Updated on January 19, 2026.
When you call your local radiology center to book a breast cancer screening, you may be offered a newer, high-tech option: a three-dimensional (3D) mammogram.
This type of mammography (also called digital breast tomosynthesis or DBT) is now available in the vast majority of screening locations across the country. More than 90 percent of certified imaging centers in the United States have DBT technology, according to the U.S. Food and Drug Administration (FDA).
Both 3D and two-dimensional (2D) mammography are considered effective by the U.S. Preventive Services Task Force (USPSTF). 3D mammography is also approved by the FDA, supported by influential medical organizations, and largely covered by health insurance plans.
With that in mind, here’s what to know about 3D mammograms.
Basics of 3D mammograms
About 1 in 8 women in the U.S. will develop breast cancer at some point. While it’s much more common in women, men can also develop breast cancer. Each year, about 2,400 men in the U.S. are diagnosed with the disease.
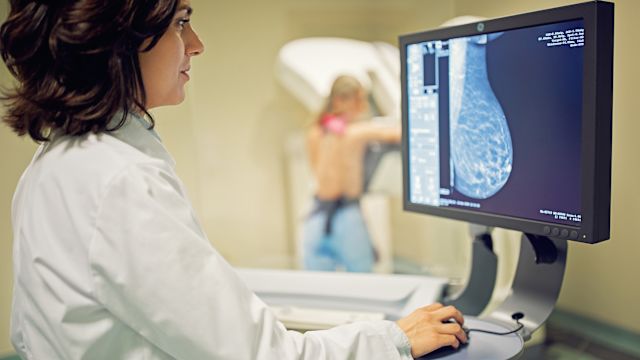
The earlier breast cancer is discovered, the easier it is to treat, and the better the odds of survival. Mammograms are the best way to screen for breast cancer, as they can reveal growths in people who don’t yet have symptoms. During a typical 2D mammogram, X-ray images of your breasts are taken from a pair of angles—the top and the side.
Now, there’s mounting evidence that using 2D and 3D imaging together is more effective for finding cancer. That’s because when you have a 3D mammogram, several pictures are taken from multiple angles. A computer then combines them into one three-dimensional composite image. This creates a more detailed representation of your breast and can help radiologists spot irregularities more easily.
“Think about a loaf of bread,” says Hildegard Toth, MD, a radiologist at NYU Langone Health in New York City. “Looking at the whole loaf at once, you don’t know what’s in the middle of it. If you slice it up, you can see each slice separately.”
While some imaging centers take 2D images independently of 3D images, machines at many centers capture both types of images at the same time. The computer simply uses individual slices of the 3D mammogram to construct 2D images, Dr. Toth says.
Potential benefits of 3D mammograms
Though more studies are needed, there are multiple possible upsides to 3D mammography.
“Fewer women have to be called back for additional views,” Toth says. Estimates vary widely, but one large study published in 2024 in the journal Radiology found that people who received 3D mammograms were called back 7.2 percent of the time, while those with 2D mammograms were called back 10.6 percent of the time.
This is partly because 3D mammograms provide better views in the first place, so irregularities that are found might not need additional imaging. It’s also because 3D mammography may cut down on false positives, or suspicious findings that may initially look like cancer, but end up being relatively harmless. False positives can lead to extra stress, cost, and invasive additional testing.
Another potential advantage of 3D mammography is the ability to detect more cancers than using 2D mammography by itself. It may be especially helpful for people with dense breasts.
Having dense breasts means you have less fatty tissue and more glandular and fibrous tissue in your breasts. Glandular tissue is meant to produce and excrete breast milk, while fibrous tissue supports these milk-producing glands. About 50 percent of women aged 40 and older have dense breasts, which increases their risk for developing breast cancer.
Both cancer and dense breast tissue appear white on the X-rays used in 2D mammograms, so it can be difficult to discern between the two. But 3D mammograms can see beyond these dense areas to detect cancer more accurately.
Getting a mammogram is the only way to confirm whether you have dense breasts. As of March 2023, the FDA requires mammography facilities to notify patients about the density of their breasts.
Potential drawbacks of 3D mammograms
There could be certain downsides to 3D mammography. First, when a 3D mammogram is done separately from a 2D mammogram, you may be exposed to a little more radiation than you would with just one scan. “However,” Toth says, “that dose is still way below the government limit.” In newer machines that perform both functions simultaneously, that exposure is diminished.
There’s also a potential for overdiagnosis, meaning a 3D mammogram could detect breast changes that might never evolve into clinically significant, potentially life-threatening cancer. These findings can result in unnecessary treatment, including biopsies, surgery, and radiation.
And although it’s not necessarily a drawback, it’s worth noting that 3D mammograms are still relatively new. As such, there haven’t been long-term studies conclusively proving that they lower mortality rates or improve quality of life compared to 2D mammograms.
The Tomosynthesis Mammographic Imaging Screening Trial (TMIST), a clinical trial supported by the National Cancer Institute, is among those seeking to shed more light. Beginning in 2017, researchers set out to enroll and monitor 165,000 healthy women between the ages 45 to 74 who planned on receiving regular screening mammograms. When the trial ends in 2030, they’ll compare 2D to 3D mammograms to see if the latter really are better at finding life-threatening cancer.
Moving forward
Given the potential risks and benefits of 3D mammograms, the decision to have one is ultimately up to you and your doctor.
Toth, who supports 3D mammograms “100 percent” says if you decide on a 3D screening, you should confirm that your health insurance will pay for it and whether you’ll need preauthorization. Some private plans may not cover them yet and Medicaid coverage may depend on the state in which you live. Medicare does cover annual 3D mammograms, often fully.
Once you’ve checked your coverage, the process itself is much the same as getting a 2D mammogram. Be sure to pick an FDA-certified imaging facility and make an appointment for when your breasts are less likely to be tender. If you’re breastfeeding, there’s no need to postpone, though you should ideally nurse or pump before the exam. Reach out to your healthcare provider with questions or for more information.
Your mammogram should take less than 20 minutes. It’s a relatively short time for a screening that may ultimately save your life. Time—and more research—will fill us in on the details.