might point to an underlying condition. If you notice spotting that lasts more than a day or two, especially if you have other symptoms, you should schedule a visit with your healthcare provider (HCP). “Any bleeding that is concerning needs to be checked,” says Dr. Mina. Your gynecological practitioner might point to one of the following reasons for your spotting.
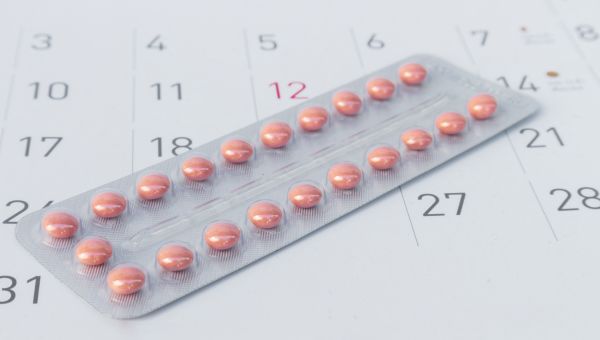
Oral contraceptives
Birth control pills contain either a combination of the hormones estrogen and progestin or progestin only. Estrogen combined with progestin prevents your ovaries from releasing an egg. Progestin alone can prevent ovulation or prevent the egg from meeting up with the sperm.
“If you miss a pill, change birth controls in the middle of a pack, or skip your placebo pills, you're adjusting your body’s hormone levels,” says Mina. That change in hormones can cause spotting. (Placebo pills are the ones you take during the week when you get your period.)
If you notice blood and your menstrual cycle lasts longer than 38 days or is shorter than 24 days, check in with your HCP. Oral contraceptives differ in their regimens. Certain formulations are also continuous, so be sure to discuss the cycle lengths you should expect and when you should report an abnormal length. Remember to tell your HCP about other medications you take—including over-the-counter drugs, vitamins, and herbal supplements—since certain drugs can interact with the pill and cause spotting.

Emergency contraception
Emergency contraception is a type of birth control that temporarily stops an ovary from releasing an egg or prevents that egg from being fertilized. It’s technically effective within five days of unprotected sex, though many pills work best when used as soon as possible within the first three days. If you choose to use it, be sure to check with an HCP about timing and ask which method might be best for you. Certain methods may be less effective for people considered to be obese.
Mina says that it's not uncommon to have spotting or bleeding like a period when using an emergency contraceptive. “If your spotting lasts longer than a few days or becomes heavier, you should speak with your gynecologist,” she says.
When you do get your period after using emergency contraception, it might come earlier or later than what you consider your typical cycle.

Sexually Transmitted Infections
Any sexually transmitted infection (STI) affecting the cervix can cause bleeding, especially after sex. Two common examples are chlamydia and gonorrhea. If you have painful urination or increased discharge along with irregular bleeding, it’s important to see your HCP. Chlamydia often comes without symptoms, so even if you are only experiencing irregular bleeding, it’s a good idea to get checked out just to be safe.
Left untreated, these types of STIs can lead to complications such as pelvic inflammatory disease (PID), which may also cause bleeding between periods or even infertility. Both chlamydia and gonorrhea can be treated with antibiotics, so it’s important to see your HCP for diagnosis and treatment as soon as possible to clear up the infections.
If you’re sexually active, speak with your HCP about regular STI screening and a Pap test to monitor your health.

Menopause
Perimenopause is the transitional phase leading up to menopause. When you experience perimenopause, your menstrual cycle often becomes less predictable than it once was. In some cases, it could become shorter, going from 28 days to, say, 26 days. Some people might skip their period altogether or it may become heavier or lighter. Other symptoms can include hot flashes, night sweats, and mood swings.
Menopause is defined as going 12 consecutive months without a menstrual period. Once you reach menopause, spotting or vaginal bleeding becomes unlikely; see an HCP if you experience it. Some common causes for bleeding after menopause include endometrial atrophy or endometrial hyperplasia. (Endometrial atrophy occurs when estrogen levels drop, causing the endometrium, or lining of the uterus, to thin. Endometrial hyperplasia occurs when the endometrium thickens.) Treatment for postmenopausal bleeding will depend on the cause. Prompt diagnosis and treatment of endometrial hyperplasia, in particular, is essential. Left untreated, it may lead to cancer.

Uterine Fibroids
Uterine fibroids are noncancerous tumors that grow in the wall or inside the cavity of the uterus. They may grow as a single tumor or in groups. They're fairly common, especially among people in their 40s and early 50s, and they are nearly always benign.
But if the growth occurs within the innermost layer of the uterus, it can cause spotting between periods. Other symptoms might include heavy and painful periods, frequent urination, and painful sex. Some people who have uterine fibroids don’t experience any symptoms at all.
Treatment will vary depending on the symptoms you’re experiencing as well as the size of the fibroids. Over-the-counter medication or birth control may be used to treat less severe cases, while other drugs or surgical removal of the tumors may be necessary to treat more severe cases.
Fibroids are also genetically linked to endometriosis, another uterine condition that may also cause spotting. The most noticeable symptom of endometriosis, however, is pelvic pain. If you experience pain and spotting, talk to your HCP.

Miscarriage or pregnancy complications
A miscarriage, or a loss of pregnancy, can happen at any time, but usually occurs in the first trimester, sometimes before a person even realizes they’re pregnant. “When people who typically have regular, predictable periods miss a period or have less bleeding than usual, it can be a sign either of pregnancy or a miscarriage,” says Mina. Other symptoms of a miscarriage might include lightheadedness, pain in the abdomen, brown discharge, or other irregular bleeding.
It's important to note that if someone knows they’re pregnant and experiences irregular bleeding, it doesn’t necessarily mean it’s a miscarriage. Spotting during pregnancy is fairly common and can happen at any time. But if you’re pregnant and you experience spotting, it's still important to call your HCP to discuss your symptoms.

Cancer
Most cancers of the reproductive organs can have intermittent, abnormal bleeding as a symptom. These include vaginal, cervical, uterine, and ovarian cancer.
If you experience bleeding lasting two weeks or longer, see your HCP. That goes double if you’re having bleeding along with other symptoms such as pelvic pain, bloating, frequent urination, or itching/burning in the vulva. The symptoms for each gynecological cancer vary from person to person and depend on the type of cancer.
Pap tests can help detect cervical cancers. Other cancers, like ovarian cancer, are harder to detect because there is no formal screening. Going to your regular checkups and screenings could help identify some types of cancer earlier, when they may be easier to treat. If the cancer is at a more advanced stage, surgery and chemotherapy might be required for treatment.

Office on Women’s Health. U.S. Department of Health and Human Services. Your menstrual cycle. Page last updated March 16, 2018.
Office on Women’s Health. U.S. Department of Health and Human Services. Birth control methods. Page last updated February 14, 2019.
Centers for Disease Control and Prevention. Gonorrhea – CDC Fact Sheet. Page last reviewed January 29, 2014.
Centers for Disease Control and Prevention. Chlamydia – CDC Fact Sheet. Page last reviewed January 23, 2014.
Centers for Disease Control and Prevention. Pelvic Inflammatory Disease (PID) – CDC Fact Sheet. Page last reviewed November 19, 2020.
The North American Menopause Society. Menopause 101: A primer for the perimenopausal.
The American College of Obstetricians and Gynecologists. Endometrial Hyperplasia. Last updated February 2021.
Office on Women’s Health. U.S. Department of Health and Human Services. Uterine Fibroids. Page last updated April 1, 2019.
Wise LA, Laughlin-Tommaso SK. Epidemiology of Uterine Fibroids: From Menarche to Menopause. Clinical Obstetrics and Gynecology. 2016 Mar;59(1):2-24.
The American College of Obstetricians and Gynecologists. Early Pregnancy Loss. Last reviewed February 2020.
Centers for Disease Control and Prevention. Gynecologic Cancers. What Are the Symptoms? Page last reviewed August 16, 2021.
Mayo Clinic. Birth Control. Last updated December 3, 2022.
More On


video

article

slideshow


video


video
