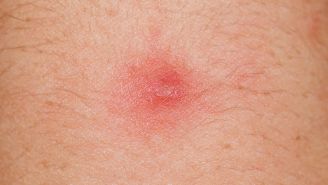
Urticaria is the clinical term for hives—red, raised, itchy welts that form on the surface of the skin. Hives are classified as either acute or chronic, depending on how long symptoms last. Hives are categorized as acute when symptoms resolve within six weeks, and chronic when symptoms persist for six weeks or longer. Only a very small percentage of the total population experience chronic urticaria, but for some, symptoms last for months or even years, and can be difficult to treat.
The initial steps for treating hives are avoiding triggers and taking medications called antihistamines. However, these steps are not always effective for every person. The majority of cases of chronic hives are categorized as chronic spontaneous urticaria (previously known as chronic idiopathic urticaria). With this type, the cause of the hives is unknown, and is not associated with any identifiable allergen or trigger.
Antihistamines work by blocking inflammatory chemicals called histamines. If symptoms do not respond to treatment with antihistamines, a healthcare provider may recommend a stronger-dose antihistamine, a different type of antihistamine, or another type of treatment. Other treatment options for chronic hives include corticosteroids, immunosuppressive drugs, a biologic therapy, and therapies for other conditions that may have a therapeutic benefit for chronic hives.
Glucocorticoids
Glucocorticoids are a type of corticosteroid, which is a type of anti-inflammatory drug. They are usually taken orally and may be prescribed as a short-term treatment when hives do not respond to treatment with strong doses of antihistamines. Because of the risk of side effects, steroids should not be prescribed as long-term treatments.
Biologic therapy
Biologic therapies are drugs that suppress or regulate immune activity. Biologic therapies are used to treat a variety of autoimmune and immune-mediated diseases. There is also a biologic therapy that is indicated for the treatment of chronic spontaneous urticaria.
Immunosuppressive drugs
There is research that supports the idea that some cases of chronic hives are associated with abnormal immune system activity that causes an unnecessary inflammatory response. Hives are also known to occur in people with certain autoimmune diseases, such as lupus. Therapies used to treat autoimmune disease are sometimes used to treat chronic hives, including immunosuppressive drugs.
Immunosuppressive drugs work by suppressing the immune system. In people who have autoimmune disorders, immunosuppressive drugs can help reduce the abnormal immune system activity that is causing symptoms.
Any therapies that impact the way the immune system works come with a risk of serious side effects, which patients and their healthcare providers will need to consider before starting an immunosuppressive or a biologic therapy.
Off-label therapies
While medications are approved for the treatment of specific health conditions, they sometimes have therapeutic benefits for other conditions they are not approved to treat—and healthcare providers sometimes prescribe medications for those other conditions. This is called “off-label prescribing.”
There are a number of treatments for other conditions that may have therapeutic benefits for chronic urticaria, which may be prescribed off-label. These include medications for asthma, malaria, gout, and depression. Any medication should always be taken under the guidance of a healthcare provider.
Choosing a healthcare provider
In many cases, hives will be treated by an allergist, a healthcare provider who specializes in the treatment of allergies. People who have chronic hives may also want to work with a dermatologist, a healthcare provider who specializes in disorders that affect the skin. Certain treatments are only available through a specialist.