Updated on October 28, 2025.
In the past, hospitals sometimes encountered hard-to-treat bacterial infections that couldn’t easily be resolved with the use of standard antibiotics. These infections tended to crop up in patients who had been in the hospital for long periods of time, who were older and more sick, and who were already taking a long list of medications.
When infections like these originate during a hospital stay, they are called “hospital acquired.” When they emerge in everyday settings—such as in public places or even in people’s homes—they’re called “community acquired.”
While any potentially dangerous bacterial infection is a cause for concern, experts have become especially worried about a rise in community acquired infections, particularly those caused by bacteria known as MRSA. In the case of MRSA, anyone—even otherwise healthy people—can be infected by this antibiotic-resistant “superbug.”
What is MRSA?
MRSA is an acronym for methicillin-resistant Staphylococcus aureus. That means it’s a type of bacteria (called Staphylococcus aureus) that doesn’t die when it is exposed to methicillin and other standard antibiotics once used to treat it. This ability to withstand antibiotic treatment is called resistance.
The Staphylococcus (aka, staph) bacterium itself is very common and can be found living harmlessly on the skin or in the nose of about a third of all people. About two out of 100 people, meanwhile, have MRSA on their bodies. People who have bacteria on their bodies without active infection are called carriers.
When staph does cause infection, the infection can become severe and in some of those cases it resists the germ-fighting effects of antibiotics.
What makes MRSA dangerous?
The community-acquired form of MRSA (CA-MRSA) usually causes infections of the skin. In people who have weakened immune systems, MRSA can spread to the bloodstream and other organs, but in most otherwise healthy people, it will remain a skin infection.
Since MRSA is resistant to typical first-line antibiotics, healthcare providers (HCPs) have to use more advanced antibiotics to treat the infection. This can cause problems beyond those posed by the infection itself because these medications have more side effects, may not be safe in pregnant or very young people, or because they can interact with other medications someone may be taking.
What are signs of a MRSA infection?
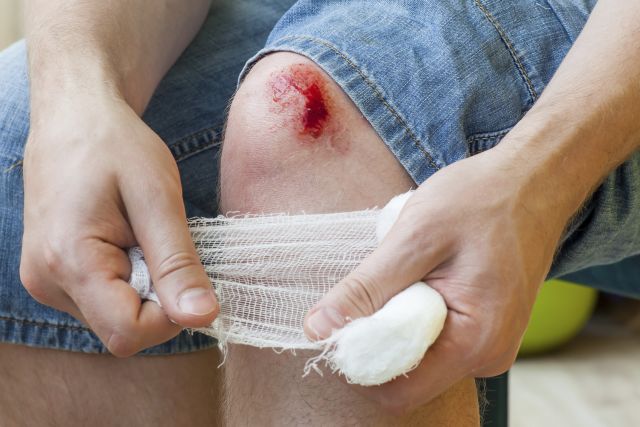
MRSA skin infections look like red or discolored swollen bumps. They could be painful, warm to the touch, and may be full of pus. If there is any sign of an abscess (such as swelling beneath the skin), pus or drainage, or if the person also has a fever, these are strong signs it might be MRSA.
Many people who visit their HCP with MRSA symptoms think they’ve had a spider bite. But unless they actually saw a spider biting them, it’s likely a MRSA infection. That said, it’s not possible to diagnose MRSA just by looking. An HCP can perform tests to confirm a suspected case.
How do you get MRSA?
MRSA is passed by direct contact. If a person has a scrape or an open wound and they touch someone who has the infection, it can be passed to them. Likewise, an item an infected person has used (such as a towel or razor) can spread the bacteria.
About 5 percent of people in hospitals are “carriers” of MRSA, meaning they have the bacteria on their skin. They usually don’t get sick from it, but they can unknowingly spread it.
Are some people at higher risk?
Certain groups are at higher risk of exposure to MRSA, mostly due to physical contact and sharing equipment. These include:
- Athletes who play contact sports: Athletic mats and locker rooms are two key areas of transmission
- Children in daycare centers: Kids often sit close together and share toys and other items.
- Anyone living in crowded conditions: These include military training camps and prisons.
Anyone who is hospitalized and gets inpatient medical care, or has surgery or medical devices implanted, is also at higher risk.
The opioid epidemic might also be connected to rising rates of community spread MRSA . People who use drugs that are injected are 16 times more likely get a severe staph infection like MRSA than people who do not inject drugs.
What can you do to prevent MRSA?
A few key preventive steps can help you minimize your risk of a MRSA infection:
- Wash your hands frequently. Remember to wash for 20 seconds. It’s also a good idea to bathe or shower immediately after any athletic activity.
- Keep any breaks to the skin (such as cuts, abrasions, and other injuries) covered, clean, and dry until they’re fully healed.
- Avoid sharing personal items with other people, especially ones that make direct contact with the skin, such as razors and towels.
What should you do if you think you have a MRSA infection?
If you notice the symptoms of a MRSA infection, immediately make an appointment with your HCP to be evaluated. In the meantime, don’t pick at the sores. Be sure to clean your hands often with soap and water and ask anyone you’re in close contact with to do so, too.
Antibiotics are still the mainstay of MRSA treatment, although HCPs have to be selective and strategic in deciding which medications to use. Meanwhile, researchers have been exploring ways to create vaccines for MRSA, but so far have not succeeded. More research is needed to develop a long-term remedy for MRSA.
Until then, you can go a long way toward protecting yourself by practicing good hand hygiene, refraining from sharing personal items, and seeking medical care promptly if you experience symptoms.