When you’ve been diagnosed with cancer, you may feel like you’re all alone—but you’re not. You’ll have a team of healthcare providers (HCPs) dedicated to helping you get better. Still, there might be some scary moments, one of which could be your first radiation treatment session.
We spoke with Brandon Mancini, MD, a radiation oncologist with Mercy Health Saint Mary’s in Grand Rapids, Michigan, to demystify radiation and give tips on what to expect from your sessions.
Types of radiation
You might have questions about which radiation therapy you'll need, as well as how it works. There are three main kinds:
- The most common type, external beam radiation uses high-powered x-rays to kill or slow the growth of cancer cells. It's used to treat a large number of cancers, such as breast cancer, head and neck cancers, lung cancer and melanoma, among others.
- Brachytherapy kills cancer cells from inside the body using radioactive devices implanted near the tumor. It’s most commonly used for reproductive system cancers in women and prostate cancer in men.
- Systemic radiation uses radioactive drugs to kill cancer cells. It’s generally used for thyroid cancers, liver cancers, and bone cancers arising from metastatic prostate cancer.
Most types of radiation require multiple sessions, and may need weeks or even months to complete treatment.
Before your first session
If you're having external beam radiation—the most-used radiation treatment—you probably won’t jump right into it. “We usually meet with a patient initially to talk about the treatment recommendations,” says Mancini. “If it’s indicated, they’ll come back for a simulation.” That means the HCPs will do a trial run of the treatment, including marking your skin precisely where the x-rays will fall.
At the simulation, staff may also fit you for an immobilization device. “The purpose is to make sure the patient is in the exact same position for every treatment,” says Mancini. Head and neck cancers usually require a tight-fitting mask. Other kinds, such as lung or prostate cancer, may use cushions, restraints or a fitted vacuum bag to keep you in place.
Before your first external beam treatment, your HCP will also give you a list of do’s and don’ts. This will probably include specific soaps to use, and ask you to avoid deodorant with aluminum and zinc, says Mancini. If you’re being treated for stomach or esophageal cancer, you’ll likely want to avoid eating two to three hours before treatment.
The first treatment
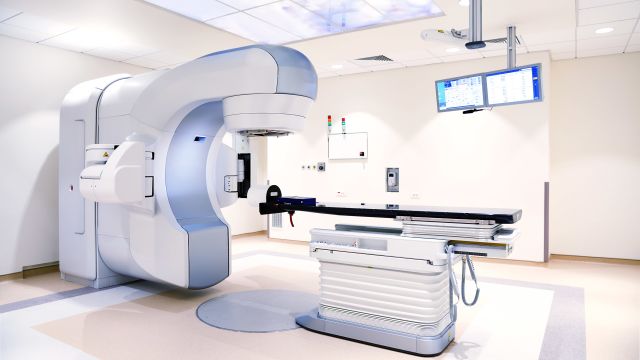
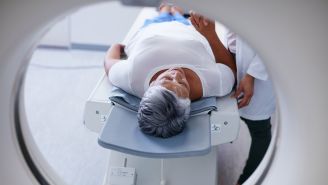
In most external beam radiation cases, you’ll be lying on your back on a table. “The typical machine is called a linear accelerator,” says Mancini. “It’s a machine with a treatment arm that rotates around the patient.” It’s not enclosed like an MRI machine, so most people don’t have to worry about triggering claustrophobia. Some facilities have a different machine called a tomotherapy unit. “It’s like a donut that the patient is slowly moving through, like a CAT scan,” Mancini says.
External beam radiation doesn’t take long. “The actual setup and treatment is usually less than 10 minutes,” says Mancini. “You’ll probably be at the facility for 30 to 40 minutes a day, five days a week.” Brachytherapy varies: you may need treatment every day for one to five weeks, you may be in the hospital for a week receiving low-dose radiation, or—in the case of a permanent implant—you may only need one treatment. Each systemic radiation session can require a hospital stay for two or three days.
For women with early-stage breast cancer who have had a lumpectomy, research shows a three-week radiation regimen is just as effective as a longer, five-week treatment course. However, a 2017 analysis of 4,225 women over 50 with early-stage breast cancer discovered that only 48 percent of patients receive the shorter regimen. If you have breast cancer and are a candidate for radiation, speak to your doctor about the length of your treatment.
The big question
Many people will begin radiation therapy with some preconceived notions. “The most common misconception of radiation therapy is that it will be painful from the start,” says Mancini. “We tell patients that they shouldn’t feel different before and after any given treatment.” But radiation is cumulative, he adds. “You’ll have minimal side effects for the first two weeks, but side effects slowly come on and slowly resolve.”
Side effects of radiation
Unless you’re getting treatment on your scalp, external beam radiation won’t make your hair fall out—that’s a side effect of chemotherapy. Side effects for external beam radiation usually involve skin irritation and fatigue. “Radiation is a temporary insult to the body,” says Mancini about fatigue. “It’s something the body has to respond to and use energy to recover from.”
Additional side effects depend on what area of the body is being treated. “If your treatment is to the abdomen you might have nausea, vomiting or diarrhea,” Mancini says. “When the bowel gets irritated, it responds by producing stool at a faster rate. The bladder does the same with urine.”
Brachytherapy implants and systemic radiation side effects are a bit different. Because the substances used in these are radioactive, you might actually become slightly radioactive while you’re being treated. The radioactivity doesn’t last long, but you may need to limit contact with other people for a few days or weeks.
Mancini wants people who need radiation therapy to know that each experience is unique—and that HCPs have become more skilled in controlling and managing side effects in the last 10 years. “Patients may have had family members or friends go through radiation, and may think their own experience will be similar,” he says. “But each experience has its own set of side effects and ways to manage them.”