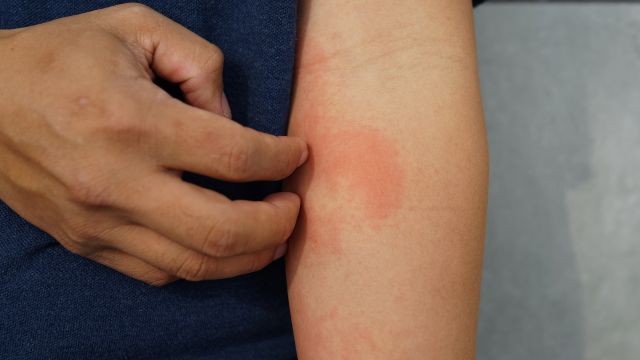
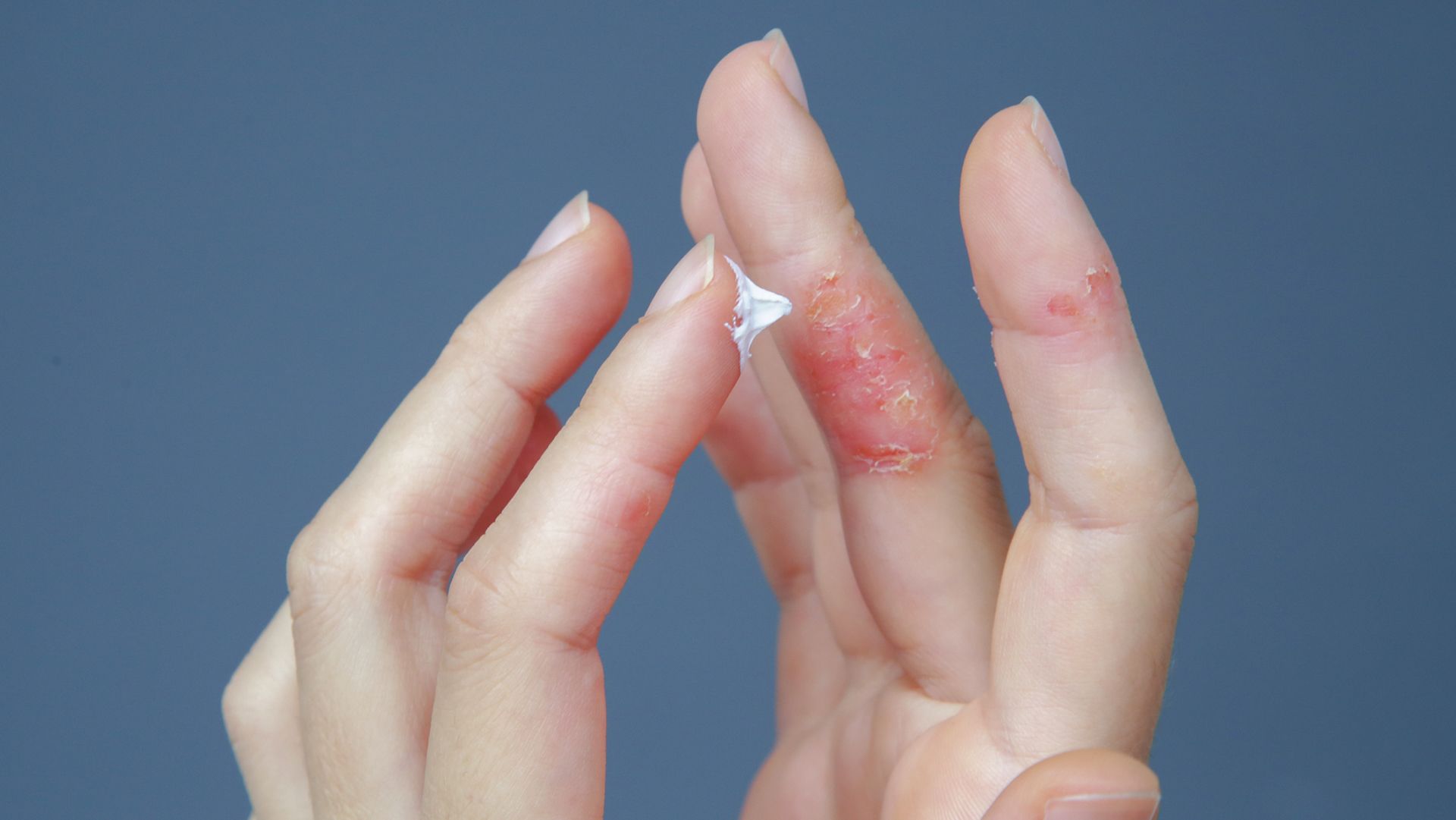
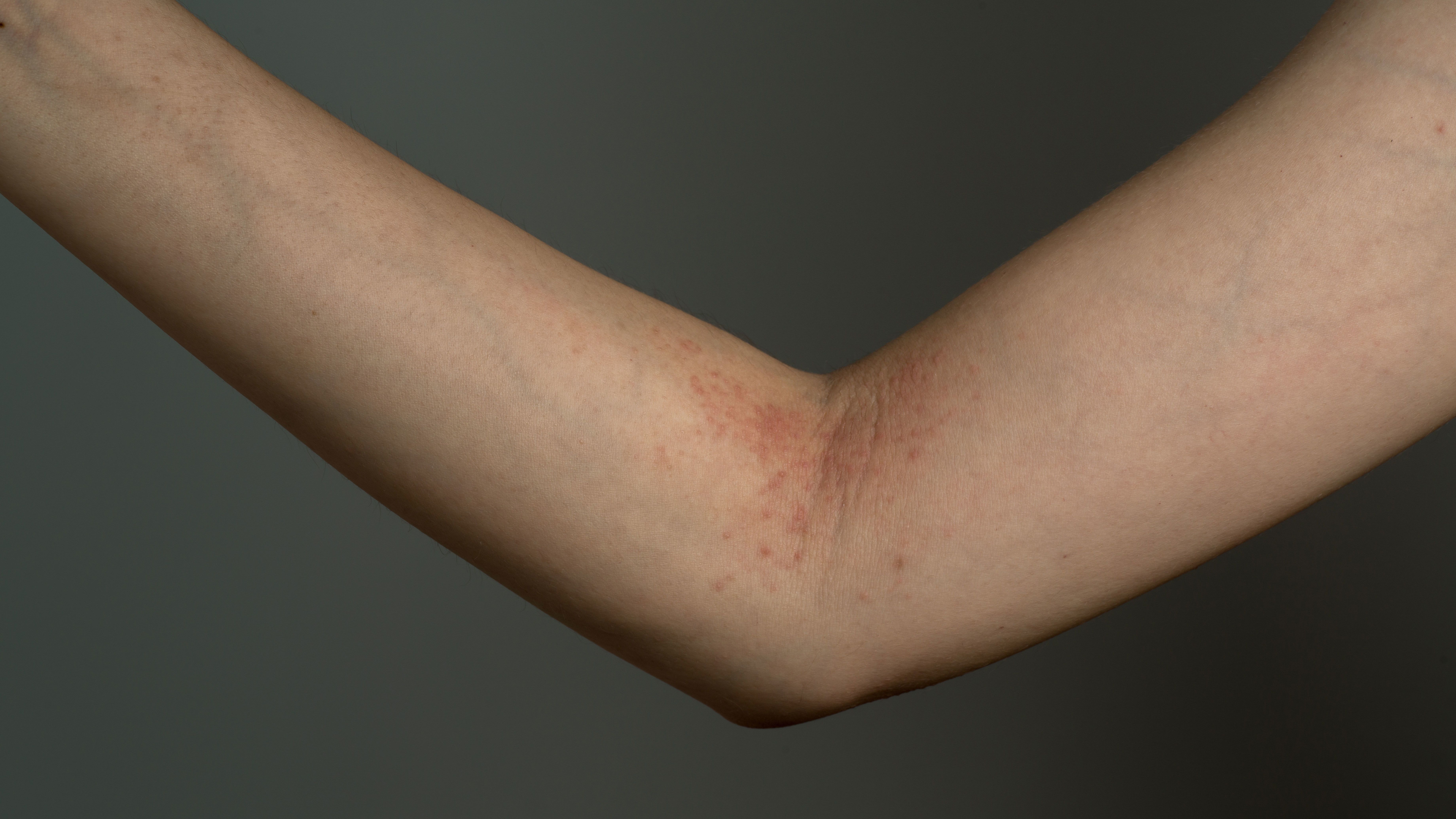
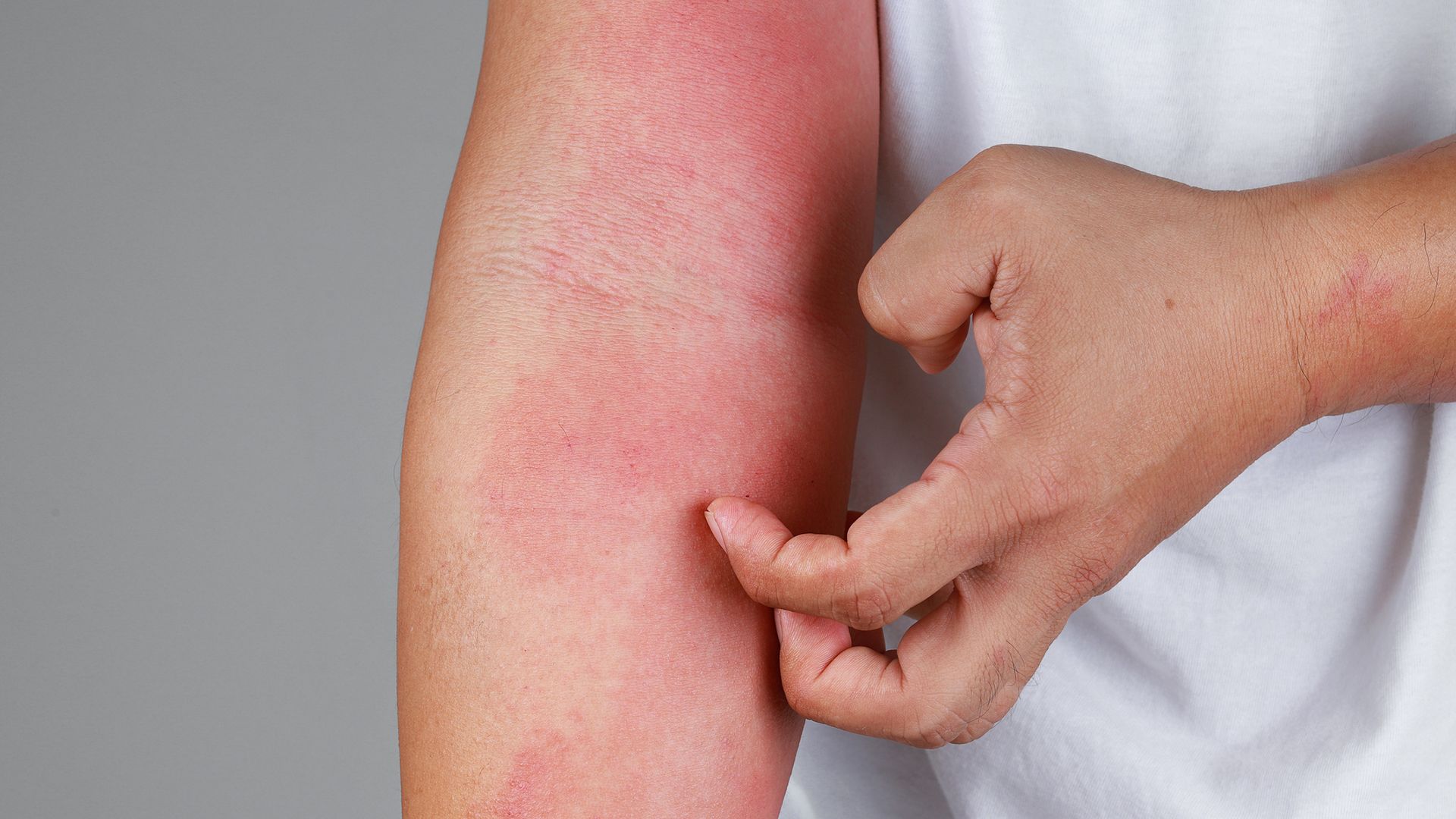
Atopic dermatitis (AD) is a chronic, inflammatory skin disorder that causes dry, itchy, scaly patches on the skin. It is the most common form of eczema and is sometimes referred to as atopic eczema.
AD is a condition that looks different for everyone. It often occurs in people who have asthma and/or allergies, but not all people with AD are diagnosed with these conditions. For many people, the condition begins during infancy or childhood—for others, it begins later in life.
If you are living with AD, it’s important to spend time defining your experience with the condition. One important question you should answer—how severe are your symptoms? Determining the severity of AD is important for several reasons, including helping you and your healthcare provider decide on the best approach to treatment.
Assessing the severity of atopic dermatitis
There are two main components to determining the severity of AD—there are the symptoms your healthcare provider assesses during your exam, and there are the symptoms that you report to your healthcare provider. Some of the factors that you and your healthcare provider should consider when determining the severity of AD include:
- How much of your skin is affected? What areas are affected?
- What do the dry patches look like? Is the skin damaged or thicker in those areas?
- How severe is the itching and when does it occur? Does itching interfere with sleep?
- How are you treating AD and how are symptoms responding to treatment?
To put it simply—if you only have a few, occasionally itchy patches of skin, AD is probably mild. If you have multiple patches of skin that are always itchy—especially if that itch often feels intense—AD is probably moderate or moderate-to-severe.
Quality of life
One of the most important things to consider is how AD impacts your quality of life. Quality of life refers to how well you are able to function mentally, emotionally, and physically on a daily basis.
Health conditions often impact quality of life. For example, someone with atopic dermatitis may not be able to sleep because of nocturnal itching, may skip social events because they are embarrassed about their symptoms, or may feel stressed due to the uncertainty of when the next flare will occur.
Quality of life is something that should be discussed with any skin condition, as skin conditions have been shown to have a significant impact on mental health, emotional health, and social functioning. Quality of life is a major consideration when determining the severity of psoriasis, another chronic inflammatory skin disorder.
Consider how having AD affects your average day and how it has affected you over time. Some specific questions you may want to consider:
- Does it feel like you’re scratching all the time or only occasionally?
- Do other people notice how much you’re scratching?
- Do you feel self-conscious about showing your arms or legs in public?
- Do you ever feel depressed or anxious because of your condition?
- Do you ever avoid social interactions because of your condition?
- Do you have difficulty sleeping at night due to scratching?
Keeping a symptom journal can be very helpful when determining the impact AD is having on your quality of life. A symptom journal can be used to keep track of physical symptoms as well as how you feel, your emotions, and things you find difficult. It can also be useful for writing down your goals, recording how you feel about your treatment, and noting questions you want to discuss with your healthcare provider.