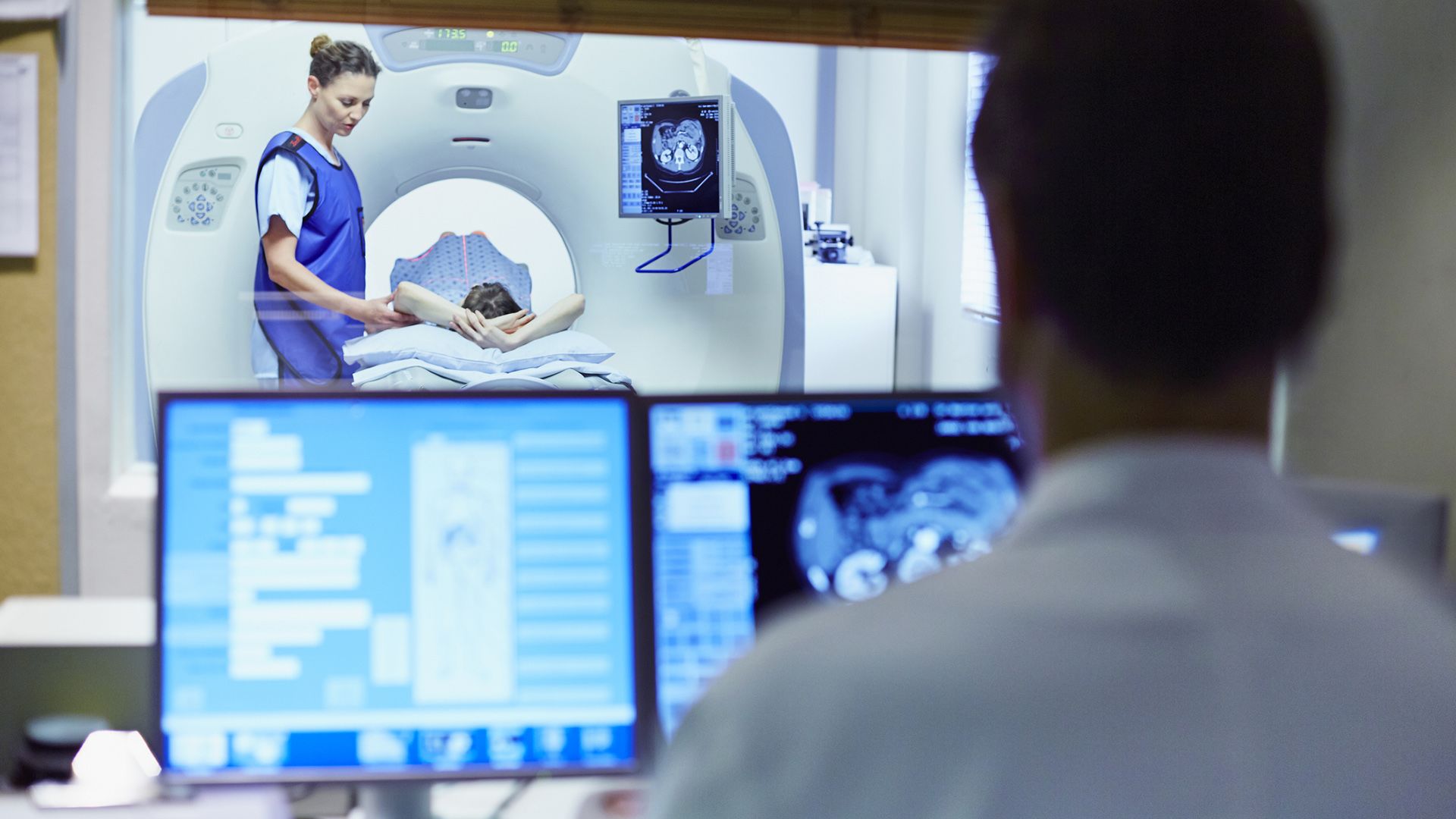
Being diagnosed with bladder cancer comes with a number of physical, emotional, and mental challenges. It is important to do everything you can to give yourself the best chance of success with your treatment.
The first step is to work with a healthcare team that understands the type of cancer and the treatment options. The choice of therapy will depend on a number of factors, including the type of cancer, the stage, and the patient’s medical history. A treatment plan may include surgery, chemotherapy, and/or radiation therapy. In some cases, newer treatments like immunotherapy and targeted therapy may be used.
In addition to working with your healthcare team, there are a number of lifestyle changes that are important after a bladder cancer diagnosis.
Quit smoking
If you smoke, talk to your healthcare provider about methods and strategies for quitting. Cigarette smoking puts a person at an increased risk for many different types of cancer (as well as other chronic illnesses) and is considered to be a major risk factor for bladder cancer.
If you are a smoker who has been diagnosed with bladder cancer, know that it is not too late to quit. Continuing to smoke increases the risk of recurrence, can make treatment side effects worse, and can make treatments less effective.
Eat well and exercise
Proper nutrition and regular exercise are cornerstones of both physical and mental health—and are habits that should be maintained or renewed after a cancer diagnosis. They are also topics that are important to discuss with a healthcare provider. Cancer and cancer treatments can impact energy levels, nutritional requirements, and a person’s ability to eat.
Ask your healthcare providers what foods you should be eating. Some healthcare teams also include a dietitian or nutritionist who can help you put together an eating plan. Also ask your healthcare provider about how to safely begin or continue an exercise program.
Look after your mental health
The emotional and mental challenges that accompany bladder cancer can be significant. While everyone handles a cancer diagnosis differently, a significant number of people with bladder cancer report feelings of distress, anxiety, depression, anger, and negative body image. Some patients may experience these feelings at the time of diagnosis, others may experience them during or after treatment.
There are people who can help you work through these challenges. The first step is talking to your healthcare team about the ways that cancer and cancer treatment have impacted your life and what you are feeling. Your healthcare providers may have recommendations that can help, such as therapies to ease troubling side effects or symptoms. For some patients, negative feelings may progress to mood disorders that require treatment with counseling or medication.
It can also help to take part in a support group. Support groups are organized gatherings for people who have shared a similar experience. There are support groups for bladder cancer patients that meet in person, as well as support groups that meet online.