7 Mammogram Myths You May Hear
Let’s set the record straight on how mammograms work, when you should get one, and what to expect.
Updated on April 30, 2024

While it remains the second deadliest cancer among American women, the rate of breast cancer deaths has dropped dramatically—almost 40 percent—since 1989. A combination of factors including increased awareness, advances in medical treatment, and the widespread use of screening mammograms, are likely responsible for this encouraging trend.
When people get regular mammograms, the screenings help identify nearly four out of five cases of breast cancer, sometimes years before the tumor would be detectable by touch alone. Yet, despite their strong track record, regular screenings are often skipped due to misunderstandings about how they work, how much they cost, or why and when they’re needed.
“There are still a lot of misconceptions out there,” says Paula Y. Rosenblatt, MD, a medical oncologist at the University of Maryland Greenebaum Comprehensive Cancer Center in Baltimore. “But I think better breast awareness and understanding has helped the situation.”
Here are the biggest breast-screening myths, along with the facts to dispel them.

MYTH: You Don’t Need A Mammogram Unless You Feel A Lump
While any lump or change in the feeling of your breast should be evaluated by a doctor, breast cancer could actually be growing for years before you’re able to feel it. That’s why having regular mammograms is so important: They can help find, diagnose, and treat cancer before signs are more evident. “A vast majority of breast cancers are now detected without any symptoms,” says Dr. Rosenblatt.
Research has found that discovering breast cancer early, before it advances, can increase quality of life and chances of survival. Between 2009 and 2015, the five-year survival rate for localized breast cancer—cancer that hasn’t extended beyond the breast—was about 99 percent, according to the National Cancer Institute. When the cancer was classified as distant, meaning it spread to other parts of the body such as the liver and lungs, the five-year survival rate dropped to 29 percent.

MYTH: Physical Breast Exams Are Just As Good As Mammograms
Studies have found no significant benefit to physical breast exams for detecting cancer, including clinical exams done by healthcare providers (HCPs) and self-exams performed at home. In fact, the U.S. Preventive Services Task Force (USPSTF) recommends that HCPs refrain from teaching patients how to do self-exams.
Mammograms, instead, are much more reliable for finding the disease. “We know from studies that mammograms can pick up significantly earlier, smaller cancers, and that improves outcomes,” Rosenblatt says.
While you should never use a physical exam in place of mammogram, you should become familiar with the normal appearance and feel of your breasts. This way, you can recognize sudden changes and bring them up with your HCP as soon as possible.

MYTH: Every Woman Should Have Yearly Mammograms Starting At 40
Most HCPs and health organizations now advise starting (or at least considering starting) screening mammograms at 40. The timing of how often to get them, however, remains up for debate. Recommendations from major organizations for women at average risk for breast cancer include the following:
- The USPSTF recommends that women between the ages of 40 and 74 get a mammogram every other year.
- The American College of Obstetricians and Gynecologists (ACOG) advises that HCPs offer mammography to women starting at age 40. But from then until age 49, they say it’s the individual’s choice whether or not to be screened. By age 50, however, ACOG recommends getting a mammogram every one or two years.
- The American Cancer Society recommends women have annual mammograms from age 45 to 54; they can switch to every two years after that. From 40 to 44, it’s a personal decision.
- The American College of Radiology and National Comprehensive Cancer Network recommend every woman begin yearly screenings at age 40.
Women at higher risk should always confer with their HCP, as they may need to begin mammograms earlier and be screened more frequently. Your HCP can use several assessment tools to help determine if you’re in this category.

MYTH: Mammograms Always Hurt
It’s true that having your breasts compressed during a mammogram may feel uncomfortable. “Some patients do experience some mild discomfort,” confirms Rosenblatt.
But the pressure on each breast is very brief—only long enough to take quick images—and many people recount the feeling as temporarily unpleasant, rather than outright painful. (If the compression does become too much to bear, alert your technician.)
Worried about potential soreness? Try to avoid scheduling your appointment when your breasts are tender, like in the days before or during your period. Rosenblatt suggests that taking an over-the-counter pain reliever could help, as long it’s safe for you. And if it’s your first mammogram, she recommends asking the technician to walk you through the process, “because the stress and tension also makes it more uncomfortable for patients.”
In addition, there are new types of mammogram machines that are curved more like the shape of the breast and may be more comfortable for you—call radiology centers in your area to see which one may offer this option.

MYTH: Mammogram Radiation Causes Cancer
Since mammograms involve X-rays, they expose you to some radiation, but the amount is strictly regulated and “remarkably low,” says Rosenblatt. It’s similar to what you receive from the environment in about seven weeks.
What’s more, the potentially lifesaving benefits of detecting breast cancer early through mammograms far outweigh the minimal risks of low-dose radiation exposure.
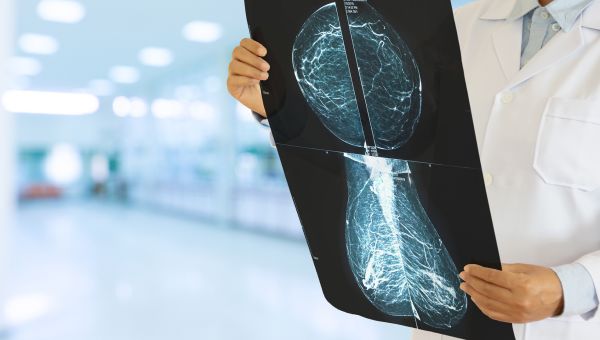
MYTH: Callbacks Mean You Have Cancer
Maybe the first images weren’t clear enough. Maybe your breast tissue is denser than average. Maybe part of your X-ray just looks a little different from the rest. Whatever the issue, if your imaging team needs another look at your breasts, they will call you back into the radiology center.
It’s estimated that up to 16 percent of women who undergo their first mammogram are called back for more testing, for various reasons. The rate is higher for pre-menopausal women. A 2016 review in JAMA suggests that more than half of women who have annual mammograms will get a call back at least once in their lifetime.
The additional assessment could involve a diagnostic mammogram—in which further images are taken—or an additional screening, such as an MRI or an ultrasound. Some people will need a biopsy, or a tissue sample, for further analysis. The good news is that more than 9 out of 10 times, people who are called back for a second look are cancer-free.
Waiting for any medical test results can be nerve-wracking, but it’s important to remember that callbacks are common —and so are anxious feelings about them. Call your HCP or the American Cancer Society at 1-800-227-2345 if you have questions or need support.

MYTH: Mammograms Are Too Expensive
If you have health insurance, you should be able to get a mammogram at no cost to you. For women over 40, the Affordable Care Act requires private plans and state Medicaid expansions to cover screening mammograms every 1 to 2 years—no copayment or coinsurance necessary. Medicare pays for annual screening mammograms, as well.
Before scheduling your mammogram, contact your insurance company to find out what exactly they will cover; some newer 3D mammograms may not be included in your coverage, for example. It’s also important to note that screening mammograms are different from diagnostic mammograms (prescribed after a lump or other symptom is found), which may not be fully covered.
If you don’t have health insurance, organizations such as the National Breast Cancer Foundation, the National Breast and Cervical Cancer Early Detection Program and the Susan G. Komen Foundation frequently partner with local imaging centers to provide free and low-cost screenings to eligible people. Visit their websites or speak with a facility representative for more information.
Regular mammograms can help find early-stage breast cancer, when the treatment may be less intense and less expensive than for cancer at a later stage. Getting regular screenings could save money, time, anxiety—and your life.

American Cancer Society. Survival Rates for Breast Cancer. Last revised March 1, 2022.
American Cancer Society. Understanding Radiation Risk from Imaging Tests. Published August 3, 2018.
Miller D, Livingstone V, Herbison P. Interventions for relieving the pain and discomfort of screening mammography. Cochrane Database Syst Rev. 2008;(1):CD002942.
American College of Radiology. Guidelines Start at 40. Published 2019.
American College of Obstetricians and Gynecologists. Mammography and Other Screening Tests for Breast Problems. Published 2020.
American Cancer Society. Breast Cancer Facts & Figures 2019-2020. Atlanta, GA: American Cancer Society, Inc.; 2019.
U.S. Preventive Services Task Force. Final Recommendation Statement. Breast Cancer: Screening. April 30, 2024.
More On


video

article

slideshow

video


video
