13 possible causes of pelvic pain that aren’t your period
Identifying the source of your discomfort can help you determine the best way to find relief.
Updated on July 23, 2024

Whether it’s a sharp pain that comes and goes, or a dull, steady ache, pain in the pelvic area can be exhausting and, for some people, even debilitating. Pain in this area, generally described as the lower abdomen between your hip bones, can be caused by a variety of different conditions and sometimes more than one condition at the same time.
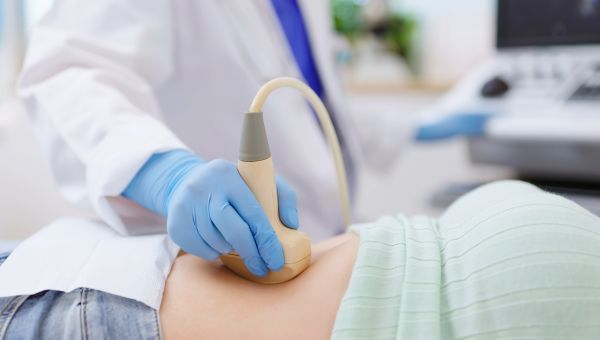
Pelvic pain may originate from any of the organs in the lower abdomen, including the uterus, ovaries, fallopian tubes, bowel, and bladder, says Alex Letham, DO, an OBGYN with LewisGale Hospital Montgomery in Blacksburg, Virginia. It can be hard to pinpoint the exact source, due to the complexity of nerves in the pelvis. That’s also why pelvic pain can be felt in the back or thighs, he adds.
Depending on the cause, the pain can present itself in different ways and on different sides of the pelvis. Determining the underlying cause can help find the best ways to treat it and get relief.

Endometriosis
Pelvic pain and pressure are the most common symptoms of endometriosis, a condition in which the endometrium (the lining of the uterus) grows outside of the uterus in places like the ovaries, fallopian tubes (which connect the ovaries to the uterus), intestines, or bladder. Endometriosis is common: About 1 in every 10 people who are menstruating have it.
Because endometrial tissue is the same type of tissue that’s in your uterus, the growths can mature and bleed as estrogen levels fluctuate. This may cause the surrounding area to become inflamed or swollen and could even result in scarring. All of this irritation can trigger pain in the pelvic region, especially before and during your period.
The preferred treatment options for endometriosis are:
- Over-the-counter pain medicines called nonsteroidal inflammatory drugs (NSAIDs). Examples are ibuprofen and naproxen.
- Birth control options such as oral contraceptive pills or hormonal intrauterine devices (IUDs). IUDs are small T-shaped devices placed in the uterus for birth control.
- A combination of NSAIDs and birth control
If these methods are unsuccessful, or if you’re trying to get pregnant, other options such as prescription medications that work on hormones are often suggested. Sometimes, surgery may be needed to treat endometriosis.

Uterine adenomyosis
Adenomyosis is a condition similar to endometriosis, since it involves the tissue that usually lines the uterus. But with adenomyosis, the tissue grows into the muscular wall of the uterus.
“The intense pelvic pain associated with adenomyosis typically follows trends with the menstrual cycle,” says Dr. Letham. That’s because your uterus swells and expands during that time. You’re likely to have heavy bleeding and even a feeling of heaviness or tenderness in your abdomen. Some people don’t have any symptoms at all, though.
Adenomyosis usually goes away on its own after menopause (not having a period for 12 months in a row). In the meantime, you can find relief with NSAIDs, or birth control options such as oral contraceptive pills or IUDs. In some cases, certain prescription medications that work on hormones or a hysterectomy (surgical removal of the uterus) are needed.

Ovarian cysts
A cyst is a sac consisting of fluid and tissue. When one forms in or around the ovaries, it's known as an ovarian cyst. Small ovarian cysts don’t always cause symptoms. When ovarian cysts do cause symptoms they can lead to pain, pressure, and bloating. Ovarian cyst pain can feel dull or sharp, sometimes on one side of your abdomen. “Pain associated with ruptured cysts can be random and sporadic and can cause some brief, intense pain that resolves over the course of a few days,” says Letham. Cysts are almost always non-cancerous.
Treatment for ovarian cysts depends on a few things, including:
- Their size, shape, and location
- Your age
- Whether or not you want to have children
- Whether or not you’re experiencing symptoms
- Your history of ovarian or breast cancer
Many people may not need any treatment since most cysts go away on their own after a couple of menstrual cycles. If cysts don’t disappear by themselves, your healthcare provider (HCP) may want to monitor them and watch for any changes.
If there are concerns that the cysts may be cancer, if the cysts are getting larger or look unusual, or if the cysts are causing major pain or other severe symptoms, a cystectomy (surgery to remove the cyst) or an oophorectomy (surgery to remove the ovary) may be needed, especially if you’re in menopause.
In rare cases, an ovarian cyst can rupture or become twisted (this is called torsion). When this happens, it can be a medical emergency, particularly if you experience sudden, severe abdominal pain with fever, vomiting, dizziness, weakness, or rapid breathing. Oral contraceptives are often recommended to help prevent new cysts from forming.

Uterine fibroids
Uterine fibroids, also known as leiomyomas or myomas, are non-cancerous growths that contain uterine muscle and fibrous connective tissue. “A fibroid slowly enlarges to a very firm ball-like mass,” says Letham. They can develop on the inside or outside of the uterus, inside the uterine wall itself, or be attached to it by a stem-like structure. Fibroids can get bigger over time but may remain small forever.
Some people who have uterine fibroids don’t experience any symptoms, but others will. “Because they are disrupting the muscle around the uterus, fibroids can cause pain and heavy periods, and can get large enough to impact the bladder or rectum,” Lethem adds. Pelvic pain or lower back pain that’s achy and sometimes sharp may accompany fibroids. Pain during sex is also typical.
If you’re not experiencing any symptoms, you may not need treatment. For more mild pain, over-the-counter pain relievers can help. If pain or other symptoms are interfering with your daily life, talk to your HCP. To help reduce pain and heavy bleeding, you may be prescribed birth control pills, an IUD, or a contraceptive injection. Your HCP may also prescribe medications that work on your hormones.
If your symptoms are severe, your HCP may recommend a surgical procedure to remove the fibroids. Myomectomies are usually recommended for those who want to become pregnant. This is a surgery that cuts out the fibroids but does not remove the uterus. New fibroids can still form after this surgery, though. If your fibroids are extremely large or other treatments haven’t worked, a hysterectomy may be recommended.

Pregnancy and miscarriage
Up to 75 percent of people who are pregnant experience some sort of pelvic pain (or lower back pain) over the nine months of pregnancy. It can occur at any time due to the way the bones and ligaments loosen and shift in the body to accommodate the pregnancy, though pain is often most prominent in the third trimester as the fetus gets larger and puts pressure on the pelvic area. Digestive and urinary tract pain may also develop during the earlier stages of pregnancy.
About two to four weeks before delivery, pregnant people may notice some pelvic heaviness that reaches around to their back. This may occur as the fetus drops lower into the pelvis to prepare for delivery.
Certain serious conditions that may develop during pregnancy can cause intense pain. These include:
- Ovarian torsion, or twisted ovary
- Ectopic pregnancy, when the fertilized egg implants outside the uterus, often in a fallopian tube
- Miscarriage, or loss of pregnancy before the 20th week
If you have a sharp pain on one side that makes it hard for you to walk, breathe, or talk, or is accompanied by other symptoms such as vomiting or bleeding, call 911 or head to the emergency room.
Regardless of how far along you are in your pregnancy, it’s best to talk with your HCP if you’re having any type of pain. After evaluation, if you’re told that your pain is typical, you can try stretching, walking, and breathing techniques to get some relief. Always follow your HCP’s advice for treatment during pregnancy.

Ovulation
“Some people will have pain for a few short days during ovulation, which is usually sometime between day 11 and day 15 of their menstrual cycle,” says Letham. “This type of pain is technically called mittelschmerz, which is German for ‘middle’ and ‘pain.’”
This pain occurs because the ovary is releasing an egg. It usually occurs on one side of the body each month, and it may switch sides from month to month.
If you’re having pain, the easiest way to connect it to ovulation is to start taking a closer look at your menstrual cycle. “Keeping a pain diary and tracking your cycle can be very helpful for the doctor when you come in for evaluation,” says Letham. You can use a regular notepad or a calendar app to record the day of your first period, how long your period lasts, and any symptoms you’re experiencing.
Ovulation pain usually goes away on its own. Over-the-counter anti-inflammatory medications like ibuprofen may provide some relief. If it lasts for more than a couple of days, gets worse, or is accompanied by burning urination or irregular bleeding, see your HCP.

Urinary tract infections
In addition to gynecological issues, other health conditions can cause discomfort in the pelvic region. A urinary tract infection (UTI) most often occurs when bacteria get into the urinary tract and start to multiply in the bladder. The typical symptom is a burning sensation while urinating combined with the urge to go more frequently. When a UTI is severe, says Letham, it may also result in lower abdominal soreness and pelvic pressure.
If you suspect you have a UTI, check in with your HCP, who can confirm the diagnosis and prescribe antibiotics to treat the infection.

Irritable bowel syndrome
Irritable bowel syndrome (IBS), is a chronic digestive condition that often triggers pain in the abdominal and pelvic areas. Bloating, constipation, and/or diarrhea are also common symptoms.
Many IBS treatment options involve lifestyle changes, including:
- Avoiding trigger foods
- Gradually adding more fiber to your diet
- Eating smaller meals throughout the day
Fiber supplements, antidepressants, antidiarrheals, and other IBS-specific medications can also help relieve symptoms. Sometimes, stress-relief techniques are also recommended, because stress can worsen IBS symptoms.

Pelvic inflammatory disease
Left untreated, certain sexually transmitted infections such as chlamydia and gonorrhea can lead to pelvic inflammatory disease (PID), an infection of the female reproductive organs. Other infections that are not sexually transmitted may also cause it. Douching can increase the risk for PID, as well. Those who use IUDs may have a small increased risk of PID in the few weeks after placement.
For some, PID may not cause symptoms. Others may notice symptoms such as:
- Pelvic pain
- Fever
- Irregular discharge from the vagina
- Pain or bleeding with sex
- Burning sensation while urinating
- Bleeding between periods
PID is curable with antibiotics. The earlier you begin treatment, the better because untreated PID can lead to complications including damage to the reproductive organs. Once PID is cured, it’s possible to get it again.
Ovarian torsion
A rare but serious condition, ovarian torsion is caused when the fallopian tubes or the ovary get twisted around the surrounding tissues. Also known as adnexal torsion, this condition usually happens on just one side. Warning signs in the form of cramps could occur for a few days or weeks before it causes sudden, severe pain, nausea, and vomiting. Most cases of ovarian torsion occur in adults of reproductive age; up to 30 percent of cases, meanwhile, may occur in people under age 20. Having an ovarian cyst can raise the risk of ovarian torsion.
The only method of treating ovarian torsion is surgery. If the twisting cuts off the blood supply and it isn’t fixed quickly, the ovary can die. However, if it’s attended to promptly, many people have a full recovery. Early recognition and treatment are vital.

Interstitial cystitis
When the walls of the bladder get irritated, it can result in symptoms like bladder pressure, bladder pain, and needing to urinate more frequently but only having a small volume of urine. This condition is known as interstitial cystitis. Sometimes it can also cause pelvic pain, including pain during sex, and between the vagina and anus or between the scrotum and anus.
This chronic condition is more likely to occur in people assigned female at birth, those over age 30, and those with irritable bowel syndrome or a chronic pain disorder like fibromyalgia (which causes chronic pain throughout the body). There is no cure, but there are many medications and therapies that help ease symptoms. These include physical therapy, a wide variety of oral medications, nerve stimulation techniques, and bladder distension (stretching the bladder). Some medications may also be applied directly to the bladder through a small tube called a catheter. For people with severe cases, if other treatments don’t help, surgical options are also available.

Appendicitis
When the appendix, a small organ that's attached to your large intestine, becomes inflamed, it causes appendicitis. Between five and nine percent of people will get appendicitis at some point in their lives. Anyone can get it, though it’s slightly more common in young adults and in people assigned male at birth.
The usual symptom of appendicitis is severe pain that starts suddenly. The pain is generally located around the belly button at first, then moves down and to the right. It may intensify if you move, sneeze, or cough. Loss of appetite, fever, swelling, nausea, constipation, and diarrhea are also possible symptoms. Sometimes children don’t get these same symptoms, so it’s important to consult an HCP about any abdominal symptoms a child might be having.
If it’s not treated, appendicitis can cause the appendix to burst, which can lead to a life-threatening infection. With prompt treatment, most people make a full recovery. Treatment may include the use of antibiotics or a surgical procedure called an appendectomy (removal of the appendix).

Musculoskeletal pain
A number of different health issues can affect the connective tissues, joints, and bones around the pelvis and cause recurring pelvic pain. If the pelvic floor muscles are tense or weak, either from being injured or from lack of use and exercise, it can be painful. These muscles can spasm or can be sore to the touch.
Sometimes nerves, joints, or other tissues might be compressed or stretched from daily movements, childbirth, or surgery. These issues may also be caused by fibromyalgia and hernias (when part of the body, such as part of an organ or tissue, protrudes through weakened tissue in the body).
Careful examination by an HCP will help to identify the exact musculoskeletal cause, after ruling out more serious conditions. The most common treatments for musculoskeletal pelvic pain are physical therapy and biofeedback. Biofeedback works by connecting your awareness of your own body with a piece of technology like an electrocardiogram (ECG, which measures brain waves), breathing sensor bands, or temperature monitors. When your body tenses, your heart races, or you begin breathing quickly, the sensors let you know immediately so you can consciously intervene with relaxation and breathing techniques.

See your healthcare provider if you have questions
The most important thing to remember about pelvic pain is that you should see your HCP for any pain that arrives suddenly or worsens, no longer responds to medications, or keeps you from daily activities, says Letham. Your HCP can examine you to determine what’s going on, refer you to another specialist if needed, and recommend your best options to find relief.

Office on Women’s Health. U.S. Department of Health and Human Services. Endometriosis. Page last updated: April 1, 2019.
Mayo Clinic. Adenomyosis. June 18, 2020.
Li J-J, Chung JPW, Wang S, Li T-C, Duan H. The investigation and management of adenomyosis in women who wish to improve or preserve fertility. Biomed Res Int. 2018;2018:6832685.
Office on Women’s Health. U.S. Department of Health and Human Services. Ovarian cysts. Page last updated: April 1, 2019.
Office on Women’s Health. U.S. Department of Health and Human Services. Uterine fibroids. Page last updated April 1, 2019.
Emily E. Bunce, MD and Robert P. Heine, MD. Pelvic Pain During Early Pregnancy. Merck Manual Consumer Version. Content last modified Jun 2021.
Kanakaris NK, Roberts CS, Giannoudis PV. Pregnancy-related pelvic girdle pain: an update. BMC Med. 2011;9:15.
U.S. National Library of Medicine. Mittelschmerz. Review date March 8, 2019.
National Institute of Diabetes and Digestive and Kidney Diseases. Bladder Infection (Urinary Tract Infection—UTI) in Adults. Accessed October 29, 2021.
Office on Women’s Health. U.S. Department of Health and Human Services. Irritable bowel syndrome. Page last updated April 1, 2019.
Centers for Disease Control and Prevention. Pelvic Inflammatory Disease (PID) – CDC Fact Sheet.
Yale Medicine. Ovarian Torsion. Page accessed March 26, 2024.
Mayo Clinic. Interstitial cystitis. Page last updated September 29, 2021.
National Institute of Diabetes and Digestive and Kidney Diseases. Appendicitis. Page last reviewed July 2021.
Mayo Clinic. Chronic Pelvic Pain. Page last updated February 28, 2024.
UCSF Health. Pelvic Pain. Page accessed March 26, 2024.
Mayo Clinic. Biofeedback. Page last updated March 18, 2023.
More On


video

article

slideshow


video


video
