9 keys to preventing and treating diabetic foot issues
Being proactive can help keep your feet healthy.
Updated on October 1, 2022

If you have diabetes, you probably know to be on the lookout for issues with your feet. Foot problems happen most often when there is nerve damage, also known as peripheral neuropathy. Nerve damage can cause tingling, painful burning or weakness in the foot.
Conversely, neuropathy can also cause numbness, so you may injure a foot and not even know it. In fact, up to half of all cases of diabetic peripheral neuropathy may come with no symptoms, which makes it all the more important to keep tabs on your feet as part of your regular routine. Poor blood flow or changes in the shape of your feet or toes may also play a role in foot-related complications.
But even if you’re experiencing these issues, you can still go a long way toward preventing serious complications from diabetes. Your best defense is a good offense. Here’s what you need to know about preventing and treating foot problems if you have diabetes.
Medically reviewed in February 2021.

Hit your blood glucose targets
It’s ideal, of course, to try to stave off foot problems before they happen. You can start by carefully monitoring your blood glucose levels. Poor glycemic control raises your risk of foot ulcers and infections. That’s because high blood glucose affects the nerves throughout your body and damages blood vessels, making it hard to fight infection.

Check your feet every day
Since nerve damage can reduce your ability to feel pain, heat and cold, you may not even be aware of a foot injury. For instance, you could have something like a pebble in your shoe and walk on it all day without feeling it. A blister or sore could form, raising your risk of infection.
Make a daily habit of checking for calluses, blisters and dry, cracked skin, as well as redness and swelling. Be sure to report these issues to your health care team as soon as you spot them.
Can’t see the bottom of your feet? Ask a friend or family member to help. Better yet, place a mirror on the floor and hold your feet above it to check for trouble spots. To make sure you remember to check, give yourself a can’t-miss reminder. Put something in your shoes or socks that must be removed—a tennis ball, for instance—before you put them on each day.

Pamper your feet
Diabetes can cause changes to the skin on your feet. That’s because the nerves that control oil and moisture in your feet may no longer work. As a result, your feet may become extremely dry. To avoid peeling or cracked skin, it’s important to moisturize.
After bathing, dry your feet thoroughly, then apply a thick moisturizer—an unscented hand cream or a thin coat of plain petroleum jelly, for instance. Be sure, however, to avoid putting any cream between your toes. Those dark, moist areas lend themselves to infection.

Protect your feet
To avoid sores, don’t go barefoot or wear shoes that are tight or rub against your feet. Ideally, there should be just enough room to wiggle your toes.
If you have diabetes, you may notice that your feet are more prone to calluses. Those rough areas are a result of the presence of high-pressure areas under the foot. If you have too much callus, severe nerve damage or foot abnormalities like hammertoes or bunions, your doctor may suggest specialized therapeutic footwear or inserts. Depending on the severity of your symptoms, you may be okay wearing well-fitted walking shoes or athletic shoes that cushion the feet and redistribute pressure. If not, the American Diabetes Association (ADA) recommends custom-molded shoes.
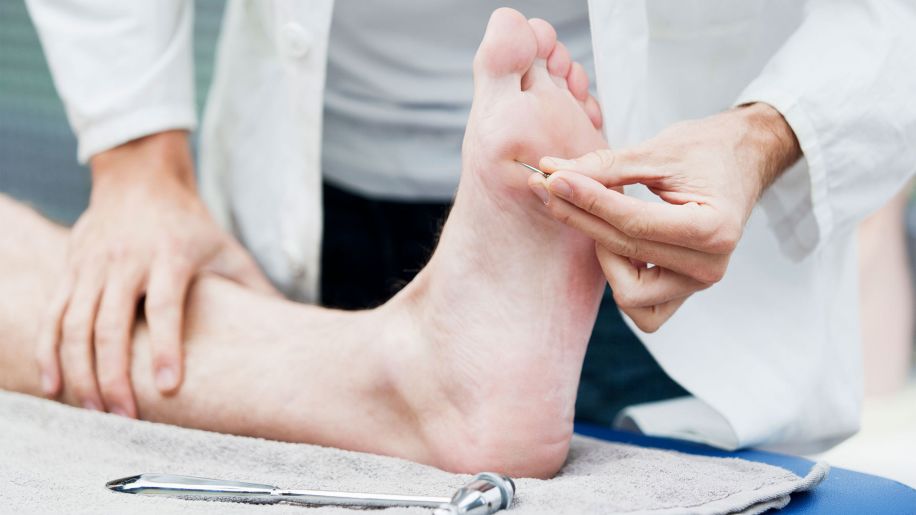
Have your doctor examine your feet
If you have diabetes, your health care provider should check your feet at every visit. Your doctor should also do a comprehensive foot exam at least once a year, according to the ADA. And, particularly if you are seeing a new doctor, be sure to bring your medical records to your appointment.
Among other things, your doctor will want to know about any history of foot ulcers, amputation, Charcot foot (a condition that causes bones to weaken), cigarette smoking, impaired vision and kidney disease. All of these things raise your risk for diabetic foot disease.
As for the exam itself, your doctor will inspect your feet and toes and do a sensory foot examination, which uses pinprick, temperature, vibration or a filament like a hairbrush bristle to check for diabetic peripheral neuropathy. Your doctor will also perform a vascular assessment, which involves using pulses in the legs and feet to evaluate the blood flow to your feet.

Keep your nails trimmed
It’s important to keep your toenails in good shape. After washing and drying your feet (which helps soften the nails), use toenail clippers to trim your nails straight across, then smooth away any sharp edges with an emery board or nail file. Avoid cutting into the skin near the corners of the nail, and don’t cut your nails shorter than the ends of toes—this helps prevent the nails from growing into your skin.
Can’t reach or feel your feet? Ask your doctor for help with trimming your nails. You may also need professional help if your nails are especially thick or if they have grown into the skin.
You may be tempted to have a pedicure but check with your doctor first to make sure it’s safe to do so. If you do get the green light, you’ll likely need to bring your own clipping tools to lower your risk of getting an infection at the salon.
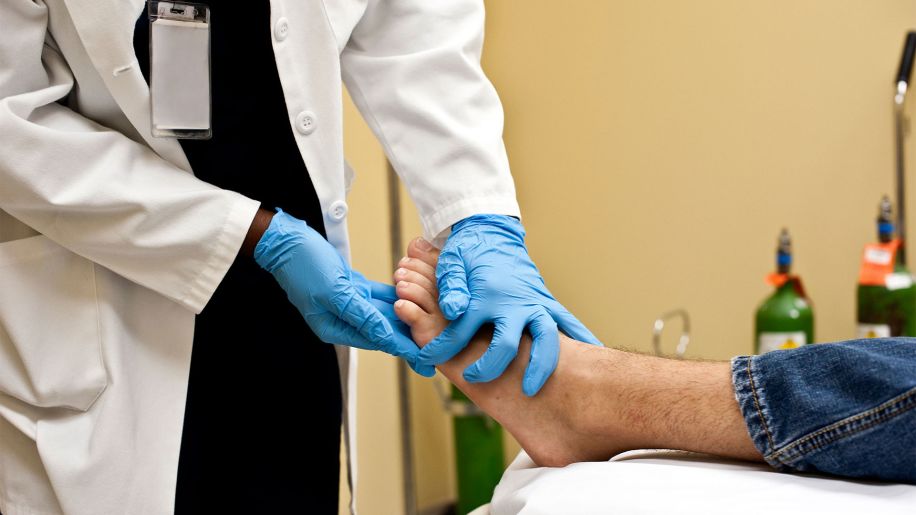
See your doctor about injuries
If you detect any foot issues, it’s important to act on them quickly and bring anything unusual to the attention of your health care provider. If you have a cut, blister, or wound on your foot that isn’t healing, don’t try to wait it out or treat it yourself with an over-the-counter antibiotic. Instead, see your doctor.
Depending on the severity, he may tend to it himself or refer you to a foot-care specialist such as a podiatrist, orthopedic or vascular surgeon or a rehab expert.
Likewise, if you smoke or have a history of lower-extremity complications, loss of protective sensation, changes in the shape of your feet (due to hammertoes or bunions) or peripheral arterial disease, he’ll recommend you see a specialist for ongoing care.

Wear therapeutic shoes
Nerve damage can lead to changes in the shape of your feet and toes. Rather than force your feet into a pair of regular shoes, talk to your health care provider about wearing those designed for people with diabetic foot disease. The ADA recommends shoes with a broad, square toe box, three or four shoelace holes on each side, a padded tongue, lightweight materials and a cushioned insole.
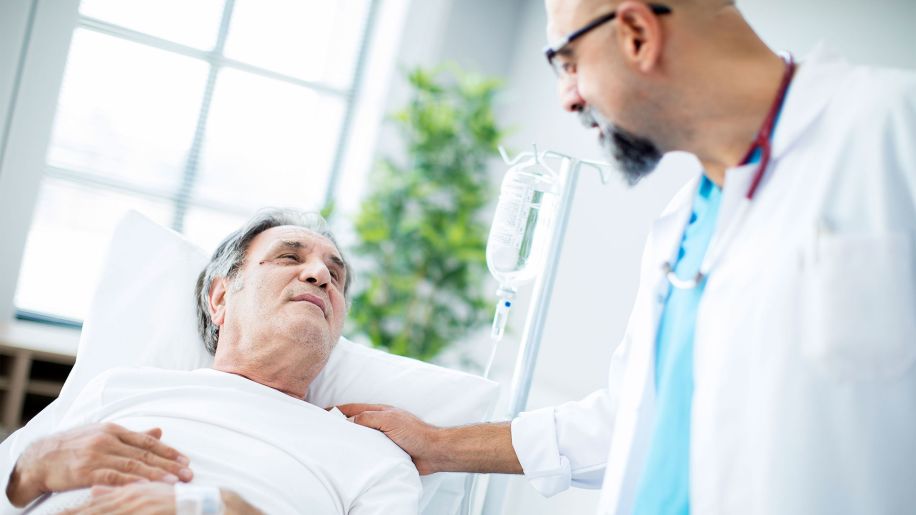
Treat severe foot issues as necessary
People with diabetes are more likely to have a foot or leg amputated than people who don’t have the condition. In fact, up to 75 percent of lower-limb amputations are performed on people with diabetic foot disease. That’s because diabetes raises your risk of what’s known as peripheral arterial disease, which reduces blood flow to the feet. People with diabetes are also prone to nerve disease, which reduces sensation. As a result, it’s easy to get ulcers and infections that may lead to amputation. Many people with diabetes who end up having amputations smoke. It is critical that you work on a quit smoking plan with your doctor.
The good news? Amputation is often avoidable if you follow your health care provider’s advice about managing your diabetes.
Featured Content

slideshow

slideshow

article
