6 things that can worsen atopic dermatitis
Dry temperatures, chemicals and other atopic dermatitis triggers to avoid.
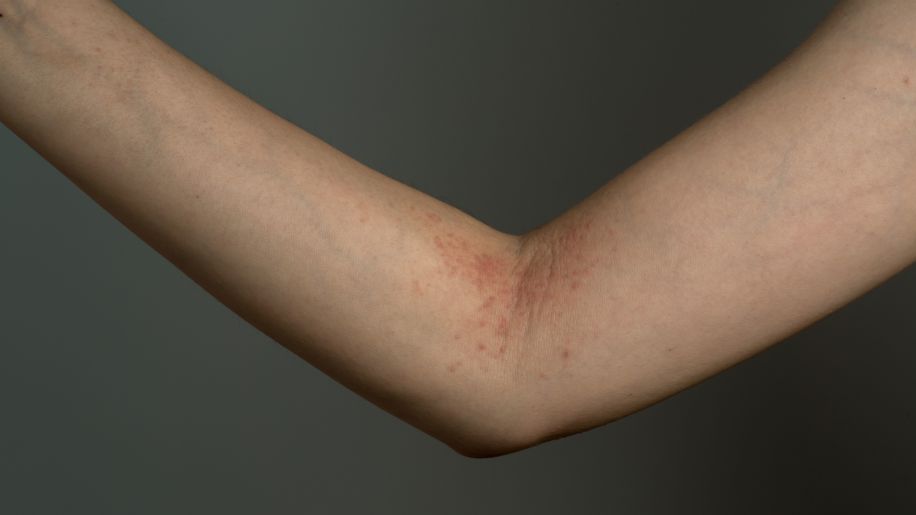
Atopic dermatitis is the most common form, and one of the more severe forms, of eczema. People who have atopic dermatitis experience flares of dry, itchy, irritated skin that can be red, scaly, flaky and covered in red bumps. Atopic dermatitis affects an estimated 27 million people in the United States, and affects people of all ages; most people with atopic dermatitis first experience symptoms during childhood.
Healthcare experts do not know the exact cause of atopic dermatitis and there is no cure for the condition. Treatment involves working with a healthcare provider, keeping the skin hydrated, treating irritated skin when it occurs and avoiding triggers, or factors that aggravate symptoms.
The following slides look at a few things that may trigger atopic dermatitis flares or worsen symptoms.

Hot temperatures
Managing atopic dermatitis is a constant battle against dry skin, and heat will make dry skin worse and exacerbate symptoms, especially itching. This is especially true of hot environments where there is little humidity in the air, such as indoor areas that are heated with space heaters. Heat also causes the skin to sweat, which can trigger or aggravate symptoms in patients whose skin is sensitive to sweat.
Hot environments are nearly impossible to avoid all of the time, but there are steps you can take to minimize their impact on your skin. Take lukewarm showers instead of hot showers. Keep the temperatures in your home moderate and consider using a humidifier. Exercise indoors on a hot summer day. And if your skin is sensitive to sweat, speak with your healthcare provider about ways you can manage sweat to minimize its impact on your skin.
Cold temperatures can also dry out the skin, and are covered on the next slide.

Cold temperatures
Cold temperatures also dry out the skin and exacerbate atopic dermatitis symptoms. Again, this is especially true of environments where the air is dry—such as a cold winter day with low humidity. Winter is often reported to be the worst season for atopic dermatitis (but not for all patients), and this could be for a number of reasons: cold, outdoor weather; hot, dry indoor environments; dressing in clothes that offer less ventilation; and shorter days with fewer hours of sunlight. Sudden shifts in temperature—whether it’s a change in weather, or from moving between outside and indoors—can also aggravate symptoms.
If you’re in an area that experiences cold temperatures, you should do everything you can to minimize the impact those temperatures have on your skin. Be diligent with your moisturizing and skincare routine, avoid other known triggers and use a humidifier in your home. It’s also important to make sure your warm clothing is made from materials that do not aggravate your symptoms. Clothing is discussed on the next slide.

Wool and synthetic fibers
Avoid clothing made from rough, scratchy fabrics and fibers, which can irritate the skin, aggravating itching and other symptoms. This includes wool and some synthetic fibers, such as such as acrylic, polyester, spandex and nylon. Soft cotton clothing is recommended, but cotton may have its own potential problems. Cotton clothes made from short fibers can also be scratchy, and dyes used in cotton clothing can act as irritants. Cotton can also harbor bacteria and fungus, two things people with atopic dermatitis should make an effort to avoid since the damaged skin that results from atopic dermatitis is more prone to infection.
Choosing clothes to avoid aggravating atopic dermatitis is the same as choosing clothes for fashion—it’s going to be a little different than everyone. Pay attention to how what you’re wearing affects your skin, and build your wardrobe around what works.

Chemicals
In addition to choosing clothing that doesn’t aggravate your skin, it’s also important to pay attention to the detergent you use on your clothing. Detergents—as well as many other products—contain chemicals that may aggravate atopic dermatitis symptoms. Choosing a detergent for sensitive skin, rinsing clothes after washing and washing new clothing before wearing can help limit your contact with potential irritants.
Additionally, avoid contact with household cleaners with ingredients like ammonia, harsh soaps and beauty products that contain alcohol, fragrances and preservatives. Opt for natural or organic cleaning products that use ingredients like baking soda and vinegar, castile soap and beauty products for sensitive skin. When using a new beauty product, such as makeup or hair dye, it’s also a good idea to do a patch test—apply a small amount of the product to the skin of your forearm and watch for a reaction.

Stress
Emotional and mental stress can trigger and exacerbate atopic dermatitis symptoms. While the connection between stress and atopic dermatitis is not yet fully understood, it is known that stress impairs skin barrier function—the ability of your skin to keep out irritants and retain water.
In addition to stress being a trigger for atopic dermatitis, atopic dermatitis is a stressful condition for a number of reasons. Many people with the condition feel embarrassed about the appearance of their skin. Itching tends to worsen at night, which can disrupt sleep. It can be extremely frustrating when symptoms flare up despite following your treatment plan and skincare routine. Anyone experiencing stress or anxiety should discuss these feelings with his or her healthcare provider.

Scratching
While more a symptom than a trigger, the itch/scratch cycle is one of the most frustrating aspects of atopic dermatitis, and one that can severely impact a person’s quality of life. Atopic dermatitis is associated with anxiety, depression, difficulty concentrating and an inability to get adequate amounts of sleep. Avoiding factors that aggravate symptoms, following your treatment plan and moisturizing regularly are all important to reducing itch and the urge to scratch.
Do whatever you can to avoid scratching itchy skin. Scratching or rubbing to relieve itch can damage the skin and make symptoms worse. Scratching can also introduce bacteria into the skin, which can cause infection. Keeping nails trimmed can help reduce the damage caused by scratching, but it is important to take steps to reduce itching and the urge to scratch. Some patients wear thin cotton gloves to bed to protect their skin from scratching during sleep. Applying moisturizer to itchy skin can also provide relief.
Featured Content
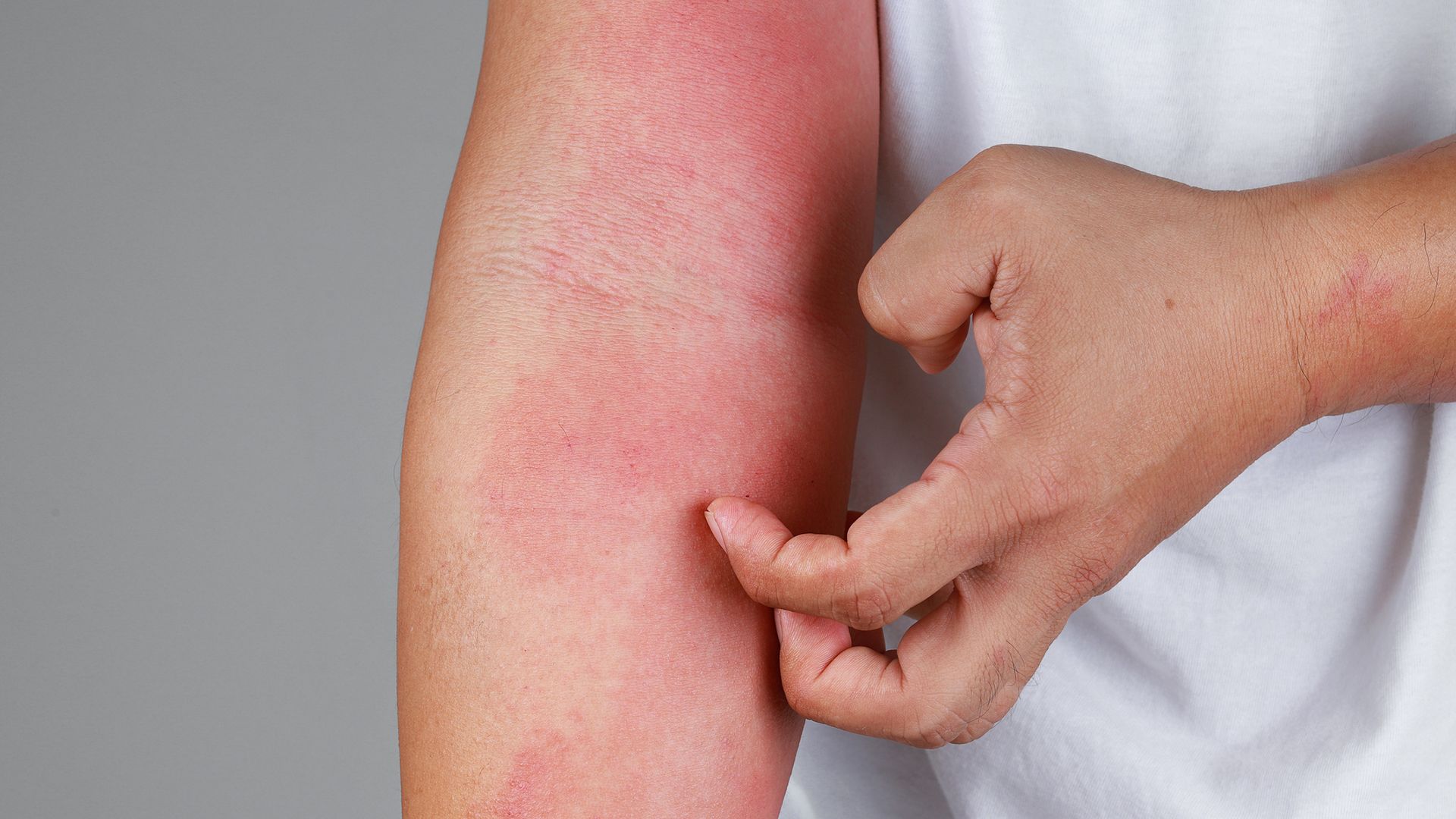
article

article

article
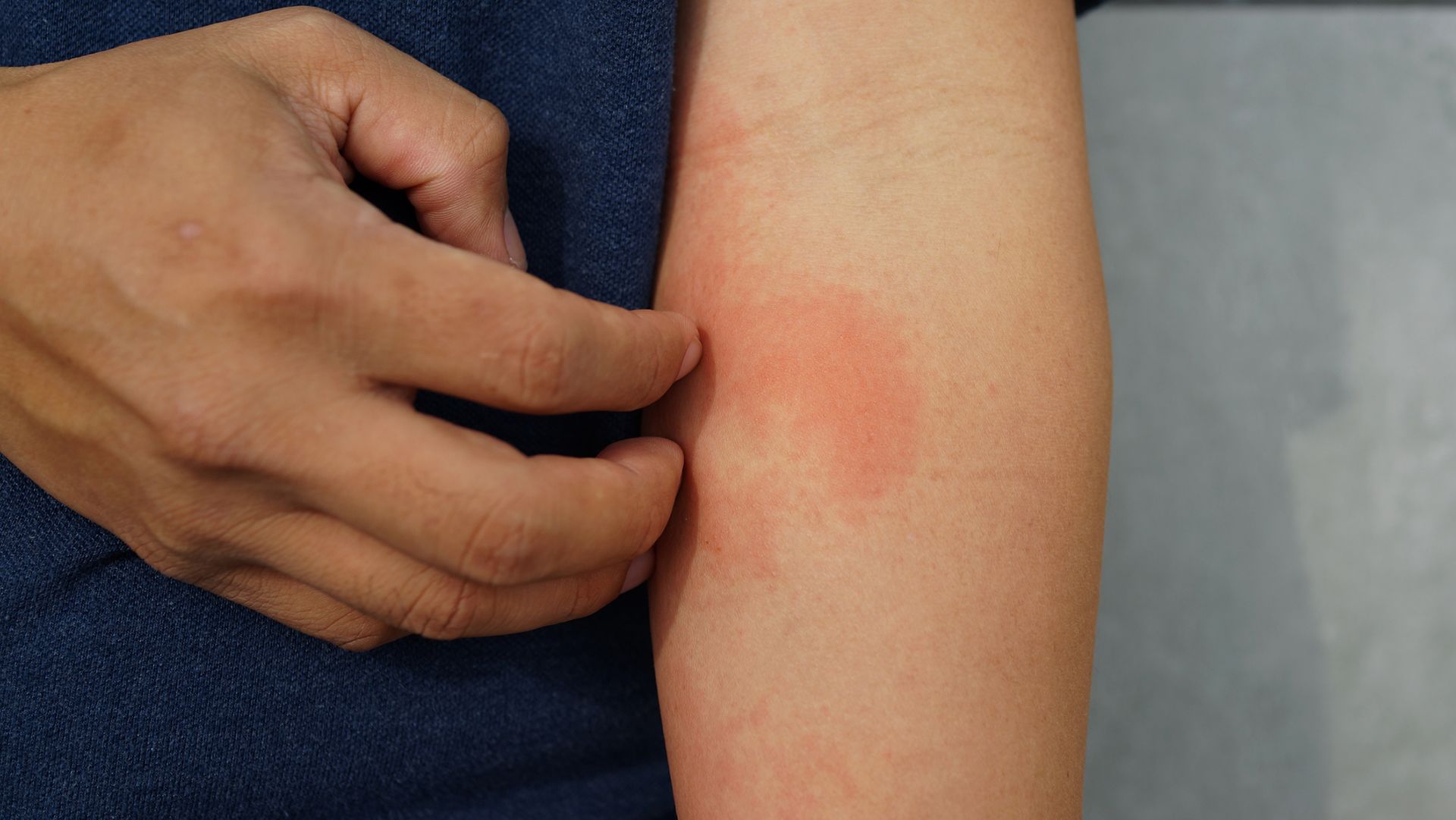
article
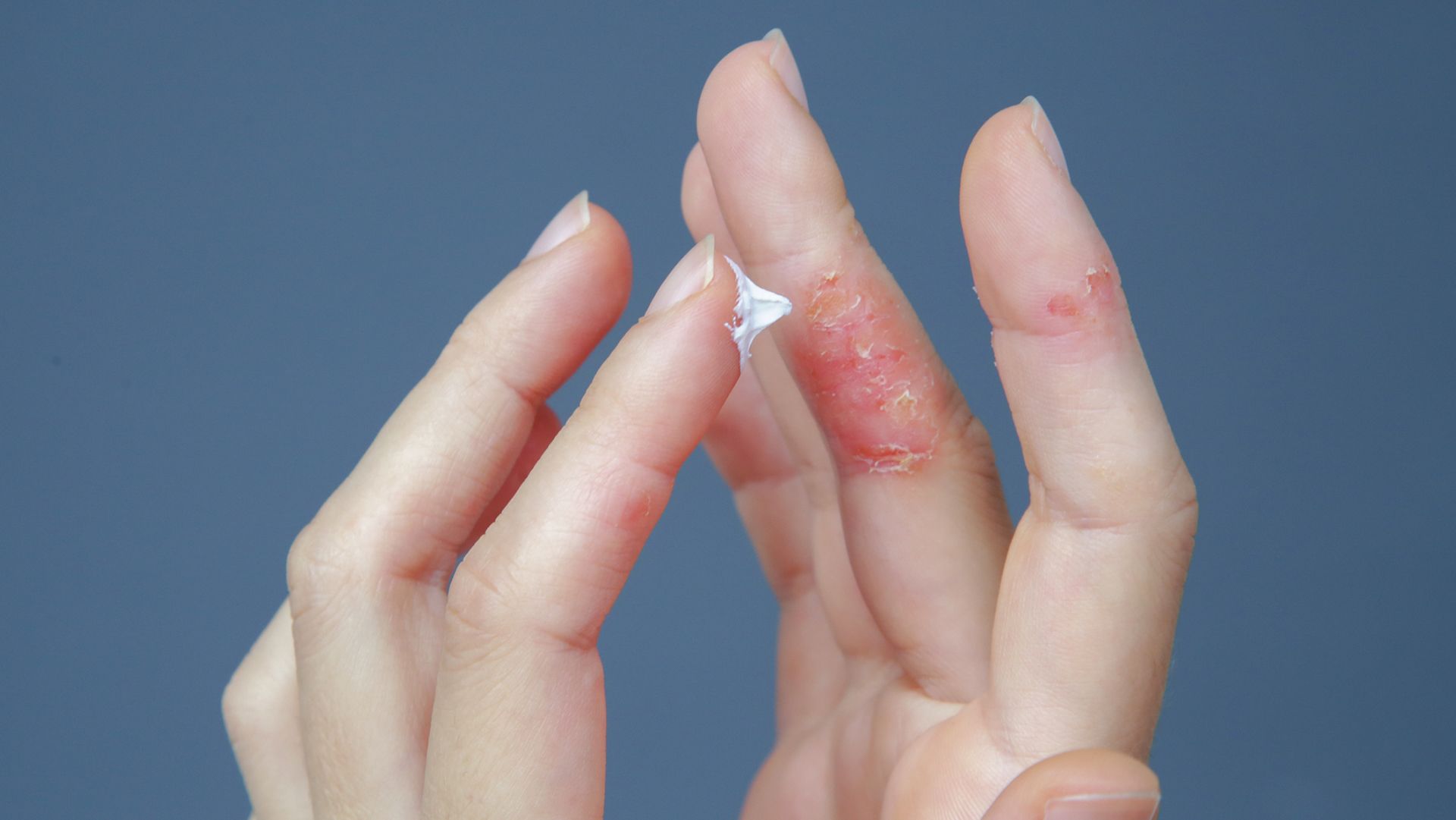
article
