Since it was first identified in 1989, medical researchers and healthcare providers have learned much about the hepatitis C virus (HCV)—how to test for the virus, the risk factors that contribute to the spread of the virus, and effective medications that can cure chronic hep C infections.
But as much as we know, there are still unanswered questions, including how many people are living with a chronic hep C infection. The numbers we do have are only estimates—somewhere between 2.4 million and 4.7 million people in the United States, with at least 40 percent of those people unaware that they have an infection.
The Centers for Disease Control and Prevention (CDC) now recommends that everyone over the age of 18 get tested for hepatitis C at least once. The CDC recommends periodic testing for people who are at a higher risk. They also recommend a person get tested with every pregnancy.
If you are living with hep C or being treated for hep C, your firsthand experience with the virus puts you in a position to encourage others to get screened.
Here are a few things to discuss with people you know that might help encourage them to get screened for hep C.
Hep C is a “silent” disease
Chronic hep C is sometimes called a “silent” disease because most infections do not cause any noticeable symptoms. A person feels fine even though the virus and the immune system are battling against one another inside the liver—the virus replicates inside liver cells, the immune system attacks those infected cells, and the liver becomes damaged and scarred in the process.
Over time, this accumulated damage can cause serious, life-threatening complications—cirrhosis (permanent damage and scarring), liver failure, and liver cancer. These complications can take years or decades to develop, but once they do, treatment options are limited.
Early detection means early treatment
Because of the lack of symptoms, the only way for a person to know if they have hep C is to get screened—and this is one of the most compelling reasons to get screened and to encourage others to get screened.
The best way to prevent chronic hep C from causing serious long-term complications is to treat it as early as possible—and the first step to treatment is getting screened. The current treatments for hep C are very effective and can cure infections in over 90 percent of cases.
Screening reduces stigma
Stigma refers to the negative, discriminatory attitudes that are unfairly directed against certain individuals. Many people with hep C face stigma. They find themselves blamed or judged for having the infection. They are treated as being highly contagious.
These kinds of stigmas prevent people from getting screened for hep C. For example, a person who is at higher risk of hep C may avoid getting screened, fearing this kind of judgement from others if they have hep C.
For another example, a person who is at relatively low risk may avoid getting tested, not wanting to be associated with people who have hep C or thinking that their risk of having hep C is nonexistent (it’s not).
More people getting screened helps reduce the stigma around screening—hopefully, screening can be a normal part of routine preventive healthcare, with no associated judgement.
Where to get screened
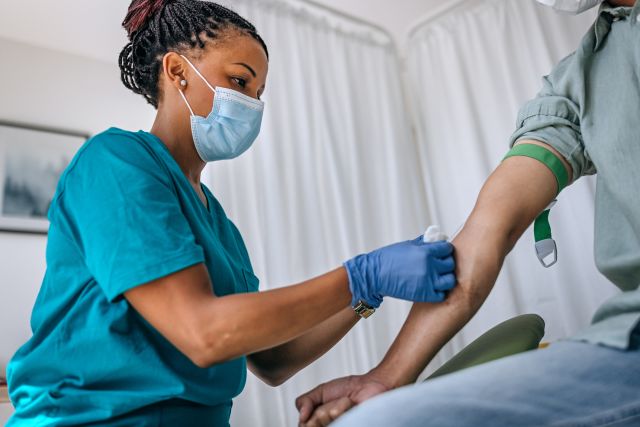
The initial screening for hep C involves a blood test that can be performed by a primary care provider. If you do not have a healthcare provider, you can search for confidential no-cost/low-cost testing in your area using the CDC’s GetTested website (gettested.cdc.gov).
If you are being treated for hep C, talk to your healthcare provider about places to access screening—this can be useful information to have on hand for other people.